Considerations in the Care of Non–Small-Cell Lung Cancer: The Value Imperative
This article discusses ways in which the oncologist can incorporate value into the management of patients with lung cancer and comply with the underlying principles of the Choose Wisely Campaign, as well as recent ASCO and ESMO initiatives, to bend the cost curve downwards while maintaining efficacy.
Oncology (Williston Park). 32(11):534-40.

Ronan Kelly, MD, MBA

Stefanie Houseknecht, PharmD, BCOP

Table 1. FDA Approvals for Lung Cancer Indications, 2014–2018
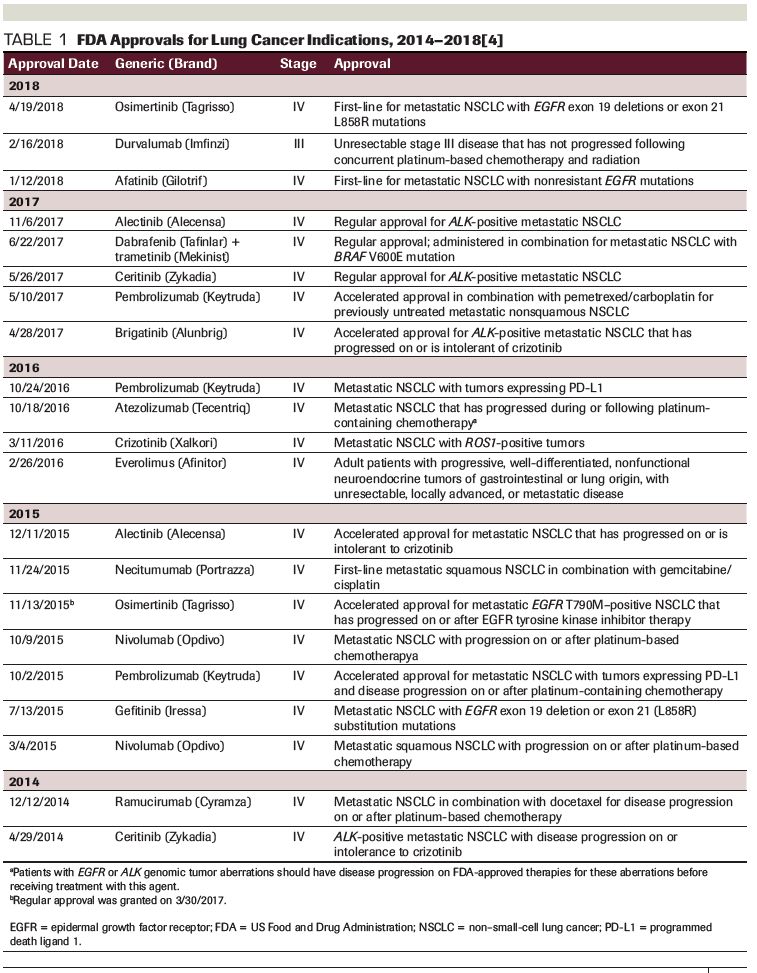
Table 2. Cost Comparison of Targeted Therapies for the Treatment of NSCLC
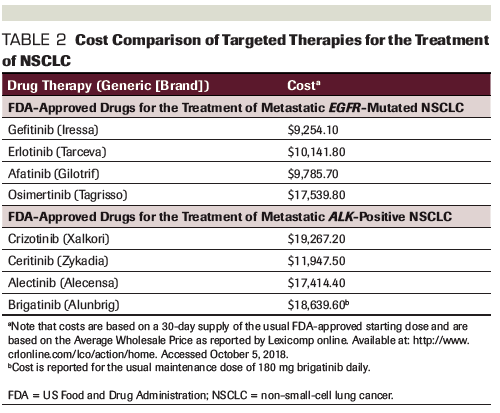
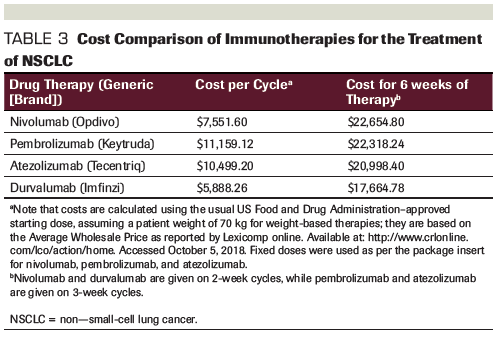
Table 3. Cost Comparison of Immunotherapies for the Treatment of NSCLC
Cancer costs in the United States continue to escalate at an alarming and unsustainable rate. These costs are not driven exclusively by a higher demand for services or by an aging population; rather, a number of systemic failures, highlighted by the Institute of Medicine (IOM), continue to plague our cancer care delivery systems and need to be rectified. Drug costs, plus expensive diagnostic tests, hospital admissions/readmissions, and unreasonable end-of-life care, combine to inflate the total cost of care. Cancer, particularly lung cancer, is one of the most expensive diseases in the United States. While individual oncologists are unlikely to influence costs in the short term, they can become more proficient at evaluating the value derived from new treatment options and maximizing the clinical benefit for their patients. Discussions of cost and patient values need not hinder patient-physician relationships, and, in fact, can strengthen them. This article discusses ways in which the oncologist can incorporate value into the management of patients with lung cancer and comply with the underlying principles of the Choose Wisely Campaign, as well as recent American Society of Clinical Oncology and European Society for Medical Oncology initiatives, to bend the cost curve downwards while maintaining efficacy.
Introduction
Lung cancer is the leading cause of cancer-related mortality in the United States, with an estimated 234,030 new cases and 154,050 deaths anticipated in 2018.[1] It is also a high-cost disease state throughout the continuum of care. In 2017, the total cost of care associated with lung cancer in the United States was estimated at $13.9 billion, with approximately 43% ($6 billion) of costs occurring during initial care and 41% ($5.8 billion) occurring within the last year of life.[2] These numbers are expected to increase as cancer drug costs rise and utilization of treatment increases, especially in the last year of life.[3] Recent data have demonstrated that the mean total and net monthly costs of medical care are consistently higher for lung cancer compared with breast cancer, prostate cancer, and colorectal cancer, regardless of the patient’s stage of disease or age.[3]
The management of non−small-cell lung cancer (NSCLC) has changed dramatically over the last decade: personalized, biomarker-driven therapeutics and immunotherapy-most notably, checkpoint inhibitors-have helped improve patient survival, safety, and quality of life. Table 1 lists all therapies indicated for the treatment of lung cancer that have been approved by the US Food and Drug Administration over the past 5 years.[4] While nearly every therapy listed in Table 1 demonstrated an improvement in progression-free survival (PFS) when compared with the existing standard, a substantial increase in costs also occurred. This trend is not sustainable, and many countries outside of the United States have not approved expensive medicines based on cost-efficacy analyses, with each jurisdiction determining the acceptable threshold level in terms of dollars per quality-adjusted life-year gained. In the United States, clinical pathways are becoming the norm in an attempt to standardize decision making and to improve therapeutic selection and care delivery. While data show pathways can help decrease costs in lung cancer, it is likely that US authorities will also implement some form of value-based pricing in the years ahead to help control drug price escalation.
Cost of Care: Just How Bad is the Problem?
Increasing awareness about therapy pricing
Most physicians do not know the cost of the drug therapies they prescribe. Even fewer know how much their patients are responsible for paying. The first step in reducing financial toxicity for both patients and the country as a whole is to increase awareness of drug costs. Two of the fastest growing drug classes in cancer are tyrosine kinase inhibitors (TKIs) and checkpoint inhibitors, both of which have seen new drug approvals or new indications for lung cancer (Table 1). The cost of these therapies is highly variable and dependent on the payer. For example, the price paid by a private practice oncology clinic for pembrolizumab differs from the price paid by a 340B drug pricing program−eligible clinic.
Although it may have limitations, and potentially represents the high end of the drug price range, the average wholesale price (AWP) can serve as a starting point for oncologists seeking to become better informed about drug prices. The AWP is readily available to the medical community and can often assist with price comparisons among agents within a drug class. Table 2 and Table 3 list the AWPs of commonly prescribed drugs for the treatment of lung cancer. It is important that oncologists treating patients with lung cancer become familiar with these numbers in order to better manage patients’ financial burden and out-of-pocket expenses.
At-risk populations
One particularly vulnerable patient population is Medicare beneficiaries: precisely the demographic most often diagnosed with lung cancer. In our experience, few oncologists understand Medicare Part D drug coverage. In addition, policies that have been created to help address out-of-pocket expenses for Medicare beneficiaries have not been as successful as intended. For example, the Affordable Care Act mandated the closing of the Part D coverage gap, better known as the “doughnut hole,” by decreasing patient cost-sharing from 100% in 2010 to 25% in 2020 for drug spending above $2,960, until the patient reaches $4,700 in out-of-pocket spending. While this might sound like a win for patients, an analysis of patient costs for oral anticancer therapies revealed that out-of-pocket costs will remain high after the hole closes, with an average of $5,663 annually across anticancer drugs.[5]
As one example, the estimated out-of-pocket expenditure for a Medicare Part D beneficiary (who does not qualify for low-income subsidies) prescribed crizotinib in 2010 was $9,120. After the gap closes in 2020, the annual out-of-pocket expense is estimated at $6,552, representing a savings of $2,568. This is based on the assumption that drug prices remain relatively stable, which is unlikely. If drug prices increase by 50% from 2014 to 2020, the estimated savings after closure of the gap in 2020 is reduced to just $203.[5] Given financial burdens, such as the scenario illustrated above with crizotinib, it is not surprising that financial toxicity is of real concern to patients prescribed oral anticancer therapies, and it deserves our attention.
Lung cancer patients prescribed oral therapies are not the only at-risk population, however. Individuals with Medicare Part B coverage receiving intravenous drug therapy for the treatment of their cancer may also face potentially high out-of-pocket expenses, especially those who do not have a supplemental or Medigap plan or do not qualify for low-income subsidies. Medicare Part B plans allow for cost-sharing, with patients responsible for 20% of the Medicare-approved amount. As drug costs rise, the complexity of regimens increases, and patients live longer, the cumulative cost of care grows. The most recent National Comprehensive Cancer Network (NCCN) guidelines for NSCLC give a category 1 recommendation to the regimen of atezolizumab, bevacizumab, carboplatin, and paclitaxel for the treatment of patients with advanced adenocarcinoma and an ECOG performance status score of 0–1.[6] This was based on the results of the IMpower150 trial.[7] This regimen costs approximately $20,500a for one cycle, and could have an estimated out-of-pocket cost as high as $4,100 per cycle for a Medicare Part B patient with no supplemental insurance. While adherence to intravenous therapy can be directly observed, a patient may need to make significant financial sacrifices in other aspects of his/her life in order to pay for this therapy.
Adverse consequences of cost-sharing
Recent data exploring the subjective financial toxicity to cancer patients found that 20% of 254 evaluated individuals reported taking less than the prescribed amount of medication due to concerns about cost.[8] Additionally, another 19% filled only part of a prescription, and 24% avoided filling the prescriptions at all as a strategy to cope with the cost of cancer care expenses. Although this patient cohort included predominantly breast cancer patients, it illustrates the unintended adverse consequences of cost-sharing that could ultimately result in higher healthcare costs downstream.
Approaching Value in Cancer Care
Follow the evidence
With costs of cancer care increasing precipitously, what can oncologists do? Several simple and practical solutions can help maximize the clinical benefit of therapy at an affordable price.[9] First, physicians should do only what is backed by robust clinical evidence. For tests or procedures, ask, “Will the results from this test or procedure change the treatment that is offered for my patient or significantly reduce symptoms or pain/suffering?” In other words, ensure that the pursuit is not purely academic.
In the treatment of lung cancer, a relevant example is the role of next-generation sequencing (NGS) panels, several of which are currently available in the United States. These testing platforms can identify mutations in more than 300 genes in tumor DNA, as opposed to limited-panel polymerase chain reaction−based tests, which evaluate mutations in a single gene. At the 2018 American Society of Clinical Oncology (ASCO) Annual Meeting, researchers reported that using NGS to test for all known lung cancer−related gene changes (EGFR, ALK, ROS1, BRAF, MET, HER2, RET, and NTRK1) at the time of diagnosis was less costly and faster than sequentially testing one or a limited number of genes at a time.[10] Commercially available treatment options exist for lung cancer patients with EGFR, ALK, ROS1, and BRAF mutations, and NCCN guidelines currently recommend treatment with oral therapies that are directed against these mutations.[6] Ongoing clinical trials for other mutations, including MET, HER2, RET, and NTRK1, are underway to test investigational agents against these targets. The authors of the study reported that their model estimated a potential savings of as much as $2.1 million for Medicare and more than $250,000 for commercial insurance providers. In addition, patients initiated appropriate therapy > 2.5 weeks sooner when mutations were found by NGS vs sequential or exclusionary testing.[10]
Bruce Pyenson, FSA, MAAA
Principal & Consulting Actuary, Milliman, Inc, New York, New York
We Need All on Board
Kelly and Houseknecht have done a great service by so clearly addressing how treatment costs affect lung cancer patients-and what oncologists can do about it. The United States spends much more than any other country on healthcare, often with worse outcomes.[1] Healthcare is drawing down the nation’s wealth and its citizens without returning the value it should.
One potential bright spot has been the proven use of lung cancer screening to detect lung cancers at early, highly curable stages. Screening has proven to be cost-effective by modeling teams who used different methods, assumptions, and even national settings.[2] The increasing prices of biologic agents and chemotherapies referenced by the authors make screening even more attractive, because these expensive therapies are focused on the late-stage, high-mortality disease that screening prevents.[3] Yet, lung cancer screening, which could save tens of thousands of lives a year, remains a rare procedure.[4]
Intense pressure to reduce costs is surely coming. Medicare’s Oncology Care Model created financial incentives for better quality and lower cost per chemotherapy episode, and participation was nearly double the targeted number of practices.[5,6] Medicare’s experiments in bundled payment (for example, setting episode budgets that include inpatient, outpatient, professional, and post-acute care) and accountable care have led to widespread program changes by payers. But a bigger force for change is likely to come from patients, their families, and the tens of millions of Americans whose opportunities and savings are being siphoned away to pay for low-quality healthcare and expensive insurance.
Kelly and Houseknecht’s recommendations point to how patients and oncologists can have better outcomes. Of course, oncologists, by themselves, can’t turn today’s medical inflation into deflation, but they may be able to ameliorate financial toxicity for some of their patients. We’ll have better healthcare when the whole system gets on board.
REFERENCES1. Medicare Payment Advisory Commission (MedPAC). Report to the Congress: Medicare Payment Policy. http://www.medpac.gov/docs/default-source/reports/mar18_medpac_entirereport_sec.pdf. Accessed October 15, 2018.
2. Pyenson B, Henschke E, Yankelevitz DF. Population health’s unanimity on lung cancer screening: far ahead of medical advice. Ann Transl Med. 2017;5:355.
3. American Cancer Society. Treatment choices for non-small cell lung cancer, by stage. https://www.cancer.org/cancer/non-small-cell-lung-cancer/treating/by-stage.html. Accessed October 15, 2018.
4. American Cancer Society. Lung cancer screening rates remain low. https://www.cancer.org/latest-news/lung-cancer-screening-rates-remain-low.html. Accessed October 15, 2018.
5. Centers for Medicare & Medicaid Services. Oncology Care Model overview. https://innovation.cms.gov/Files/slides/ocm-overview-slides.pdf. Accessed October 15, 2018.
6. Centers for Medicare & Medicaid Services. Oncology Care Model (OCM) request for applications (RFA). February 2015. https://innovation.cms.gov/Files/x/ocmrfa.pdf. Accessed October 15, 2018.
FINANCIAL DISCLOSURE:Mr. Pyenson performs actuarial analytics for Visiongate and Medical Imaging and Technology Alliance.
Another appropriate use of mutation testing is prior to considering osimertinib for the treatment of EGFR-mutated metastatic NSCLC progressing on a first- or second-generation EGFR TKI. The data currently support the use of osimertinib when the T790M mutation is detected and is believed to be the driver of progression on current therapy. When T790M is found, the response rate to second-line osimertinib is 71%, and the median PFS is 10.1 months.[11] However, if T790M is not detected, the response rate to osimertinib is 21% (median PFS, 2.8 months), and this is largely driven by patients who received chemotherapy in the interim.[12] Patients who went directly from a first- or second-generation EGFR TKI to osimertinib with no detectable T790M mutation had a response rate of 11% vs 36% if the therapy immediately prior to osimertinib was not an EGFR TKI. One could make the argument that, for T790M-negative patients, $17,539.80b per month of therapy for an 11% response rate is not a good value. Instead, these patients may be better served by enrolling in a clinical trial or starting chemotherapy.
Inappropriate use of NGS panels includes testing of patients with a low probability of detecting a targetable mutation, such as patients with squamous histology and an extensive smoking history, as well as those with performance status scores that preclude further active treatment. Without specialization in a given disease state within oncology, it can be difficult to interpret the results of molecular testing, and more difficult still to make treatment decisions for a given patient as it pertains to the use of a targeted therapy, with little to no evidence of efficacy in the patient’s disease.
Engage the patient
Physicians should involve patients in the discussion of value and cost. This initiative, established by ASCO over a decade ago, was only recently well defined in the ASCO Value Framework.[13] Conversations with patients should include expected outcomes in terms of median PFS, as well as toxicities that are likely to occur and their associated morbidity. As much as possible, the oncologist should also include costs-both total and out-of-pocket-that are likely to be incurred from the chosen treatment, as well as those associated with alternative treatments.
It is important to remember that additional months of PFS is not always the endpoint most valued by the patient. Patient-defined value incorporates the needs, values, and preferences of the patient.[14] For example, a young lung cancer patient with children approaching college may not want to incur additional costs of therapy, at the expense of reducing money available for his or her children’s higher education, if life expectancy is unlikely to differ by more than a few months regardless of the chosen treatment. Similarly, another patient may refuse a treatment that will require him to tap into retirement funds because he prefers to use available funds to travel with his spouse.
One major factor limiting the utility of these discussions is the lack of data on patient-reported outcomes and quality of life, which can help oncologists better consider the factors most important to patients.[14] Knowing which cancer-related symptoms are likely to improve with a given therapy and then assessing the global change in quality of life, which is affected by the toxicity of a treatment, can give patients valuable insights into the benefit of a prospective treatment.
Tips for cost-of-care discussions
Incorporating cost-of-care conversations into clinical practice may seem daunting, but it can become routine with a few simple strategies. First, take action by initiating such a discussion with patients. Research has shown that cost conversations may not be as harmful as previously thought.[15] A bigger threat to the patient-physician relationship is pretending that cost of care does not matter. Additionally, a recent study challenges the notion that such conversations are too time-consuming: the median duration of a cost-of-care discussion at a breast oncology clinic was 33 seconds, out of a median appointment time of 12 minutes and 2 seconds.[16]
Do your homework
Secondly, do a little homework. If you know that a clinic visit will focus on pain management, ask a support staff member to provide a list of formulary agents for a given patient’s insurance plan prior to the visit. Formularies are available online, and obtaining a copy of a patient’s most updated medical and prescription insurance card should be a common practice for all new patients. Make this information available to patients during the discussion; it does little good to discuss a therapy that may be financially unobtainable. If your clinic has financial counselors, this may be a good time to utilize such services in order to offer the most value possible. For example, you might ask the counselors to prepare a quick financial comparison of the direct costs associated with two proposed intravenous treatment regimens, which you can then share with the patient. For practices with onsite specialty pharmacies, this can be done for oral therapies as well.
As one example of the potential impact these steps can have, we recently ran test claims for both oral topotecan and oral temozolomide for a patient with relapsed/refractory small-cell lung cancer. Because this patient had Medicare Part B with no supplemental insurance, he was responsible for 20% coinsurance, and the out-of-pocket cost for a cycle of topotecan was nearly 10-fold higher than that of temozolomide (> $1,000 for topotecan vs ~$100, respectively). Both options, along with a discussion of the expected treatment benefit, toxicities, and dosing schedules, were presented to the patient during the clinic visit. Resources from several manufacturers are available, even to small practices with no onsite pharmacy, to assist with benefits investigations and to enroll patients in copay or financial assistance programs. Two such programs are AstraZeneca Access 360™ (https://www.myaccess360.com/patient/patient-unbranded/home.html) and Takeda Oncology 1Point™ (https://www.takedaoncology1point.com/patient/home). Make applicable forms available to patients during the first encounter in which drug recommendations take place. While it is not realistic to be able to identify all financial pitfalls, it is important to let patients know that alternatives to any treatment choice are available. Make sure your patients know that they can notify the care team if they encounter financial hurdles.
Finally, clinicians should incorporate periodic self-assessments into their practice to provide feedback on prescribing patterns and outcomes. These assessments could include denials from insurance companies, the frequency of chemotherapy/immunotherapy/targeted therapy administration in the last 2 weeks of life, and the rates of toxicities that result in hospitalization or loss of life. The latter cannot be understated, as clinical trial outcomes differ from real-world experience when patients who might not be perfect fits for clinical trial inclusion are treated off-protocol. For example, an oncologist might evaluate the incidence of hospitalizations for immune-related adverse events in her practice and ask, “Are patients being adequately screened for consideration of immunotherapy, such as identification of preexisting autoimmune conditions?” One area of interest in our practice is the incidence of pneumonitis in the real world (outside of the PACIFIC trial) when treating patients with durvalumab as consolidation following curative-intent concurrent chemoradiation. In our case, we asked, “How can we better identify patients who are developing pneumonitis, educate these patients, and initiate prompt treatment with steroids to avoid unnecessary morbidity and mortality?” When self-assessment is incorporated into practice, oncologists can improve outcomes for patients and reduce healthcare expenditures.
A Brief Word on Clinical Pathways
The IOM estimates that approximately 30% of all healthcare dollars are spent on unnecessary tests, procedures, and doctor visits.[17] Clinical pathways are one proposed way to streamline patient management and reduce costs. Pathways are a subset of guidelines designed to standardize care with best evidence, while reducing unwarranted variability and cost.[18] Developers of clinical pathways claim that a given pathway is chosen based on three factors: efficacy, toxicity, and cost. However, in lung cancer, it is rare for therapy options to have equal efficacy and toxicity, such that the sole deciding factor is cost. One of the best-known studies supporting the use of clinical pathways performed in NSCLC comes from the US Oncology Network. In this study, researchers reported no difference in overall survival for patients treated in the adjuvant or in the first- or second-line metastatic setting when treated on or off their level one pathway; however, costs were reduced by 35% in those treated on vs off their pathway.[19] Little data exist to determine whether clinical pathways make care more affordable for patients.
Despite their shortcomings, clinical pathways have the potential to improve patient care in lung cancer. Standardization of diagnostic procedures, including imaging and molecular testing, could streamline the screening for patients eligible for clinical trials. Pathways might also serve as a springboard for discussions with patients. Many patients are influenced by direct-to-consumer advertising by drug manufacturers, and nearly all patients with lung cancer ask their oncologist whether they are a candidate for immunotherapy. As an academic medical center seeing a fair share of second-opinion referrals from the community, we have seen several EGFR mutation−positive metastatic lung adenocarcinoma patients with intermediate to high programmed death ligand 1 (PD-L1) expression who are started on single-agent immunotherapy off-trial in the first-line setting. This practice is not evidence-based, and it potentially confuses assessment of toxicity when EGFR TKI therapy is initiated. In addition to being costly, this practice could also limit the patient’s clinical trial options in the future.
Conclusion
While the future of reimbursement paradigms in the United States remains uncertain, it is undeniable that the current state of escalating healthcare costs, especially in lung cancer, is unsustainable. The Affordable Care Act contained a number of government programs that are attempting to bend the cost curve by incentivizing providers to deliver high-quality care in a cost-effective manner. Among these programs is the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA), which includes the Quality Payment Program (QPP), made up of the Merit-based Incentive Payment System (MIPS) and Alternative Payment Models (APMs). These programs seek to enhance the quality of care, while improving patient outcomes and cost efficiency. Starting in 2019, US physicians will receive more or less reimbursement from the Centers for Medicare and Medicaid Services (CMS), depending on how they compare with their peers in quality and in value. Clinicians who adopt a quality-driven practice model now, regardless of the timelines imposed by the CMS, will be better prepared for the changes to come.
Change is hard, and harder still when the mentality of many patients has been, and continues to be, to do everything possible to prolong life, no matter the cost. Engaging patients in candid discussions about quality and cost throughout the spectrum of cancer care will lead to greater patient satisfaction, and lay the foundation for a more value-conscious healthcare culture. Returning healthcare to a patient-centered approach in the United States requires a commitment on the part of physicians to ask and to listen. This is especially important in the rapidly evolving field of lung cancer, where it can be difficult to keep abreast of and assimilate new data. As stewards of some of the most expensive therapies in healthcare, oncologists are ideally suited to lead the way.
aCost is based on the AWP as published by Lexicomp Online (accessed July 9, 2018) with the following assumptions: body surface area, 1.8 m2; weight, 70 kg; and creatinine clearance by means of Cockcroft and Gault equation, 100 mL/min. Prices for generic medications are an estimate of the AWP, as multiple prices are available and depend on the generic manufacturer used. One cycle of therapy represents atezolizumab 1200 mg, bevacizumab 15 mg/kg, paclitaxel 200 mg/m2, and carboplatin dosed at an area under the curve (AUC) of 6 using the Calvert formula. Cycle length is 21 days.
bCost is based on the AWP as published by Lexicomp Online (accessed July 9, 2018).
Financial Disclosure:Dr. Kelly reported that he receives clinical trial grant support from and is an advisory board member/consultant for AstraZeneca, Bristol-Myers Squibb, and Eli Lilly. He is also an advisory board member/consultant for Cardinal Health and Novartis. Dr. Houseknecht has no significant financial interest in or other relationship with the manufacturer of any product or provider of any service mentioned in this article.
References:
1. American Cancer Society. Cancer facts & figures 2018. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2018/cancer-facts-and-figures-2018.pdf. Accessed October 5, 2018.
2. National Cancer Institute. Cancer Trends Progress Report. Financial burden of cancer care. https://progressreport.cancer.gov/after/economic_burden. Accessed October 5, 2018.
3. Banegas MP, Yabroff KR, O’Keeffe-Rosetti MC, et al. Medical care costs associated with cancer in integrated delivery systems. J Natl Compr Canc Netw. 2018;16:402-10.
4. US Food & Drug Administration. Drugs@FDA. Hematology/oncology (cancer) approvals & safety notifications. https://www.fda.gov/drugs/informationondrugs/approveddrugs/ucm279174.htm. Accessed October 5, 2018.
5. Dusetzina SB, Keating NL. Mind the gap: why closing the doughnut hole is insufficient for increasing Medicare beneficiary access to oral chemotherapy. J Clin Oncol. 2016;34:375-80.
6. National Comprehensive Cancer Network (NCCN). Non-small cell lung cancer. https://www.nccn.org/professionals/physician_gls/pdf/nscl.pdf. Accessed October 5, 2018.
7. Socinski MA, Jotte RM, Cappuzzo F, et al; Impower150 Study Group. Atezolizumab for first-line treatment of metastatic nonsquamous NSCLC. N Engl J Med. 2018;378:2288-301.
8. Zafar SY, Peppercorn JM, Schrag D, et al. The financial toxicity of cancer treatment: a pilot study assessing out-of-pocket expenses and the insured cancer patient’s experience. Oncologist. 2013;18:381-90.
9. Kelly RJ, Smith TJ. Delivering maximum clinical benefit at an affordable price: engaging stakeholders in cancer care. Lancet Oncol. 2014;15:e112-e118.
10. Pennell NA, Mutebi A, Zhou Z, et al. Economic impact of next generation sequencing vs sequential single-gene testing modalities to detect genomic alterations in metastatic non-small cell lung cancer using a decision analytic model. Presented at the 2018 ASCO Annual Meeting; June 1-5, 2018; Chicago, IL. Abstract 9031.
11. Mok TS, Wu Y-L, Ahn M-J, et al. Osimertinib or platinum-pemetrexed in EGFR T790M-positive lung cancer. N Engl J Med. 2017;376:629-40.
12. Jänne PA, Yang JC, Kim DW, et al. AZD9291 in EGFR inhibitor-resistant non-small-cell lung cancer. N Engl J Med. 2015;372:1689-99.
13. Schnipper LE, Davidson NE, Wollins DS, et al. American Society of Clinical Oncology statement: a conceptual framework to assess the value of cancer treatment options. J Clin Oncol. 2015;33:2563-77.
14. Ersek JL, Nadler E, Freeman-Daily J, et al. Clinical pathways and the patient perspective in the pursuit of value-based oncology care. In: ASCO Educational Book. Vol 38. Chicago, IL: American Society of Clinical Oncology; 2017. p. 597-606.
15. Brick DJ, Scherr KA, Ubel PA. The impact of cost conversations on the patient-physician relationship. Health Commun. 2017 Oct 20. [Epub ahead of print]
16. Hunter WG, Zafar SY, Hesson A, et al. Discussing health care expenses in the oncology clinic: analysis of cost conversations in outpatient encounters. J Oncol Pract. 2017;13:e944-e956.
17. Institute of Medicine, Committee on the Learning Health Care System in America. Best care at lower cost: the path to continuously learning health care in America. In: Smith M, Saunders R, Stuckhardt L, McGinnis JM, eds. Washington, DC: National Academies Press (US); 2013.
18. Chiang AC, Ellis P, Zon R. Perspectives on the use of clinical pathways in oncology care. In: ASCO Educational Book. Vol 38. Chicago, IL: American Society of Clinical Oncology; 2017. p. 155-9.
19. Neubauer MA, Hoverman JR, Kolodziej M, et al. Cost effectiveness of evidence-based treatment guidelines for the treatment of non-small-cell lung cancer in the community setting. J Oncol Pract. 2010;6:12-8.