Updated CheckMate 649 Results Show Sustain Benefit of Nivolumab Plus Chemo for Gastric/GEJ Cancer
Nivolumab in combination with chemotherapy was beneficial vs chemotherapy alone in patients with gastric or gastroesophageal junction cancer at a follow-up of at least 24 months.
Follow-up data from the CheckMate 649 trial (NCT02872116) that were presented at the 2022 Gastrointestinal Cancers Symposium indicated that use of nivolumab (Opdivo) plus chemotherapy for patients with gastric or gastroesophageal junction (GEJ) cancer continued to result in durable survival benefit, with lead author Kohei Shitara, MD, reporting overall and progression-free survival (PFS) advantages across key patient subgroups.1
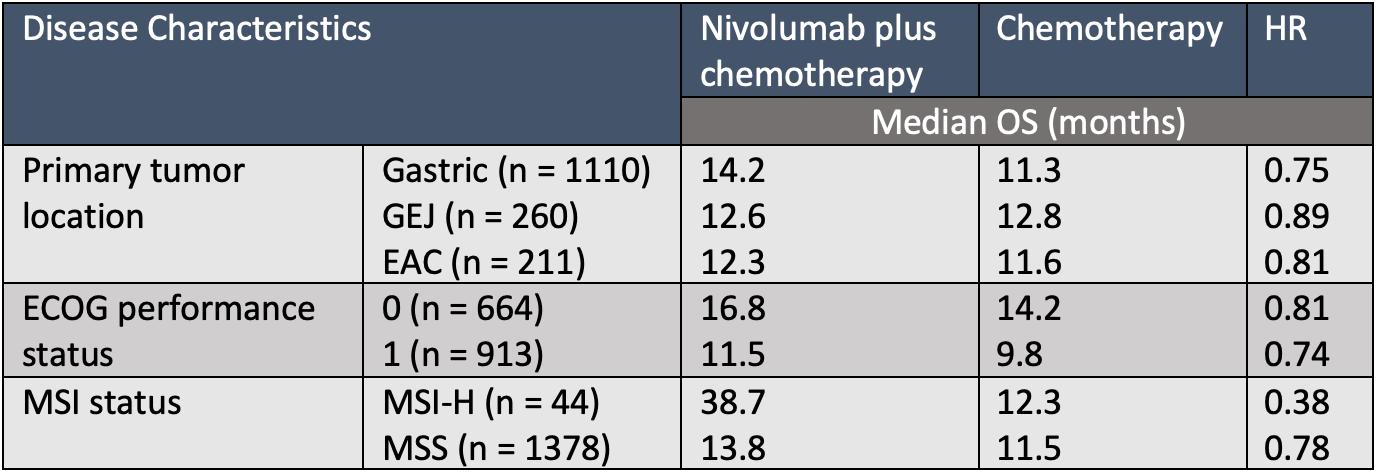
Results showed that the median overall survival (OS) was 13.8 months (95% CI, 12.4-14.5) vs 11.6 (95% CI, 10.9-12.5) favoring the combination (HR, 0.79; 95% CI 0.71-0.88). The combination was associated with improved median OS irrespective of microsatellite status, tumor location, or ECOG performance score (TABLE). The median PFS was 7.7 months (95% CI, 7.1-8.6) in the combination arm vs 6.9 months (95% CI, 6.7-7.2) with chemotherapy (HR, 0.79; 0.70-0.89).
EAC, esophageal adenocarcinoma; GEJ, gastroesophageal junction; MSS, microsatellite stable; MSI, microsatellite instability status; MSI-H, microsatellite instability high.
“Nivolumab plus chemotherapy continues to demonstrate clinically meaningful improvement in efficacy at 24 months follow-up and was characterized by favorable PFS2 in all randomized patients,” said Shitara, chief of the Department of Gastrointestinal Oncology at National Cancer Center Hospital East in Kashiwa, Japan.
Additionally, nivolumab/chemotherapy was associated with a 25% reduction in the risk for death or disease progression on subsequent therapy. The median PFS2 was 12.2 months (95% CI, 11.3-13.5) vs 10.4 months (95% CI, 9.7-11.2) with the combination (HR, 0.75; 95% CI, 0.67-0.84).
“Clinically meaningful improvement in overall survival and PFS with nivolumab/chemotherapy was maintained with longer follow-up,” Shitara said. “Actual 2-year survival rates were 28% with nivolumab/chemotherapy and 19% with chemotherapy.”
In April 2021, the FDA approved nivolumab for use in combination with select types of chemotherapy for the frontline treatment of patients with advanced or metastatic gastric cancer, GEJ cancer, and esophageal adenocarcinoma, based on earlier findings of CheckMate 649.2
Investigators recruited 2031 patients with previously untreated, unresectable, advanced or metastatic gastric/GEJ/esophageal adenocarcinoma into the open-label, international, phase 3 CheckMate 649 trial irrespective of PD-L1 status. Patients were then assigned to 1 of 3 treatment arms: nivolumab at 360 mg plus XELOX chemotherapy every 3 weeks or nivolumab at 240 mg plus FOLFOX every 2 weeks (n = 789); XELOX every 3 weeks or FOLFOX every 2 weeks (n = 833); or nivolumab at 1 mg/kg plus ipilimumab (Yervoy) at 3 mg/kg every 3 weeks for 4 cycles, followed by nivolumab at 240 mg every 2 weeks (n = 409).
The new analysis included 789 patients assigned to nivolumab/chemotherapy and 792 assigned to chemotherapy alone.
Patients had to have an ECOG performance status of 0 or 1 as well as no known HER2-positive status. Stratification factors included PD-L1 expression on tumor cells (≥1 vs <1%), region (Asia vs United States/Canada vs rest of world), ECOG performance status (0 vs 1), and chemotherapy regimen (XELOX vs FOLFOX).
Baseline characteristics were balanced across the treatment arms. The median age was 61.5 years (range, 18-90) and 69.5% of patients were male. Seventy percent of patients had gastric cancer, 16.5% had GEJ, and 13.5% had esophageal adenocarcinoma. The majority of patients (87%) had microsatellite stable disease.
The minimum follow-up was 24.0 months in the nivolumab/chemotherapy arm.
Nivolumab/chemotherapy improved OS and objective response rate (ORR) across all PD-L1 subgroups. “The overall survival hazard ratio was 0.69 in patients with a CPS of 5 or higher versus 0.94 for patients with a CPS less than 5,” Shitara said. “Notably, response rates are higher in the nivolumab/chemotherapy arm across all PD-L1 CPS [cutoffs].”
Investigators next excluded patients with microsatellite instability–high (MSI-H) status in the PD-L1 analysis. The HR was 0.71 for patients with a CPS of 5 or higher compared with 0.94 for those below 5. Shitara said these data were consistent with findings in the overall population.
ORR was higher and responses were more durable with the combination whether or not CPS was at least 5. For patients with a score at least 5, the ORR was 60% (95% CI, 55%-65%) with 13 complete responses (CR) and 47 partial responses (PR) with nivolumab/chemotherapy (n = 378). The median duration of response was 9.7 months (95% CI, 8.2-12.4) vs 7.0 months (95% CI, 5.6-7.9) in favor of the combination.
For those with a CPS less than 5, the ORR was 55% (95% CI, 48%-62%) with 7 CRs and 48 PRs with nivolumab/chemotherapy (n = 219). The median duration of response was 7.7 months (95% CI, 6.2-9.9) vs 6.9 months (95% CI, 5.7-8.2) in favor of the combination.
Shitara said the adverse event (AE) profile with the combination was consistent with the individual drug components and investigators identified no new safety signals. Sixty percent of patients in the combination arm experienced grade 3/4 treatment-related (TR) AEs compared with 45% in the chemotherapy arm. Seventeen percent and 10% of patients, respectively, experienced grade 3/4 serious TRAEs.
Eighteen percent of patients in the combination arm discontinued due to grade 3/4 TRAEs vs 9% assigned to chemotherapy. Investigators observed 16 (2%) treatment-related deaths compared with 4 (<1%) in the chemotherapy arm. The most common grade 3/4 TRAEs in the combination arm included neutropenia (15%), decreased neutrophil count (11%), and anemia (6%).
Grade 3/4 TRAEs with potential immunologic etiology occurred in 5% of patients or less in the combination arm.
References
- Shitara K, Janjigian YY, Moehler M, et al. Nivolumab (NIVO) plus chemotherapy (chemo) versus chemo as first-line (1L) treatment for advanced gastric cancer/gastroesophageal junction cancer/esophageal adenocarcinoma (GC/GEJC/EAC): Expanded efficacy, safety, and subgroup analyses from CheckMate 649. J Clin Oncol. 2022;40(suppl; abstr 240). doi:10.1200/JCO.2022.40.4_suppl.240
- FDA approves first immunotherapy for initial treatment of gastric cancer. News release. FDA. April 16, 2021. Accessed April 16, 2021. https://bit.ly/3tqsjKA
Targeted Therapy First Strategy Reduces Need for Chemotherapy in Newly Diagnosed LBCL
December 7th 2025Lenalidomide, tafasitamab, rituximab, and acalabrutinib alone may allow 57% of patients with newly diagnosed LBCL to receive less than the standard number of chemotherapy cycles without compromising curative potential.