Gene Therapy for Head and Neck Cancers
Despite advances in surgery, radiotherapy, and chemotherapy, survival of patients with squamous cell carcinoma of the head and neck has not significantly improved over the past 30 years. Locally recurrent or refractory disease is particularly difficult to treat. Repeat surgical resection and/or radiotherapy are often not possible, and long-term results for salvage chemotherapy are poor. Recent advances in gene therapy have been applied to recurrent squamous cell carcinoma of the head and neck. Many of these techniques are now in clinical trials and have shown some efficacy. This article discusses the techniques employed in gene therapy and summarizes the ongoing protocols that are currently being evaluated in clinical trials. [ONCOLOGY 15(3):303-314, 2001]
ABSTRACT: Despite advances in surgery, radiotherapy, and chemotherapy, survival of patients with squamous cell carcinoma of the head and neck has not significantly improved over the past 30 years. Locally recurrent or refractory disease is particularly difficult to treat. Repeat surgical resection and/or radiotherapy are often not possible, and long-term results for salvage chemotherapy are poor. Recent advances in gene therapy have been applied to recurrent squamous cell carcinoma of the head and neck. Many of these techniques are now in clinical trials and have shown some efficacy. This article discusses the techniques employed in gene therapy and summarizes the ongoing protocols that are currently being evaluated in clinical trials. [ONCOLOGY 15(3):303-314, 2001]
Introduction
Squamous cell carcinoma of the head and neck affects approximately 125,000 patients annually in developed countries worldwide. In the United States, an estimated 30,100 new cases will be identified in the year 2001, with 7,800 associated deaths.[1] Primary therapy for localized disease is surgery with or without adjuvant radiotherapy or radiotherapy alone. Despite advances in surgical resection, reconstruction, and adjuvant treatment, survival in these patients has not improved significantly over the past 30 years.[2]
Local and/or regional tumor recurrence develops in approximately one-third of patients following surgery.[3-6] In the majority of cases, disease recurs in the region of the original primary tumor and leads to severe morbidity due to pain, oropharyngeal dysfunction, and laryngeal obstruction, with resultant difficulties in swallowing and speech. Once the cancer has recurred and/or metastasized, the patient is often considered incurable. Conventional salvage treatment, including radiation therapy or surgery, is often difficult or disfiguring and offers little hope for long-term survival.
Several chemotherapeutic agents have been used in recurrent squamous cell carcinoma of the head and neck. Combination regimens with cisplatin (Platinol) and fluorouracil (5-FU) have induced responses in 32% to 47% of patients; however, this therapy can be toxic and shows no clear impact on survival.[7-12]
When recurrent squamous cell carcinoma of the head and neck becomes refractory to chemotherapy and/or radiation therapy, the median life expectancy is 3 months and the tumor response rate to second- or third-line chemotherapeutic agents is approximately 15%. Two-thirds of patients dying with this disease have no symptomatic distant metastases. Therefore, local and regional disease control is paramount, and there is an urgent need for more effective therapies for these terminally ill patients. Because of these considerations, much of the interest in treating squamous cell carcinoma of the head and neck currently lies in generating new and effective therapies such as gene therapy.
Gene therapy has the potential for targeting cancer cells while sparing normal tissues. These treatments are potentially useful for recurrent disease, as well as in the adjuvant setting (ie, at the resected margins). The purpose of this article is to describe the principles of gene therapy as they relate to head and neck cancer and to summarize the ongoing protocols that are currently being evaluated in clinical trials.
Principles of Gene Therapy
Gene therapy may be defined as the introduction of genetic material into a cell to modify cellular function.[13] The transfer is either in vivo (in which the gene is introduced into the body) or ex vivo (in which a tumor is removed, the genetic material is delivered, and the cells are then reintroduced into the patient). The ex vivo approach has not been utilized in head and neck cancer because superficial lesions of the head and neck usually lend themselves to direct injection of genetic material.
Genetic material is transferred via vectors that may be chemical, physical, or viral. The ideal vector would transfer an exact amount of genetic material into a specific area of each target cell, thereby allowing proper expression of the gene product without causing toxicity. Unfortunately, the ideal vector does not exist.
Chemical transfection introduces DNA with calcium phosphate, lipid, or protein complexes. Lipid vectors are a combination of plasmid DNA (pDNA) and a lipid solution that result in the formation of a liposome. This fuses with the cell membranes of a variety of cell types, passing the pDNA into the cytoplasm and nucleus, where it is transiently expressed. DNA/protein complexes can be more specific than liposomes by conjugating DNA with a tissue-specific ligand or antibody.[13] The DNA is thus internalized via receptor-mediated endocytosis. To prevent lysosomal DNA degradation, it is usually complexed to an endosome lysis agent.[13]
Physical transfection of genes is accomplished by electroporation, microinjection, and ballistic particles.[2] These have not been particularly useful in clinical trials as of yet. Currently, viral vectors are the most widely used method of genetic transfer.
Viruses in Gene Therapy
Viruses commonly used in gene therapies include retroviruses, adenoviruses, and herpesviruses.
Retroviruses: Retroviruses contain RNA genomes that undergo reverse transcription after infecting a cell, thereby producing double-stranded DNA. This DNA integrates in a stable, random fashion into the host genome, thus passing copies of the gene to all subsequent generations of cells. One limitation of retroviruses is that they can only infect actively dividing cells, leaving quiescent cells unaffected. As DNA is permanently inserted, this also raises long-term safety questions.
Adenoviruses: An adenovirus is a DNA virus that infects a cell, loses its protein coat, and transfers DNA into the nucleus, where it is transcribed. This DNA does not integrate into the host genome, and thus, its effects are transient (range: 7 to 42 days). Therefore, multiple administrations of the vector are usually required. The advantage of adenoviral vectors is that most cells are susceptible to infection, regardless of their position in the cell cycle. In addition, adenoviruses can be produced at a high titer-up to 1012 plaque-forming units-making their administration more efficient. As exposure to adenovirus is common, approximately 90% of humans have antibodies against the virus. Preexisting antibodies can limit the effectiveness of this strategy, particularly upon a second exposure to the vector.
TABLE 1

Summary of Commonly Used Vectors in Gene Therapy
Herpesviruses: Most herpesvirus vectors are developed from strains of herpes simplex virus type 1 (HSV-1). This is a double-stranded DNA virus that has several interesting properties, including the ability to remain latent in tissue and to be reactivated at the original site of infection. After infecting a cell, HSV-1 replicates within the cell, causing cell lysis and infection of surrounding cells. In addition, HSV-1 thymidine kinase (tk) is expressed during viral replication-a property that can be exploited to activate prodrugs, such as ganciclovir (Cytovene). In addition, HSV-1 is a common pathogen in humans and rarely causes significant illnesses. Table 1 summarizes the advantages and disadvantages of the various clinically significant vectors.
Gene Therapy Strategies
Potential uses of gene therapy in head and neck cancer include the treatment of recurrent disease and adjuvant treatment, for example, at a surgically resected margin. Localized distant metastatic disease is another potential target of gene therapy in patients with head and neck cancer.
Gene therapy is primarily limited by the need to directly inject the vector into a lesion. This makes head and neck cancer a particularly appropriate target, because most primary and recurrent lesions are accessible by needle. Intravenous methods of administration have been attempted in animal models; however, significant efficacy has not been demonstrated.
There are four main strategies in gene therapy:
(1) to restore a defective tumor-suppressor gene (replacement gene therapy);
(2) to enhance immune surveillance (immunotherapy);
(3) to activate prodrugs that have a chemotherapeutic effect ("suicide" gene therapy); and
(4) to introduce viruses that destroy tumor cells as part of the replication cycle.
What follows are detailed descriptions of these four treatment strategies as they are being studied in head and neck cancer.
Replacement Gene Therapy
Normal cells have the ability to regulate their cell cycles and eventually undergo programmed cell death (apoptosis). Cancer cells have lost the ability to regulate their cell cycles, largely due to mutations and overexpression of cell-cycle regulators.[14] Several genetic mutations have been described in head and neck cancer, including mutations of p53, the retinoblastoma gene (RB1), p16, and p21.[14] The most extensively studied mutations are those of p53.
p53 and Ad-p53: The p53 gene functions as a tumor-suppressor gene, responding to cell stress and DNA damage by activating other genes, inhibiting DNA synthesis, and inducing apoptosis.[15] Loss of p53 function leads to unregulated cellular proliferation. Inactivation or mutation of the p53 gene product occurs in approximately 70% of human solid tumors, including 45% to 70% in squamous cell carcinoma of the head and neck.[16-18] The basis of replacement gene therapy has focused on restoration of normal p53, which would restore the cell’s control of its cycle.
A genetically engineered type 5 adenovirus (Ad-p53) has been studied by Clayman et al.[15,19-21] This virus is replication-defective, with a cytomegalovirus-promoted, human wild-type p53 cDNA placed in the deleted E1 region of the vector.[20] In preclinical evaluations, this virus induced apoptosis in squamous cell carcinoma of the head and neck cell lines without significant effects on normal cell lines.[22,23] Ad-p53 also prevented the establishment of tumors after subcutaneous injection of squamous cell carcinoma of the head and neck cell lines in a nude mouse model.[22]
Phase I Trial of Ad-p53: A phase I clinical trial using Ad-p53 in 33 patients with locally recurrent squamous cell carcinoma of the head and neck consisted of patients with surgically unresectable disease and patients who subsequently underwent a resection.[20] Treatment consisted of intralesional injection three times a week for 2 weeks in the nonsurgical arm, and 1 week of treatment followed by an intraoperative and postoperative dose in the surgical arm. Injections were well tolerated, with injection site pain and fever being the most common side effects. Representative biopsy samples showed p53 transgene expression despite detectable antibodies to type 5 adenovirus in patients who received greater than 107 plaque-forming units of the virus.
In the nonsurgical arm, 2 of 17 patients exhibited a partial response to treatment, 6 patients had stable disease, 9 had progressive disease, and 1 was not evaluable. In the surgical arm of the study, 4 of 15 patients were alive with no evidence of disease at 11.5 to 29.1 months, 1 was alive with disease, 8 subsequently died of their disease, and 2 died of unrelated causes. The median disease-free interval was 3.9 months for the postsurgical patients in whom disease recurred.
Of note, the p53 status of the lesions in this study did not directly correlate with the antitumor effects from Ad-p53 treatment. It may be that other mechanisms of action besides p53 expression are involved in the response, such as antiangiogenic effects, host immune response, or local replication of the virus (thereby causing cell lysis).[20]
Phase II Trial of Ad-p53: An international phase II study is currently evaluating Ad-p53 in 170 patients. This study group is also considering the use of Ad-p53 as an adjuvant treatment. Future studies of Ad-p53 may combine the virus with traditional chemotherapeutic agents, since the response to such a combination was apparently augmented in a preclinical evaluation of lung cancer cell lines.[24]
Replacement of Other Genes: Studies are also ongoing regarding replacement of other commonly mutated genes in squamous cell carcinoma of the head and neck. In vitro and in vivo animal studies using an adenoviral vector with a p16 transgene have shown some efficacy.[25] A phase I clinical trial utilizing this approach is being organized at the Johns Hopkins Hospital.
Immunotherapy
The immunotherapeutic approach to head and neck cancer involves either increasing the immunogenic potential of tumor cells or augmenting the patient’s immune response to a tumor.[26] Patients with squamous cell carcinoma of the head and neck may have deficient function of natural killer cells, T lymphocytes, and cytokines.[14] Initial attempts to enhance the immune response with bacillus Calmette-Gurin, either alone or in combination with methotrexate, have shown minimal benefit.[27,28]
Interleukins: Cytokine enhancement of patient immune response has focused on interleukin-2 (IL-2; aldesleukin [Proleukin]). Produced by activated T lymphocytes, IL-2 stimulates both natural killer cells and T cells. When IL-2 is administered systemically, significant toxicity results.[29]
Intratumoral IL-2 has been used in squamous cell carcinoma of the head and neck with limited success.[30] Adenoviral-mediated IL-2 gene therapy has also been minimally successful, with no complete responses generated in animal models.[31,32]
Interleukin-12 (IL-12) is also a potent immunostimulatory agent. It is primarily produced by activated macrophages and acts synergistically with IL-2, as well as independently in stimulating natural killer cells, T cells, and cytokine release. Animal models using intratumoral IL-12 have demonstrated an antitumor effect that will be further evaluated in a phase I clinical trial in patients with recurrent squamous cell carcinoma of the head and neck.[33]
MHC Molecules: To avoid the toxicity associated with cytokines, attempts have been made to improve the surface expression of immunogenic antigens. Squamous cell carcinoma of the head and neck expresses a wide array of surface antigens to which T cells respond. In order for proteins to be properly recognized, antigens must be displayed by major histocompatability complex (MHC) class I and class II molecules. It is often the diminished expression of MHC class I molecules that facilitates decreased cytotoxic T-cell recognition and subsequent tumor growth in squamous cell carcinoma of the head and neck.
Improved immunogenicity has been observed after the transfer of MHC class I and II genes into tumor cells.[34] Increasing the expression of MHC class I proteins has been studied as a tumor-specific gene therapy in squamous cell carcinoma of the head and neck. A tumor that expresses a human, but foreign, antigen (alloantigen) provokes an intense immune response, not only to the MHC class I alpha-chain and beta2-microglobulin, but also to the tumor-specific antigens that they present.
Allovectin-7: This alloantigen concept provided the foundation for the development of Allovectin-7, which contains a plasmid that encodes for class I MHC human leukocyte antigen (HLA)-B7 alpha-chain and beta2-microglobulin.[14,35] The plasmid is contained in a liposomal vector because a low level of transfection is thought to be sufficient for an intense immune reaction and tumor reduction. Liposomal vectors also avoid the potential toxicities associated with viral vectors. No toxicity was observed in animal studies of Allovectin-7.[36]
A phase I trial of Allovectin-7 in 20 patients with recurrent or refractory squamous cell carcinoma of the head and neck was completed by Gleich.[14] Tumors were injected once a week for 2 weeks, for a total of two cycles if they did not exhibit disease progression. No drug-related adverse events occurred.
Disease progressed after one cycle in 11 patients, who had a median survival of 21 weeks. Nine patients completed two cycles of treatment, with a median survival of 54 weeks. Time to tumor progression ranged from 20 to 80 weeks in these nine patients. At 16 weeks, four patients exhibited a partial response, two had stable disease, and three progressed. Only one patient survived for 106 weeks without additional treatment. Expression of HLA-B7 was demonstrated in the treated tumors, and increased apoptosis was seen in responding tumors. Currently, a multi-institutional trial is ongoing to further evaluate this treatment.
‘Suicide’ Gene Therapy
Gene-directed enzyme prodrug (GDEP) therapy, also called "suicide" gene therapy, is widely used. This strategy involves the introduction of a gene into a cell that enables the activation of a prodrug into an active cytotoxic drug.
The most extensively studied approach of this sort utilizes HSV-tk. The gene encodes a viral enzyme that phosphorylates ganciclovir into a monophosphate form, which is then further phosphorylated by intracellular enzymes into an active triphosphate compound that terminates DNA synthesis.[37] Thus, this system selectively targets actively dividing cancer cells. Ganciclovir is also an excellent substrate for HSV-tk and a poor substrate for mammalian thymidine kinase, thereby making cytotoxic levels achievable in transfected cells, while leaving untreated cells relatively unharmed.[38]
The Bystander Effect: Another effect of GDEP therapy with the HSV-tk system is described as the "bystander effect." This phenomenon involves the killing of nontransduced dividing cells, presumably due to the transfer of the active toxic metabolite. The process is mediated by gap junctions between cells, through which the toxic metabolite is able to pass.[39] As a result of the bystander effect, a significant antitumor effect is seen only when 10% of the tumor cells are transduced.
Animal Studies: Suicide gene therapy for head and neck cancer has been evaluated in animal models using HSV-tk with ganciclovir. In the treatment of a nude mouse model of human-derived squamous cell carcinoma, significant antitumor effects and extended survival were demonstrated.[40]
In an evaluation of this treatment in immunocompetent mice, efficacy and safety were also confirmed.[41] Moreover, HSV-tk was found in distant organs (eg, liver, lung, kidney) in animals treated at higher doses.
Clinical Trials: Clinical evaluations of suicide gene therapy using HSV-tk and ganciclovir have been performed in ovarian cancer, malignant mesothelioma, and malignant brain tumors.[14]
In a phase I/II study of 12 patients with recurrent glioblastoma, tumors were debulked and injected with HSV-tk followed by intravenous ganciclovir.[42] No significant adverse events occurred. At 4 months, 4 patients showed no evidence of tumor recurrence, with a median survival of 528 days, compared to 194 days for nonresponders. At 2.8 years after treatment, 1 patient is still disease free. Phase I studies of HSV-tk in patients with recurrent squamous cell carcinoma of the head and neck are being considered.
Replicating Viruses That Destroy Tumor Cells
FIGURE 1
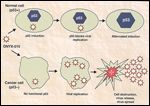
Selective Effect of ONYX-015 on p53-Deficient Cells
Another novel approach to gene therapy for squamous cell carcinoma of the head and neck involves a vector that selectively replicates within and lyses tumor cells. An E1B-55kD gene-deleted adenovirus, ONYX-015 (dl1520), is currently being developed for the treatment of tumors lacking p53 function.[43-45] Since the E1B-55kD gene product is responsible for p53 binding and inactivation, it has been hypothesized that an E1B-55kD deletion mutant would be unable to inactivate p53 in normal cells and would thus be unable to efficiently replicate. In contrast, cancer cells lacking functional p53 (eg, due to gene mutation) would hypothetically be sensitive to viral replication and subsequent cytopathic effects (Figure 1).
Animal studies with ONYX-015 have also suggested that the efficacy of the virus is significantly augmented with the administration of standard chemotherapeutic agents.[44]
Clinical Trials: Results of a phase I clinical investigation with intratumoral injection of ONYX-015 in advanced head and neck cancer confirmed the agent’s safety, with the main toxicity being grade 1 to 2 flu-like symptoms.[46] Evidence for virus replication was found by in situ hybridization in posttreatment biopsies. In addition, no cytolytic activity was observed in surrounding normal tissues.
A recently reported phase II study evaluated intratumoral ONYX-015 in combination with cisplatin and 5-FU in 37 patients with recurrent or refractory squamous cell carcinoma of the head and neck.[47] Patients were treated with 1010 plaque-forming units of virus per day for 5 consecutive days. Chemotherapy consisted of cisplatin (80 mg/m2 IV) on day 1 and 5-FU (800 to 1,000 mg/m2 IV per day) on days 1 through 5. The treatment was well tolerated and chemotherapy toxicity was not significantly altered by concomitant viral therapy.
In 30 evaluable patients, 19 (63%) showed an objective response, consisting of 8 complete responses and 11 partial responses. With a median follow-up of 5 months, none of the 19 responding tumors had progressed. Interestingly, in 6 patients with multiple tumors, the injected tumor responded, while the noninjected tumor did not, thereby suggesting that the antitumor effects are due to the viral replication in combination with chemotherapy, rather than the chemotherapy alone. Median survival of patients was 10.5 months.
Currently, a phase III investigation is commencing to further evaluate the efficacy of this treatment regimen with a control arm of cisplatin and 5-FU alone.
Related Replicating Virus: A similar E1B-deleted, replicating adenovirus has been constructed that also contains the HSV-tk gene.[48,49] This virus has been quite effective in in vitro and in vivo studies due to its dual method of action-both viral oncolysis and ganciclovir-induced cytotoxicity. This virus has yet to be studied in clinical trials.
Conclusions
Gene therapy offers an innovative approach to the treatment of cancer. As our understanding of the molecular mechanisms of cancer expands, it is becoming possible to exploit these principles and to selectively target tumors. Squamous cell carcinoma of the head and neck is an attractive tumor target due to its frequent genetic mutations and propensity for local/regional recurrence. Phase I trials have established the safety of gene therapy in squamous cell carcinoma of the head and neck, and phase II studies have demonstrated clinical efficacy.
Phase III clinical trials and studies of the use of gene therapy in the adjuvant setting are needed. Importantly, gene therapy has the potential for reducing the tumor burden and improving quality of life in patients with squamous cell carcinoma of the head and neck. This modality therefore merits further investigation.
References:
1. Greenlee RT, Hill-Harmon M, Murray T, et al: Cancerstatistics, 2001. CA Cancer J Clin 51:15-36, 2001.
2. Ganly I, Soutar DS, Kaye SB: Current role of gene therapy inhead and neck cancer. Eur J Surg Oncol 26:338-343, 2000.
3. Schwartz GJ, Mehta RH, Wenig BL, et al: Salvage treatment forrecurrent squamous cell carcinoma of the oral cavity. Head Neck 22:34-41, 2000.
4. Pearlman NW: Treatment outcome in recurrent head and neckcancer. Arch Surg 114:39-42, 1979.
5. Jones KR, Lodge-Rigal RD, Reddick RL, et al: Prognosticfactors in the recurrence of stage I and II squamous cell cancer of the oralcavity. Arch Otolaryngol Head Neck Surg 118:483-485, 1992.
6. Fu KK, Lichter A, Galante M: Carcinoma of the floor of themouth: An analysis of treatment results and the sites and causes of failures.Int J Radiat Oncol Biol Phys 1:829-837, 1976.
7. Paredes J, Hong W, Felder T, et al: Prospective randomizedtrial of high-dose cisplatin and fluorouracil infusion with or without sodiumdiethyldithiocarbamate in recurrent and/or metastatic squamous cell cancer ofthe head and neck. J Clin Oncol 6:955-962, 1988.
8. Jacobs C, Lyman G, Velez-Garcia E, et al: A phase IIIrandomized study comparing cisplatin and fluorouracil as single agents and incombination for advanced squamous cell carcinoma of the head and neck. J ClinOncol 10:257-263, 1992.
9. Forastiere A, Metch B, Schuller D, et al: Randomizedcomparison of cisplatin plus fluorouracil and carboplatin plus fluorouracil vsmethotrexate in advanced squamous cell carcinoma of the head and neck: ASouthwest Oncology Group study. J Clin Oncol 10:1245-1251, 1992.
10. Schrijvers D, Johnson J, Jimenez U, et al: Phase III trialof modulation of cisplatin/fluorouracil chemotherapy by interferon alfa-2b inpatients with recurrent or metastatic head and neck cancer. J Clin Oncol16:1054-1059, 1998.
11. Liverpool Head and Neck Oncology Group: A phase IIIrandomized trial of cisplatin, methotrexate, cisplatin + methotrexate, andcisplatin + 5-FU in end-stage squamous carcinoma of the head and neck. Br JCancer 61:311-315, 1990.
12. Clavel M, Vermorken J, Cognetti F, et al: Randomizedcomparison of cisplatin, methotrexate, bleomycin, and viscristine (CABO) vscisplatin and 5-fluorouracil vs cisplatin in recurrent or metastatic squamouscell carcinoma of the head and neck: A phase III study of the EORTC Head andNeck Cancer Cooperative Group. Ann Oncol 5:521-526, 1994.
13. Cusack JC, Tanabe KK: Cancer gene therapy. Surg Oncol Clin NAm 7:421-471, 1998.
14. Gleich LL: Gene therapy for head and neck cancer.Laryngoscope 110:708-726, 2000.
15. Clayman GL: The current status of gene therapy. Semin Oncol27:39-43, 2000.
16. Boyle JO, Hakim J, Kock WM, et al: The incidence of p53mutations increases with progression of head and neck cancer. Cancer Res53:4477-4480, 1993.
17. Caamano J, Zhang SY, Rosvold EA, et al: P53 alterations inhuman squamous cell carcinomas and carcinoma cell lines. Am J Pathol142:1131-1139, 1993.
18. Shin DM, Lee JS, Lippman SM, et al: p53 expression:Predicting recurrence and second primary tumors in head and neck squamous cellcarcinoma. J Natl Cancer Inst 8:519-528, 1996.
19. Clayman GL, el-Naggar AK, Lippman SM, et al:Adenovirus-mediated p53 gene transfer in patients with advanced recurrent headand neck squamous cell carcinoma. J Clin Oncol 16:2221-2232, 1998.
20. Clayman GL, Frank DK, Bruso PA, et al: Adenovirus-mediatedwild-type p53 gene transfer as a surgical adjuvant in advanced head and neckcancers. Clin Cancer Res 5:1715-1722, 1999.
21. Clayman GL, Dreiling LK: Injectable modalities as local andregional strategies for head and neck cancer. Hematol Oncol Clin North Am13:787-810, 1999.
22. Clayman GL, el-Naggar AK, Roth JA, et al: In vivo moleculartherapy with p53 adenovirus for microscopic residual head and neck squamouscarcinoma. Cancer Res 55:1-6, 1995.
23. Lui TJ, el-Naggar AK, McDonnell TJ, et al: Apoptosisinduction mediated by wild-type p53 adenoviral gene transfer in squamous cellcarcinoma of the head and neck. Cancer Res 55:3117-3122, 1995.
24. Fujiwara T, Grimm EA, Mukhopadhyay T, et al: Induction ofchemosensitivity in human lung cancer cells in vivo by adenovirus-mediatedtransfer of the wild-type p53 gene. Cancer Res 54:2287-2291, 1994.
25. Rocco JW, Li D, Liggett WH, et al: p16INK4A adenovirusmediated gene therapy for human head and neck squamous cell cancer. Clin CancerRes 4:1697-1704, 1998.
26. Nemunaitis J, Kuhn JA: Immune modulation as cancer treatmentusing gene therapy. BUMC Proc 12:231-237, 1999.
27. Papac R, Minor DR, Rudnck S, et al: Controlled trial ofmethotrexate and bacillus Calmette-Guérin therapy for advanced head and neckcancer. Cancer Res 38:3150-3153, 1978.
28. Taylor SG IV, Sisson GA, Bytell DE, et al: A randomizedtrial of adjuvant BCG immunotherapy in head and neck cancer. Arch Otolaryngol109:544-549, 1983.
29. Siegel JP, Puri RK: Interleukin-2 toxicity. J Clin Oncol9:694-704, 1991.
30. Cortesina G, De Stefani A, Sacchi M, et al: Immunomodulationtherapy for squamous cell carcinoma of the head and neck. Head Neck 15:266-270,1993.
31. Li D, Jiang W, Bishop JS, et al: Combination surgery andnonviral interleukin-2 gene therapy for head and neck cancer. Clin Cancer Res5:1551-1556, 1999.
32. O’Malley BW Jr, Li D, Buckner A, et al: Limitations ofadenovirus-mediated interleukin-2 gene therapy for oral cancer. Laryngoscope109:389-395, 1999.
33. Myers JN, Mank-Seymour A, Zitvogel L, et al: Interleukin-12gene therapy prevents establishment of SCC VII squamous cell carcinomas,inhibits tumor growth, and elicits long-term antitumor immunity in syngeneic C3Hmice. Laryngoscope 108:261-268, 1998.
34. Plautz GE, Yang ZY, Wu BY, et al: Immunotherapy ofmalignancy by in vivo gene transfer into tumours. Proc Natl Acad Sci USA90:4645-4649, 1993.
35. Gleich LL, Gluckman JL, Armstrong S, et al: Alloantigen genetherapy for squamous cell carcinoma of the head and neck: Results of a phase Itrial. Arch Otolaryngol Head Neck Surg 124:1097-1104, 1998.
36. Parker SE, Vahlsing HL, Serfilippi LM, et al: Cancer genetherapy using plasmid DNA: Safety evaluation in rodents and non-human primates.Hum Gene Ther 6:575-590, 1995.
37. Matthews T, Boehme R: Antiviral activity and mechanism ofaction of ganciclovir. Rev Infect Dis 10(suppl 3):490-494, 1988.
38. O’Malley BW Jr, Cope KA, Chen SH, et al: Combination genetherapy for oral cancer in a murine model. J Cancer Res 56:1737-1741, 1996.
39. Freeman SM, Abboud CN, Whartenby KA, et al: The"bystander effect": Tumor regression when a fraction of the tumor massis genetically modified. Cancer Res 53:5274-5283, 1993.
40. O’Malley BW Jr, Chen SH, Schwartz MR, et al:Adenovirus-mediated gene therapy for human head and neck squamous cell cancer ina nude mouse model. Cancer Res 55:1080-1085, 1995.
41. Sewell DA, Li D, Duan L, et al: Safety of in vivoadenovirus-mediated thymidine kinase treatment of oral cancer. Arch OtolaryngolHead Neck Surg 123:1298-1302, 1997.
42. Klatzmann D, Valery CA, Bensimon G, et al: A phase I/IIstudy of herpes simplex virus type 1 thymidine kinase suicide gene therapy forrecurrent glioblastoma. Study group on gene therapy for glioblastoma. Hum GeneTher 9:2595-2604, 1998.
43. Heise CC, Williams A, Olesch J, et al: Efficacy of areplication competent adenovirus (ONYX-015) following intratumoral injection:Intratumoral spread and distant effects. Cancer Gen Ther 6:499-504, 1999.
44. Heise CC, Sampson-Johannes A, Williams A, et al: ONYX-015and E1B gene-attenuated adenovirus cause tumor-specific cytolysis andantitumoral efficacy that can be augmented by standard chemotherapeutic agents.Nat Med 6:639-645, 1997.
45. Bischoff JR, Kirn DH, Williams A, et al: An adenovirusmutant that replicates selectively in p53-deficient human tumor cells. Science274:373-376, 1996.
46. Ganly I, Kirn D, Eckhardt SG, et al: Phase I study ofONYX-015, an E1B attenuated adenovirus, administered intratumorally to patientswith recurrent head and neck cancer. Clin Cancer Res 6:798-806, 2000.
47. Khuri F, Nemunaitis J, Ganly I, et al: A controlled trial ofintratumoral ONYX-015, a selectively replicating adenovirus, in combination withcisplatin and 5-FU in patients with recurrent head and neck cancer. Nat Med6:879-885, 2000.
48. Wildner O, Morris JC, Vahanian NN, et al: Adenoviral vectorscapable of replication improve the efficacy of HSVtk/GCV suicide gene therapy.Gene Ther 6:57-62, 1999.
49. Wildner O, Morris JC: The role of the E1B 55 kDa geneproduct in oncolytic adenoviral vectors expressing herpes simplex virus-tk:Assessment of antitumor efficacy and toxicity. Cancer Res 60:4167-4174, 2000.