Rituximab: First Report of a Phase II Trial in NHL Patients With Bulky Disease
Rituximab (Rituxan) is the first monoclonal antibody (MoAb) approved for the treatment of non-Hodgkin’s lymphoma (NHL). This anti-CD20 MoAb is effective in inducing apoptosis, complement-dependent cytotoxicity (CDC), and antibody-dependent cellular cytotoxicity (ADCC). In single-agent studies in relapsed or refractory low-grade or follicular NHL (International Working Formula [IWF] types A-D), an overall response rate (ORR) of 48% has been reported.
Rituximab (Rituxan) is the first monoclonal antibody (MoAb) approved for the treatment of non-Hodgkins lymphoma (NHL). This anti-CD20 MoAb is effective in inducing apoptosis, complement-dependent cytotoxicity (CDC), and antibody-dependent cellular cytotoxicity (ADCC). In single-agent studies in relapsed or refractory low-grade or follicular NHL (International Working Formula [IWF] types A-D), an overall response rate (ORR) of 48% has been reported.
In this phase II trial, 31 patients (requiring treatment for progressive disease) with bulky low-grade or follicular NHL (³ 1 lesion ³ 10 cm) received rituximab at 375 mg/m² weekly × 4 infusions. Patient characteristics included: 52% male; median age, 55 years; median 4 years from diagnosis; and median three prior therapies.
Most related adverse events were mild to moderate (usually first infusionrelated): fever (61%), chills (36%), leukopenia (23%), nausea (19%), dizziness (19%), and throat irritation (19% of patients). Tumor lysis syndrome was not reported. Four patients had grade 3 or 4 nonhematologic adverse events: pulmonary (two patients), chills (one patient), and hypotension (one patient). One patient died with bronchiolitis obliterans 10 months posttreatment. Seven patients had a transient grade 3 or 4 hematologic adverse event: hemoglobin (three patients), absolute neutrophil count (ANC; six patients), and ANC + platelets (one patient). No patient developed a human antichimeric antibody (HACA) reaction. There were no grade 3 or 4 infections.
In evaluable patients, the ORR was 43% (12/28) with 1 complete response (CR) and 11 partial responses (PRs). The median time to progression (responders) was 8.1 months, with a median duration of response of 5.9 months. Of 12 responses, 3 are ongoing, with a maximum time to progression of 24.6+ months. B-symptoms resolved in 8/10 patients.
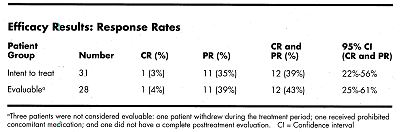
Exploratory analysis of prognostic factors revealed: 55% ORR in patients with IWF types B, C, D (12/22); higher MoAb levels in responders; and no correlation with number of relapses, number of prior chemotherapies, or chemoresistance.
CONCLUSION: Bulky disease is associated with poor prognosis in patients treated with chemotherapy (poor response, treatment-related mortality, short survival). Outpatient therapy (four infusions in 22 days) with rituximab is safe and effective in bulky low-grade or follicular NHL and does not limit subsequent treatment options.
Click here for Dr. Bruce Chesons commentary on this abstract.
How Supportive Care Methods Can Improve Oncology Outcomes
Experts discussed supportive care and why it should be integrated into standard oncology care.