(P094) Retrospective Analysis of Patients With Locally Advanced Unresectable Pancreatic Cancer (LAUPC) Treated With Chemotherapy Alone or Chemotherapy Combined With Radiation Therapy: The Indiana University Simon Cancer Center (IUSCC) Experience
A retrospective study was performed to investigate potential prognostic indicators and evaluate treatment outcomes in patients diagnosed with locally advanced unresectable pancreatic cancer (LAUPC), treated with chemotherapy alone (C), concurrent chemoradiation therapy (CRT), induction C followed by concurrent chemoradiation (C-CRT), CRT followed by chemotherapy (CRT-C), or C-CRT followed by C (C-CRT-C).
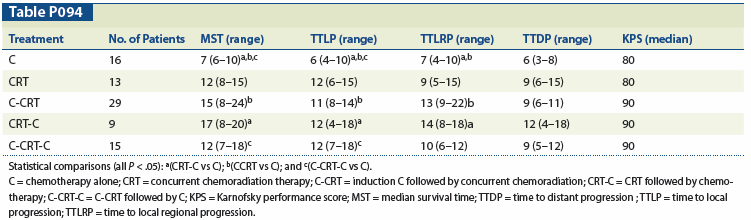
Table P094
Geoffrey L. Ray, MD, Edward Mannina, MD, MPH, MS, Sandra Althouse, MS, Higinia R. Cardenes, MD, PhD; Indiana University Simon Cancer Center, Indiana University School of Medicine
Purpose: A retrospective study was performed to investigate potential prognostic indicators and evaluate treatment outcomes in patients diagnosed with locally advanced unresectable pancreatic cancer (LAUPC), treated with chemotherapy alone (C), concurrent chemoradiation therapy (CRT), induction C followed by concurrent chemoradiation (C-CRT), CRT followed by chemotherapy (CRT-C), or C-CRT followed by C (C-CRT-C).
Patients and Methods: Medical records from 82 patients (38 women and 44 men) with a mean age of 61.8 years (range: 38–81 yr) diagnosed with LAUPC between January 19, 2000 and May 11, 2012 were reviewed and analyzed. All patients were initially evaluated by a pancreatic surgeon to determine resectability. Tumor locations include the head (71%), body (18%), and other (11%) sites of the pancreas. The majority of the patients (n = 78) received gemcitabine C, and for patients receiving radiation therapy (RT), the median radiation dose was 5,000 cGy. All but one patient had a Karnofsky performance score (KPS) above 70. Primary endpoints were median survival time (MST), time to local progression (TTLP), time to local regional progression (TTLRP), and time to distant progression (TTDP), calculated from the time of diagnosis. Baseline patient characteristics regarding age, race, gender, performance status, smoking history, and initial CA 19-9 and tumor characteristics were also included in the analysis.
Results: Median follow-up for all patients was 12 months (range: 9–15 mo). No significant findings were noted regarding patient baseline characteristics with respect to MST, but African Americans had lower TTDP compared with whites: 4 (range: 1–9) vs 9 (range: 7–11) months (P = .02). The following table demonstrates the outcomes with respect to primary endpoints (in months) for each treatment group. All CRT arms had improved outcomes over C alone.
Conclusions: In this single-institution experience, chemoradiation therapy plus pre-CRT and/or post-CRT chemotherapy significantly improved MST, TTLP, and TTLRP compared with chemotherapy alone. However, given the limited number of patients, the various chemotherapy agents used, and the limitations of a retrospective review, further investigation is needed in determining the most appropriate treatment regimen in patients diagnosed with LAUPC.