Surprising Success in Immunotherapy Treatment for Leukemia
Researchers at the University of Pennsylvania have reported on the results of a trial in which a patient with chronic lymphocytic leukemia (CLL) experienced a complete remission after immunotherapy with tumor-reactive modified T cells.
Researchers at the University of Pennsylvania have reported on the results of a trial in which patients with chronic lymphocytic leukemia (CLL) experienced a complete remission after immunotherapy with tumor-reactive modified T cells. The studies were reported last week in the New England Journal of Medicine, DOI: 10.1056/NEJMoa1103849 and in the journal Science Translational Medicine.
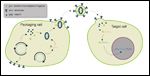
Packaging and infection by a lentiviral vector
David Porter and his colleagues designed a lentiviral vector that expressed a chimeric antigen receptor with specificity for the B-cell antigen CD19, coupled with CD137 (a costimulatory receptor in T cells) and CD3-zeta (a signal-transduction component of the T-cell antigen receptor) signaling domains.
The researchers pretreated patients with chemotherapy with pentostatin and cyclophosphamide in order to deplete their lymphocytes. A low dose of the autologous chimeric antigen receptor–modified T cells was then reinfused into the patient.
Twenty-two days after treatment, tumor lysis syndrome was diagnosed; at this time, high levels of cytokines (interferon-γ and interleukin-6) were detected and circulating chimeric antigen receptor-positive T cells (CAR T cells) were found to have expanded to a level that was more than 1000 times as high as the initial engraftment level. Some of these CAR T cells persisted with a memory phenotype, which enabled them to respond quickly and effectively to a second exposure to CLL cells.
Indeed, eight months later, the high chimeric antigen receptor-positive T cell levels persisted, and two of the three CLL patients who underwent treatment had complete remission of their leukemia. On average, the researchers believe, each engineered T cell had killed roughly 1,000 cancer cells. The side effects from treatment included loss of normal B cells and tumor lysis syndrome.
Dr. David Porter, director of the blood and marrow transplantation program at the Hospital of the University of Pennsylvania in Philadelphia and a coauthor of both papers said that the researchers knew the therapy could be "very potent, but I don't think we expected it to be this dramatic on this go-around."
Thus far, therapy with tumor-infiltrating lymphocytes and other immunotherapies that have been clinically tested have proven to be costly and time-consuming. In an editorial in the NEJM, by Walter Urba at Oregon Health & Science University and colleagues, Urba states that “Chimeric antigen receptors have theoretical advantages over other T-cell based therapies,” but it seems that the jury is still out over whether this data will prove to have wide clinical significance.