Immunotherapy in Colorectal Cancer
Immune checkpoint inhibitors have demonstrated impressive activity in patients with CRC and other solid tumors that are dMMR. Researchers explore the data.
FIGURES (1)
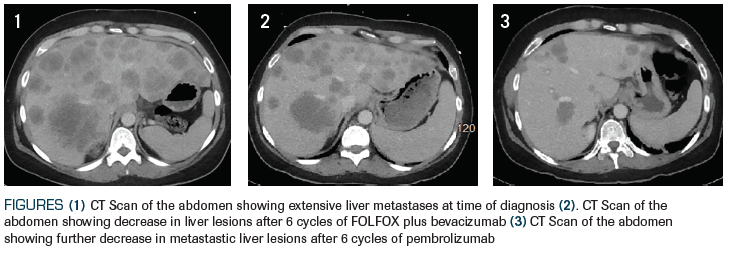
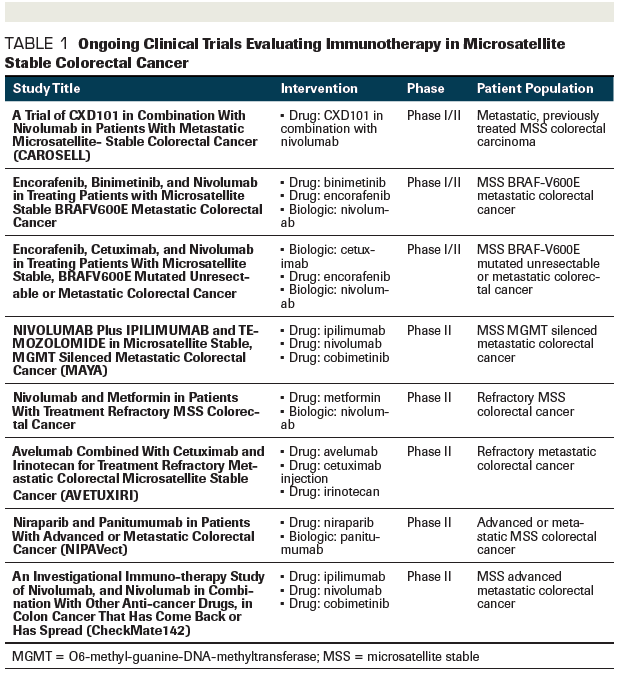
TABLE 1: Ongoing Clinical Trials Evaluating Immunotherapy in Microsatellite Stable Colorectal Cancer

ABSTRACT: Colorectal cancer (CRC) is the third leading cause of cancer deaths, with only 15% of patients surviving 5 years in the metastatic setting. Recent exciting developments in cancer immunotherapy, which involves priming the host’s natural immune defenses to recognize, target, and destroy cancer cells effectively, have brought some glimpse of hope in fighting this deadly disease. Although CRC has been shown to evade immune detection like many other cancers do, immunotherapy has been noted to produce some very impressive results in a select group of patients. Patients with mismatch repair-deficient and microsatellite instability-high type CRC have benefited most from recent immunotherapy approaches, leading to US Food and Drug Administration approval of new immunotherapeutic agents in recurrent refractory metastatic disease. Research continues to explore and hopefully define the role of immunotherapy in CRC as single-agent therapy or in combination with other agents in neoadjuvant, adjuvant, and first-line metastatic setting, and to find the optimal combination and sequencing of this new therapeutic approach. One of the most challenging tasks is to find ways to expand the use of immunotherapy to not only a select group of CRC patients but also to all patients with this disease. This article will provide a practical concise overview of the current landscape of immunotherapy in CRC for the practicing oncologist along with a representative case presentation from our community oncology practice.
Introduction
CRC is the second leading cause of cancer death among men and women and the third most common cancer diagnosis in the United States, with an estimated 145,600 new cases and 51,020 cancer-related deaths to occur in 2019.[1] The majority of patients with metastatic CRC have incurable disease, with a median overall survival of 30 months at best.[2,3] Based on the molecular genetic profile, various subsets of CRC with different predictive and prognostic behavior have been described. Among the most widely recognized and well known to most practicing oncologists are the main subtypes: mismatch repair-deficient or microsatellite instability-high (dMMR–MSI-H) tumors and mismatch repair-proficient or microsatellite instability-low (pMMR–MSI-L) tumors.[4] Microsatellite instability (MSI) occurs as a result of germline mutations in the genes of MLH1, MSH2, MSH6, and PMS2, which are involved in the DNA mismatch repair (MMR) pathway that encode MMR proteins. MSI results from either insertion or deletion of repeat units of DNA base pairs attributed to defects in the DNA MMR system.[5] The MSI subgroup makes up approximately 15% of all comers in CRC, but its prevalence is stage dependent. Whereas up to 15% of stage II/III CRCs are dMMR, only 4% to 5% of stage IV CRCs are dMMR.[6,7] Although two-thirds of the dMMR CRC cases are sporadic and associated with epigenetic modification leading to the inactivation of the MLH1 gene, one-third of dMMR deficiency cases are part of the hereditary nonpolyposis colorectal cancer syndrome, also known as Lynch syndrome.[8] CRC patients with MSI-H tumors exhibit distinct clinical and pathologic features such as younger age, early stage, proximal colon location, and poorly differentiated histology with rich tumor-infiltrating lymphocytes.[9]
Immune checkpoint inhibitors have demonstrated impressive activity in patients with CRC and other solid tumors that are dMMR.[10] These dMMR tumors exhibit high levels of frameshift mutations detectable as variability in the length of short stretches of DNA (microsatellites). This has been called MSI and has been noted to make these tumors more prone to accumulating mutations, which leads to the generation of neoantigens that can be recognized by the immune system. To counteract and avoid immune detection and destruction, tumor cells express cell surface inhibitory checkpoint molecules that downregulate the immune response (eg, programmed death-1 [PD-1]/PD-1 ligand 1 [PD-L1] and cytotoxic T-lymphocyte–associated antigen-4 [CTLA-4]).[10] Blocking PD-1/PD-L1 and CD80/CTLA-4 interactions has proven to be a very effective immunotherapy approach.
Many critical questions remain regarding the most appropriate use of immunotherapy in CRC. Among these are: role of immunotherapy in neoadjuvant, adjuvant, and first-line metastatic setting; single agent versus most optimal combination with other available cytotoxic, targeted, and immunotherapeutic agents; discovery and development of good prognostic and predictive biomarkers for response; and role of other immunotherapeutic approaches such as vaccines, cellular therapies, and cytokines targeting other immune checkpoint molecules, macrophages, and components of innate immunity.
Current landscape of immunotherapy in colon cancer
Recent discoveries and our better understanding of the complex interactions between cancer cells and the immune system has led to novel and successful immunotherapeutic approaches. Treatment with selective anti-PD-1, anti-PD-L1, and/or anti-CTLA-4 monoclonal antibodies has revolutionized our therapeutic approach to several cancer types. While the highest clinical efficacy of immunotherapy has been observed in melanoma and lung cancer, results in CRC have been less than impressive except in the dMMR–MSI-H group.
The clinical heterogeneity of CRC that occurs during its pathogenesis is driven by chromosomal alterations and defective DNA mismatch-repair gene function. Based on both tumor and infiltrating stromal gene expression profiles, a consensus molecular subtype (CMS) classification has been proposed to identify four major groups of colorectal cancer. CMS1 (MSI-like) constitutes approximately 14% of CRC cases and harbors hypermutated tumors with MSI-H features. This group can also exhibit BRAF mutations and display a robust immune infiltration. CMS2 (canonical) constitutes 37% of cases characterized by the activation of the WNT and MYC pathways. CMS3 (metabolic) constitutes approximately 13% of the cases with frequent KRAS mutations and a deregulation of metabolic pathways in cancer cells. Finally, CMS4 (mesenchymal) constitutes approximately 23% of the cases characterized by transforming growth factor (TGF)-Ã pathway activation, enhanced angiogenesis, stromal activation, and inflammatory infiltrate.[11] While CMS1 and CMS4 tumors show intense immune infiltration, CMS2 and CMS3 tumors lack immune activation in their microenvironment. This molecular characterization of CRC has provided some basis for the identification of favorable and unfavorable immune response attributes linked to clinical outcomes.[12]
MSI-H tumors have been identified as the best candidates for immunotherapy treatment, and a number of studies have evaluated the efficacy of anti-PD-L1 and anti-CTLA-4 monoclonal antibodies in this setting. Two phase II trials (KEYNOTE-016 and KEYNOTE-164) and one phase II trial (CheckMate-142) conducted in previously treated MSI-H/dMMR metastatic CRC patients provided objective response rates (ORR) ranging from 28% to 52%, progression-free survival (PFS) rates ranging from 34% to 59%, and overall survival (OS) rates of 72% to 76%.[13–15] CheckMate-142 evaluated nivolumab with or without low-dose ipilimumab in previously treated MSI-H/dMMR metastatic CRC with an ORR of 55% and disease control rate for 12 weeks or longer of 80%.[15] Currently, there are three US Food and Drug Administration (FDA)-approved immunotherapeutic agents (pembrolizumab, nivolumab plus or minus ipilimumab) for metastatic CRC patients with MSI-H/dMMR.[16–18]
Unfortunately, the vast majority of CRC patients, the pMMR/microsatellite stable (MSS) group, does not benefit from immunotherapy. Novel therapeutic approaches are needed to render this group of CRC patients immunogenic and thus offer effective immunotherapies. Hypothetically, immunotherapy might be effective for all CRC types if they were able to be converted to a “CMS1-like” immune phenotype. CMS4 tumors, which show the worst prognosis in terms of overall and relapse-free survival, for example, are characterized by an unfavorable, inflamed immune phenotype revealing high expression of mesenchymal genes, stromal cell infiltration, and an angiogenic microenvironment. Vascular endothelial growth factor-A (VEGF-A), a proangiogenic molecule produced by the tumors, has been shown to have a crucial role in the development of this immunosuppressive microenvironment.[19] Several clinical trials are investigating whether the combination of bevacizumab with either immunotherapy alone or combined with targeted therapies and conventional chemotherapy might show activity in this setting (ie, NCT02873195, NCT02291289, NCT02876224). CMS4 tumors also show activation of the TGF-Ã signaling pathway. Targeting the TGF-Ã pathway either as monotherapy and/or in combination with anti-PD-1 agents has been the subject of some basic science research.[20,21]
The other two molecular types of CRC, CMS2 and CMS3, have been also called “cold” tumors, meaning that they lack immune cell infiltration. In this group, the expression of immunosuppressive genes has been noted to be low, suggesting different mechanisms of immune escape. Novel therapeutic approaches to render CMS2 and CMS3 tumors immunogenic are being explored. Among those are cytokine treatment, cancer vaccination, and passive immunotherapy with adoptive T-cell transfer or monoclonal antibodies targeting tumor-associated antigens.[22]
Critical questions and proposed answers for the practicing community oncologist:
What are the currently approved immunotherapeutic treatment options for colorectal cancer?
Currently, there are three FDA-approved immunotherapeutic agents (pembrolizumab, nivolumab plus or minus ipilimumab) for metastatic CRC patients with MSI-H/dMMR.[16–18]
What are the biomarkers of immune response in CRC?
Several ongoing studies are investigating potential targetable pathways involved in the host immune response to CRC. Correlative studies from clinical trials are essential to identify biomarkers that can serve as immune response surrogates. Patients harboring MSI-H/dMMR tumors appear to benefit most from colon cancer immunotherapy.[23]. DNA MSI-H defined as instability at more than two loci (or more than 30% of loci if a larger panel of markers is used) results in a high number of DNA replication errors and represents as a predictive biomarker to anti-PD-1 therapy. Utility of PD-L1 expression as a surrogate marker for tumor immunogenicity has been extensively studied. Upregulation of PD-L1 in tumor microenvironment has been found to be associated with an increased effector T-cell infiltration providing higher likelihood of clinical benefit from checkpoint inhibitors in malignancies other than CRC.[24] The immune response to tumor cells can be evaluated by the density and distribution of the tumor-infiltrating lymphocytes, which represents another potential predictive biomarker in CRC. Immunoscore has been developed as a risk stratification tool by quantifying two lymphocyte population densities in the core of the tumor and at the invasive margin.[25] Although immunoscore has been shown to be a better prognostic biomarker than MSI-H status in predicting disease-specific recurrence and survival in CRC, its role in predicting response to immunotherapy agents has not yet been widely accepted.[26]
What is the role of immunotherapy in MSS/pMMR CRC?
Analyses of MSS/pMMR metastatic CRC cohorts in the checkpoint inhibitor trials has not shown any clinically meaningful benefit with either single-agent PD-1 or the combination of PD-1 and CTLA-4 immunotherapy.[27] This can be explained by the lower antigenicity due to the presence of fewer neoantigens. Clinical trials are testing strategies to improve tumor antigenicity by increasing tumor antigen and major histocompatibility complex class I molecule expression, and to positively alter the tumor microenvironment by vaccination.[28] Based on preclinical data showing increased T-cell tumor infiltration and PD-L1 activity with MEK inhibition, a phase III clinical trial assessing the combination of cobimetinib and atezolizumab did not provide survival benefit over regorafenib in refractory metastatic MSS/pMMR CRC.[29,30] Several ongoing clinical trials are trying to address the role of immunotherapy in this group of CRC patients (Table).
When should immunotherapy be utilized in MSI-H/dMMR colon cancer patients?
For metastatic MSI-H/dMMR CRC patients, currently recommended first-line treatment is still combination chemotherapy plus targeted therapy. Nivolumab with or without low-dose ipilimumab and pembrolizumab is approved on progression following first-line treatment with fluoropyrimidine, oxaliplatin, and irinotecan.[31] Although no trials have directly determined whether patients should receive nivolumab alone or in combination with ipilimumab, an indirect comparison suggested that nivolumab plus low-dose ipilimumab provides improved efficacy over nivolumab monotherapy with a favorable risk–benefit profile.[15] Recently, first-line metastatic use of combination immunotherapy (nivolumab 3 mg/kg every 2 weeks plus low-dose ipilimumab 1 mg/kg every 6 weeks) in CRC patients with MSI-H metastatic CRC has been reported with favorable results.[32] This study has enrolled 45 patients. The ORR was 60% (27/45), with 7% complete responses (3/45). The 12-month PFS and OS rates were 77% and 83%, respectively. Grade 3/4 treatment-related adverse events occurred in 16% of patients, with only 7% of patients requiring discontinuation of therapy. Current FDA approval for pembrolizumab, nivolumab, and nivolumab plus ipilimumab for the treatment of MSI-H metastatic CRC patients remains restricted to those who have progressed after first-line therapy. Neoadjuvant treatment with a combination of the immune checkpoint inhibitors nivolumab and ipilimumab achieved major pathologic responses in 7/7 (100%) of early-stage colon cancers with dMMR, according to results reported at ESMO 2018 from the first exploratory phase II trial to investigate this approach.[33] The role of immunotherapy in the adjuvant setting is being evaluated by the ATOMIC trial (Alliance A021502), which is a randomized phase III study of standard chemotherapy (modified FOLFOX-6) alone or in combination with atezolizumab as adjuvant treatment for stage III colon cancer patients with tumors that are deficient DNA MMR with MSI. NCT02912559.
When should immunotherapy be discontinued in responding patients, and what is the outcome of patients who discontinue treatment?
Although outcomes associated with the discontinuation of checkpoint inhibitors have not been rigorously evaluated, subgroup analyses suggest that checkpoint inhibitor therapy may produce long-lasting clinical benefit despite limited treatment duration. Eighteen patients from KEYNOTE-016 who discontinued pembrolizumab after 2 years because of complete remission (n = 11) or intolerance to therapy (n = 7) showed no evidence of recurrence or progression after median times off therapy for 8.3 and 7.6 months, respectively. Sixteen patients from CheckMate-142 with MSI-H/dMMR CRC who discontinued nivolumab plus low-dose ipilimumab because of treatment-related side effects had a disease control rate of 81%, with a median duration of response that was not reached. [34,35]Currently, there are no clear data to define exact treatment duration with checkpoint inhibitors. In most cases, treatments are given until true progression or toxicity occurs.
What is the role of immunotherapy in combination with other available therapies?
Combinations of immune checkpoint inhibitors with chemotherapy, radiation therapy, and targeted therapies (including other immunotherapies) in MSI-H/dMMR metastatic CRC are under rigorous investigation. In a phase Ib/II trial investigating pembrolizumab plus cetuximab in RAS wild-type metastatic CRC, 7 of 9 patients achieved stable disease and treatment was well tolerated.[36] Atezolizumab plus bevacizumab has also been studied in an attempt to augment the antitumor immune response in MSI-H/dMMR CRC.[37] In this phase Ib trial of 10 previously treated patients with MSI-H/dMMR metastatic CRC, atezolizumab plus bevacizumab produced an ORR of 40% and disease control rate of 90%. Nivolumab plus other immunotherapies, such as the anti-lymphocyte-activation gene 3, relatlimab, and daratumumab, and an anti-CD38 cytolytic monoclonal antibody are being investigated in CheckMate-142.[38]
Conclusion
Immunotherapy of cancer is a novel and effective therapeutic strategy. Treatment with selective anti-PD-1, anti-PD-L1, and/or anti-CTLA-4 monoclonal antibodies has brought revolutionary results in MSI-H/dMMR CRC patients. As immune checkpoint inhibitors are integrated into the CRC treatment landscape, their use as single-agent therapy or in combination therapy will evolve and be better defined. Currently, there remain more questions than answers including the timing of treatment initiation, optimal sequencing and optimal duration of treatments and accurate evaluation of response, and management of adverse events. The most difficult challenge of all, however, is to identify those patients with specific tumor and tumor-infiltrating stromal molecular and functional characteristics that could be effectively treated with immunotherapy among the heterogeneous spectrum of CRC patients with MSS/pMMR CRC.
CASE PRESENTATION
A 41-year-old Hispanic woman presented with a 3-month history of abdominal pain and 15-lb weight loss. There was no history of hematemesis, melena, or hematochezia. She was initially treated with antacid and pain medications with no improvement. Further evaluation with a CT scan of chest abdomen and pelvis revealed a right-sided colonic mass with associated lymphadenopathy and an enlarged liver with diffuse hepatic metastases in the abdomen (Figure 1) and small bilateral indeterminate pulmonary nodules in the chest. Needle biopsy of the right node of the liver confirmed a diagnosis of adenocarcinoma consistent with colorectal primary cancer. Colorectal gene panel was negative for pathogenic alterations of KRAS, NRAS, or BRAF. Polymerase chain reaction (PCR) testing detected MSI-H. Gene sequence and deletion/duplication analyses of MLH1, MSH2, MSH6, PMS2, and EPCAM revealed a heterozygous p.S461 pathogenic mutation in the PMS2 gene. Family history was notable only for her maternal grandfather, who had had a diagnosis of colon cancer at age 65.
What is the most appropriate next step?
A. Surgical resection of colon mass followed by systemic therapy
B. Systemic chemotherapy plus immunotherapy
C. Systemic chemotherapy followed by immunotherapy
D. Systemic chemotherapy with FOLFOX or FOLFIRI plus cetuximab or panitumumab
E.Systemic immunotherapy with pembrolizumab or nivolumab plus or minus ipilimumumab
F. Systemic chemotherapy with thew combination regimen of leucovorin, fluorouracil, and oxaliplatin (FOLFOX) or fluorouracil, leucovorin, and irinotecan (FOLFIRI) plus bevacizumab
Correct Answer (F): Systemic chemotherapy with thew combination regimen of leucovorin, fluorouracil, and oxaliplatin (FOLFOX) or fluorouracil, leucovorin, and irinotecan (FOLFIRI) plus bevacizumab
ANSWER EXPLAINED: Patient was started on the regimen of FOLFOX plus bevacizumab for the first-line treatment of her metastatic CRC. After 6 cycles of treatment, restaging CT scans revealed a significant decrease in liver lesions, but several new small (6–9 mm) nodules appeared in bilateral lung fields (Figure 2). Her treatment was changed to single-agent pembrolizumab immunotherapy. After 6 cycles of immunotherapy, restaging scans showed complete disappearance of lung lesions and a further decrease in her liver metastatic disease (Figure 3). To date, she remains on single-agent pembrolizumab with very good tolerance and no evidence of disease progression.B. Systemic chemotherapy plus immunotherapy
References:
1. American Cancer Society. Cancer Statistics Center. Available at: https://cancerstatisticscenter.cancer.org/#/cancer-site/Colorectum. Accessed September 30, 2019.
2. Siegel RL, Miller KD, Jemal A. Cancer statistics, 2018. CA Cancer J Clin. 2018;68:7-30.
3. Loupakis F, Cremolini C, Massi G, et al. Initial therapy with FOLFOXIRI and bevacizumab for metastatic colorectal cancer. N Engl J Med. 2014;371:1609-18.
4. Rodriguez-Salas N, Dominguez G, Barderas R, et al. Clinical relevance of colorectal cancer molecular subtypes. Crit Rev Oncol Hematol. 2017;109:9-19.
5. PeltomÓki P. Role of DNA mismatch repair defects in the pathogenesis of human cancer. J Clin Oncol. 2003;21:1174-9.
6. Gryfe R, Kim H, Hsieh ET, et al. Tumor microsatellite instability and clinical outcome in young patients with colorectal cancer. N Engl J Med. 2000;342:69-77.
7. Koopman M, Kortman GA, Mekenkamp L, et al. Deficient mismatch repair system in patients with sporadic advanced colorectal cancer. Br J Cancer. 2009;100:266-73.
8. Herman JG, Umar A, Polyak K, et al. Incidence and functional consequences of hMLH1 promoter hypermethylation in colorectal carcinoma. Proc Natl Acad Sci U S A. 1998;95:6870-5.
9. Greenson JK, Bonner JD, Ben-Yzhak O, et al. Phenotype of microsatellite unstable colorectal carcinomas: well-differentiated and focally mucinous tumors and the absence of dirty necrosis correlate with microsatellite instability. Am J Surg Pathol. 2003;27:563-70.
10. Le DT, Durham JN, Smith KN, et al. Mismatch repair deficiency predicts response of solid tumors to PD-1 blockade. Science. 2017;357:409-13.
11. Guinney J, Dienstmann R, Wang X, et al. The consensus molecular subtypes of colorectal cancer. Nat Med. 2015;21:1350-6.
12. Roelands J, Kuppen PJK, Vermeulen L, et al. Immunogenomic classification of colorectal cancer and therapeutic implications. Int J Mol Sci. 2017;18:2229-49.
13. Le DT, Kavan P, Kim TW, et al. KEYNOTE-164: Pembrolizumab for patients with advanced microsatellite instability high (MSI-H) colorectal cancer. J Clin Oncol. 2018;36(15 suppl):abstr 3514.
14. Diaz L, Marabelle A, Kim TW, et al. Efficacy of pembrolizumab in phase 2 KEYNOTE-164 and KEYNOTE-158 studies of microsatellite instability high cancers. Ann Oncol. 2017;28(5 suppl):abstr 386P.
15. Andre T, Lonardi S, Wong M, et al. Nivolumab + ipilimumab combination in patients with DNA mismatch repair-deficient/microsatellite instability-high (dMMR/MSI-H) metastatic colorectal cancer (mCRC): first report of the full cohort from CheckMate-142. J Clin Oncol. 2018;36 (4 suppl):abstr 553.
16. U.S. Food and Drug Administration. FDA approves first cancer treatment for any solid tumor with a specific genetic feature. May 23, 2017. Available at: https://www.fda.gov/news-events/press-announcements/fda-approves-first-cancer-treatment-any-solid-tumor-specific-genetic-feature. Accessed September 30, 2019.
17. U.S. Food and Drug Administration. FDA grants nivolumab accelerated approval for MSI-H or dMMR colorectal cancer. Available at: https://www.fda.gov/drugs/resources-information-approved-drugs/fda-grants-nivolumab-accelerated-approval-msi-h-or-dmmr-colorectal-cancer#targetText=On%20July%2031%2C%202017%2C%20the,fluoropyrimidine%2C%20oxaliplatin%2C%20and%20irinotecan. Accessed September 30, 2019.
18. U.S. Food and Drug Administration. FDA grants accelerated approval to ipilimumab for MSI-H or dMMR metastatic colorectal cancer. Available at: https://www.fda.gov/drugs/resources-information-approved-drugs/fda-grants-accelerated-approval-ipilimumab-msi-h-or-dmmr-metastatic-colorectal-cancer. Accessed September 30, 2019.
19. Voron T, Colussi O, Marcheteau E, et al. VEGF-A modulates expression of inhibitory checkpoints on CD8+ T cells in tumors. J Exp Med. 2015;212:139-48.
20. Triplett TA, Tucker CG, Triplett KC, et al. STAT3 signaling is required for optimal regression of large established tumors in mice treated with anti-OX40 and TGFβ receptor blockade. Cancer Immunol Res. 2015;3:526-35.
21. Schaer D, Li Y, Castaneda S, et al. Targeting the TGFβ pathway with galunisertib, a TGFβRI SMI, promotes anti-tumor immunity leading to durable, complete responses, as monotherapy and in combination with checkpoint inhibition. J Immunother Canc. 2015;3(2 suppl):P402.
22. Bittoni A, Sotte V, Meletani T, et al. Immunotherapy in colorectal cancer treatment: actual landscape and future perspectives. J Canc Metas Treat. 2018;4:55.
23. de’Angelis GL, Bottarelli L, Azzoni C, et al. Microsatellite instability in colorectal cancer. Acta Bio Med. 2018;89(9 suppl):97-101.
24. Carbognin L, Pilotto S, Milella M, et al. Differential activity of nivolumab, pembrolizumab, and MPDL3280A according to the tumor expression of programmed death-ligand-1 (PD-L1): sensitivity analysis of trials in melanoma, lung and genitourinary cancers. PloS One. 2015;10(6):e030142.
25. Galon J, Costes A, Sanchez-Cabo F, et al. Type, density, and location of immune cells within human colorectal tumors predict clinical outcome. Science. 2006;313:1960-64.
26. Mlecnik B, Bindea G, Angell HK, et al. Integrative analyses of colorectal cancer show immunoscore is a stronger predictor of patient survival than microsatellite instability. Immunity. 2016;44:698-711.
27. Segal NH, Saltz LB. Translational considerations on the outlook of immunotherapy for colorectal cancer. Curr Colorec Canc Rep. 2015;11:92-7.
28. Le DT, Hubbard-Lucey VM, Morse MA, et al. A blueprint to advance colorectal cancer immunotherapies. Cancer Immunol Res. 2017;5:942–9.
29. Long J, Lin J, Wang A, et al. PD-1/PD-L blockade in gastrointestinal cancers: lessons learned and the road toward precision immunotherapy. J Hematol Oncol. 2017;10:146.
30. Bendell J, Ciardiello F, Tabernero J, et al. Efficacy and safety results from IMblaze370, a randomized phase III study comparing atezolizumab+cobimetinib and atezolizumab monotherapy vs regorafenib in chemotherapy-refractory metastatic colorectal cancer. Ann Oncol. 2018;29(5 suppl):abstr LBA-004.
31. National Comprehensive Cancer Network (NCCN). Clinical practice guidelines in oncology (NCCN Guidelines): Colon cancer version 3. 2019. Available at https://www.nccn.org/professionals/physician_gls/recently_updated.aspx. Accessed October 1, 2019.
32. Lenz H-JJ, Cutsem EV, Limon ML, et al. Durable clinical benefit with nivolumab (NIVO) plus low-dose ipilimumab (IPI) as first-line therapy in microsatellite instability-high/mismatch repair deficient (MSI-H/dMMR) metastatic colorectal cancer (mCRC). Ann Oncol. 2018;29 (8 suppl):abstr LBA18_PR.
33. Chalabi M, Fanchi LF, Van den Berg JG, et al. Neoadjuvant ipilimumab plus nivolumab in early stage colon cancer. Ann Oncol. 2018;29 (8 suppl):abstr LBA37_PR.
34. Le DT, Durham JN, Smith KN et al. Mismatchrepair deficiency predicts response of solid tumorsto PD-1 blockade. Science 2017;357:409–413
35. Overman MJ, Lonardi S, Wong KYM et al.Durable clinical benefit with nivolumab plusipilimumab in DNA mismatch repair-deficient/microsatellite instability-high metastatic colorec-tal cancer. J Clin Oncol 2018;36:773–779.
36. Boland PM, Hutson A, Maguire O, et al. A phase Ib/II study of cetuximab and pembrolizumab in RAS-wt mCRC. J Clin Oncol. 2018;36 (4 suppl):abstr 834.
37. Hochster HS, Bendell JC, Cleary JM, et al. Efficacy and safety of atezolizumab (atezo) and bevacizumab (bev) in a phase Ib study of microsatellite instability (MSI)-high metastatic colorectal cancer (mCRC). J Clin Oncol. 2017;35 (4 suppl):abstr 673.
38. ClinicalTrials.gov. An investigational immuno-therapy study of nivolumab, and nivolumab in combination with other anti-cancer drugs, in colon cancer that has come back or has spread (CheckMate142). Available at: https://clinicaltrials.gov/ct2/show/NCT02060188. Accessed October 1, 2019.

How Supportive Care Methods Can Improve Oncology Outcomes
Experts discussed supportive care and why it should be integrated into standard oncology care.