Follicular Lymphoma: a Focus on Current and Emerging Therapies
This review article written by Kirk E. Cahill, MD, and Sonali M. Smith, MD, discusses standard and emerging therapies for the treatment of follicular lymphoma.
Abstract
Follicular lymphoma (FL) is the most common indolent lymphoma and is characterized by a relapsing and remitting course. In addition to significant biologic heterogeneity, the clinical trajectory for patients is variable, with some being observed for many years, and others having aggressive disease requiring multiple treatment courses. Unfortunately, FL remains incurable, and continues to cause early mortality. Improved understanding of the genetic and immune biology of FL has led to several FDA-approved therapies in the relapsed and refractory setting, including PI3K inhibitors; immunomodulatory agents; the EZH2 inhibitor, tazemetostat; and anti-CD19 chimeric antigen receptor (CAR) T-cell therapy, axicabtagene ciloleucel. This review outlines the current approach to the diagnosis and treatment of FL with a focus on emerging investigational therapies, including targeted protein inhibitors, antibody-drug conjugates, monoclonal antibodies, bispecific antibodies, and novel combination strategies.
Key Words: follicular lymphoma; treatment; novel therapies
Oncology (Williston Park). 2022;36(2):97-106.
DOI: 10.46883/2022.25920946
Introduction
Follicular lymphoma (FL) is an incurable B-cell lymphoid neoplasm with significant biological and clinical heterogeneity. As the most common indolent lymphoma and second most common non-Hodgkin lymphoma (NHL), it has a relapsing and remitting course with risk of transformation to aggressive disease.1,2 Most patients present with advanced disease and will eventually
require treatment for symptomatic disease. Given the range of clinical behaviors, the decision of when to treat is equally important as how to treat, noting that therapeutic goals include meaningful remission, symptom palliation, and prolongation of life.
While the majority of patients have survival approximating 2 decades, a subset of patients have aggressive disease with poor outcomes.3 Unfortunately, baseline identification of these patients remains challenging. Approximately 20% of patients with FL have progressive disease within 2 years of initial chemoimmunotherapy and a 5-year overall survival (OS) of 50%.4 Cumulative toxicity from repeated exposure to palliative cytotoxic chemotherapy also contributes to morbidity and mortality. While anti–CD20-based chemoimmunotherapy remains an important standard of care, more rational and biologically driven agents are either approved or in development. In this review, we examine the current approach to the diagnosis and treatment of FL with a focus on targeted therapy and other novel agents.
Current Standards for Diagnosis
A diagnosis of FL requires histologic examination of a lymph node biopsy for assessment of nodal architecture and grading.5 FL is characterized by neoplastic germinal center B-cells growing in densely packed follicles with distortion of the normal nodal architecture. Grading depends on the number of centroblasts/high-power field. Grade 1-3a are considered indolent, whereas 3b is more aggressive and clinically approached as diffuse large B-cell lymphoma (DLBCL).6 The classic immunophenotype includes the B-cell antigens CD19, CD20, and CD79a; lymphoid progenitor marker, CD10; and nuclear proteins, BCL-2 and BCL-6. Unlike mantle cell lymphoma and chronic lymphocytic leukemia/small lymphocytic lymphoma, it is negative for CD5.
Molecular Testing
Cytogenetically, FL is characterized by the translocation t(14;18), which occurs in up to 90% of cases, as a result of aberrant V(D)J recombination. This results in BCL-2 protein overexpression and increased cell survival (Figure 1).7 As a hallmark of FL, it is necessary, but alone insufficient, for lymphomagenesis.8-10 An important recent finding is early mutations in genes coding for chromatin modifying proteins.11-13 These ‘epimutations’ are a second hallmark of FL and include: KMT2D (~70-80%), CREBBP (~65-70%), EZH2 (~25%), and EP300 (~14%).12,14 These transcriptionally repressive mutations result in increased germinal center proliferation, differentiation block, and immune evasion.15-17 Along with the BCL2 translocation, these mutations are early events occurring in a common progenitor cell.
FIGURE 1. Genomic Hallmarks of FL
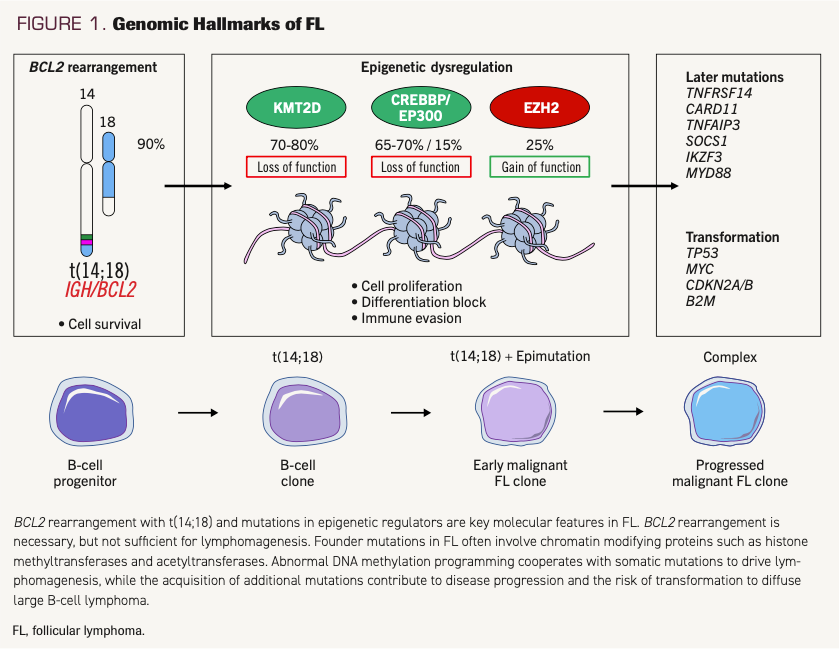
Through divergent clonal evolution, other mutations are subsequently acquired including mutations in genes involved in immune modulation (TNFRSF14); JAK-STAT signaling (STAT6, SOCS1); and B-cell receptor–NF-kB signaling (CARD11, TNFAIP3, MYD88).12 While conventional karyotyping and fluorescent in situ hybridization (FISH) for t(14;18) are part of the standard evaluation for FL, genomic sequencing is limited to testing for the EZH2 mutation when tazemetostat is being considered.18 Nonetheless, next-generation sequencing has revealed the diverse mutational landscape of FL and provides insight into disease pathogenesis, as well as opportunities for more precise therapeutic strategies.
Stratification for Treatment Selection
The treatment of FL must consider individual parameters and balance the risk of cumulative toxicity versus remission and palliation of symptoms. The conventional approach to FL is clinical observation until there is an indication to treat, typically based on criteria of the Groupe d’Etude des Lymphomes Folliculaires (GELF) or National Comprehensive Cancer Network (NCCN).19,20 There are several prognostic indices in FL including the Follicular Lymphoma International Prognostic Index (FLIPI), FLIPI-2, and m7-FLIPI, but none dictate the timing or type of treatment at an individual patient level.14,21,22
The m7-FLIPI and gene expression profiling panels include genomic features, but have varied performance and are not validated for clinical practice.23 Staging with positron emission tomography (PET) imaging helps to identify the extent of disease and preferred sites for biopsy when histologic transformation to DLBCL is suspected, as this occurs in up to 15% of patients.3 The assumption here is that higher uptake values correspond with more rapid cell turnover and aggressive histology. This is somewhat controversial, and PET alone does not appear to predict histologic transformation.24 Nonetheless, PET imaging does result in disease upstaging in approximately 10% to 60% of cases, which often has treatment implications.25,26
Therapy Selection
First-line Treatment
For patients with stage I-II disease, there are several options including observation, rituximab (Rituxan), chemoimmunotherapy, or radiation, with the majority of patients having similar excellent long-term survival regardless of initial approach.27 Approximately 70% of patients have advanced disease (stage III or IV) at diagnosis.3,28 Asymptomatic patients with low disease burden may be actively monitored. When treatment is indicated for patients with low tumor-burden advanced disease, rituximab monotherapy is often used, given the high overall response rate (ORR; complete remission [CR] plus partial remission [PR]) of 71%, low toxicity, and long median time to treatment failure of approximately 4 years, which delays the need for cytotoxic therapy.29
When selecting initial treatment for patients with high tumor burden and symptomatic advanced FL, there are several considerations regarding the chemotherapy backbone, the anti-CD20 antibody, the use of maintenance strategies, and whether to opt for a nonchemotherapy regimen (Figure 2). Based on the StiL (NCT00991211) and BRIGHT (NCT00877006) trials, bendamustine and rituximab (BR) or rituximab with cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP), are both options with ORR >90%.30,31
FIGURE 2. A Proposed Treatment Approach for Advanced-Stage FL
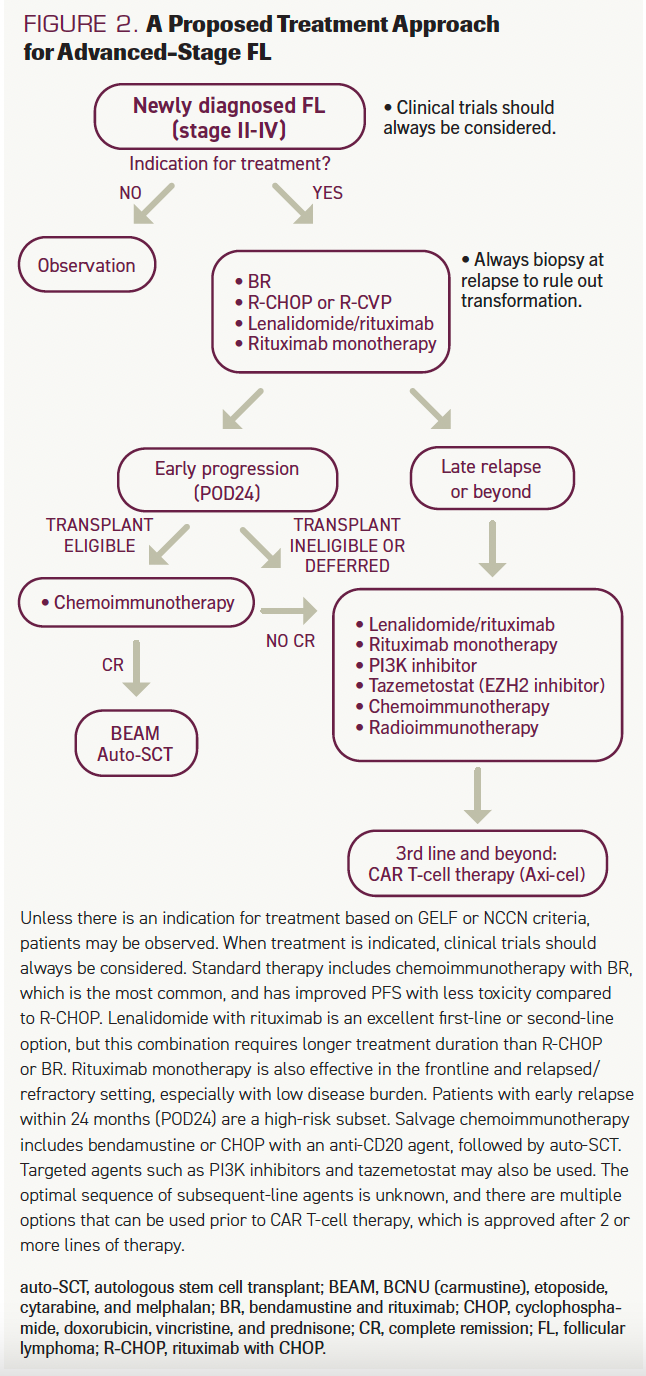
BR has become a preferred option based on superior progression-free survival (PFS) over R-CHOP (70 vs 31 months, respectively) and it is also not associated with alopecia, anthracycline-associated cardiotoxicity, vinca alkaloid-associated neuropathy, or steroid-associated risks. R-CHOP may be preferred in cases where occult transformation is suspected, or immune suppression associated with bendamustine is to be avoided. In patients treated with R-CHOP or rituximab with cyclophosphamide, vincristine, and prednisone (R-CVP), maintenance therapy with rituximab every
8 weeks for 2 years compared with placebo improves PFS, but not OS, based on the PRIMA study (NCT00140582).32
It is unclear whether this extends to patients treated with BR. In the GALLIUM study (NCT01332968), chemoimmunotherapy with obinutuzumab (Gazyva) versus rituximab improved PFS, with no difference in OS, but did result in high grade 3-5 adverse events, including infusion-related events and infections.33,34 The use of maintenance therapy is controversial, and even more so during the COVID-19 pandemic. Among surveyed physicians who treat indolent lymphomas with a maintenance therapy strategy, 53% hold rituximab maintenance to allow for vaccination.35 Lenalidomide (Revlimid)with rituximab is an alternative to chemoimmunotherapy with similar response rates, PFS, and OS to chemoimmunotherapy (R-CHOP, BR, or R-CVP).36 Similar to chemoimmunotherapy, it is a fixed-duration treatment, but with a much longer time frame at 18 months. It remains an option for patients wishing to avoid cytotoxic chemotherapy.
Relapsed/Refractory Treatment
There is no standard treatment or sequence of treatments for relapsed/refractory FL (RR-FL), but the number of options is increasing. Approximately 20% of patients have early relapse and progression of disease within 24 months (POD24), and these patients have poor outcomes.4 Unfortunately, upfront identification of these patients is not possible, and more effective treatments for these patients are needed. For all patients with RR-FL, a chemoimmunotherapy regimen (BR, R-CHOP, or R-CVP) different from the first-line therapy is an option.
There is limited data on R-CHOP after BR, but second-line BR in patients with indolent NHL with previous rituximab (39%) or CHOP (54%) had an ORR of 82% and PFS of 34 months.37 Rituximab monotherapy is also effective for some patients with low tumor burden and previous rituximab-based regimens with an ORR 55% to 64% and PFS of 14 months.38,39 Obinutuzumab with either bendamustine or CHOP may improve outcomes by overcoming rituximab refractoriness, especially for relapses within 6 to 12 months.40,41 In transplant-eligible patients with chemosensitive disease to first salvage, consolidative autologous stem cell transplantation (auto-SCT) appears to improve long-term survival based on several retrospective analyses.
Among patients with POD24, auto-SCT has an improved 5-year OS of approximately 77% vs 59% among those without auto-SCT.42 Similar results were observed for patients undergoing auto-SCT within 1 year of treatment failure, with a 5-year OS of 73% compared with 60% without auto-SCT.43 It should be noted, however, that the benefit of auto-SCT may simply be due to a favorable response to second-line therapy and randomized studies are needed.
In the era of increased alternative treatments, the use of auto-SCT has been substantially reduced. The use of allogeneic-SCT, a historical option with curative potential in FL, has also declined. While the preferred therapy for high-risk patients with early relapse has yet to be defined, targeted therapy beyond anti-CD20 monoclonal antibodies has been reshaping the treatment landscape of FL since 2014 (Table 1), with several new trials focusing on this population, including a US Intergroup Study S1608 (NCT03269669).
TABLE 1. Recent FDA-Approved Therapies for FL
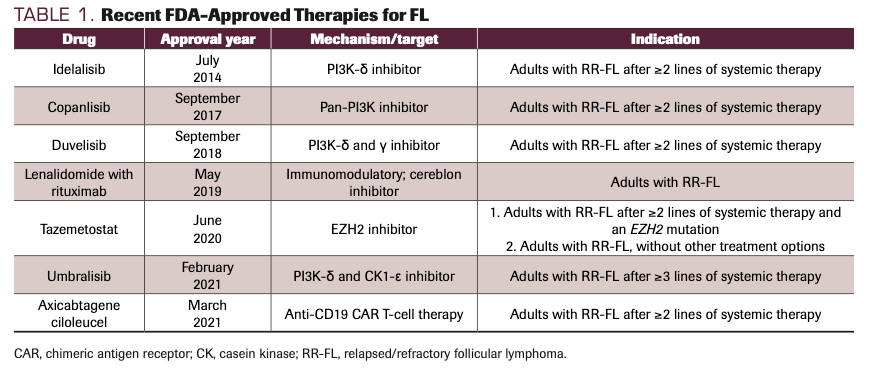
Lenalidomide
Lenalidomide is an immunomodulatory drug with direct cytotoxicity to lymphoma cells via inhibition of the E3 ubiquitin ligase, cereblon, as well as indirect antitumor effects mediated through changes in the tumor microenvironment.44 Lenalidomide with rituximab is an active regimen in rituximab-sensitive relapsed FL, as demonstrated in the AUGMENT trial (NCT01938001) with an ORR of 80% (CR 35%) compared with an ORR of 55% (CR 20%) for rituximab alone.39 The combination had a 2-year OS and median PFS of 95% and 39.4 months compared with 86% and 13.9 months, respectively, for rituximab alone. The combination had a higher incidence of all grades of infections (63% vs 49%, respectively), neutropenia (58% vs 23%), and cutaneous reactions (32% vs 12%). Of the grade 3 or 4 adverse events, a higher incidence of neutropenia (50% vs 13%) was also observed with the combination. This study led to the regulatory approval of lenalidomide with rituximab in patients with RR-FL.
PI3K Inhibitors
Inhibition of PI3K signaling has been a largely successful approach, with 4 FDA-approved agents in RR-FL.45 PI3K mediates proximal intracellular B-cell receptor signaling, as well as cell survival signals received from the tumor microenvironment. Idelalisib (δ isoform inhibitor; Zydelig) was the first of these agents to be approved and a major breakthrough in the RR-FL space. The ORR was 57% (CR 6%) with a median duration of response (DOR) of 12.5 months and median PFS of 11 months in very heavily pretreated patients.46 Unfortunately, significant toxicities, including neutropenia, diarrhea, transaminitis, and pneumonia, limited its development. Copanlisib (pan-isoform inhibitor; Aliqopa); duvelisib (δ and γ isoform inhibitor; Copiktra); and umbralisib (δ isoform and CK1 ε inhibitor; Ukoniq) are also approved for RR-FL with comparable efficacy and improved toxicity profiles.47-49 They all have an ORR ranging from 42% to 59%, median DOR of 10 to 12 months, and median PFS of 9.5 to 11 months. They have regulatory approval for patients with multiply relapsed FL, based on activity in the heavily pretreated setting.
Tazemetostat
Approximately 25% of patients with FL have a gain of function mutation in the histone methyltransferase protein, EZH2, with consequent increased expression of genes involved in cell proliferation.12,14,50 Although it contributes to lymphomagenesis, EZH2 gene mutations are associated with improved PFS.50 Tazemetostat (Tazverik) is an EZH2 inhibitor that targets this epimutation. It is the first biomarker-directed therapy in FL and has been approved as a third-line option in RR-FL, with an ORR of 69% and CR rate of 13%.51 With a median follow-up of 22 months, the median PFS was 13.8 months, and median OS was not reached. It also appears to have activity in patients without an EZH2 gene mutation, with ORR of 35% and similar median PFS and OS. There were few significant treatment-related adverse events, with 3% of patients having grade 3 or 4 myelosuppression and a low discontinuation rate of 8%. Its favorable toxicity profile makes it an attractive oral option.
Radioimmunotherapy
For patients with RR-FL, radioimmunotherapy (RIT) is an effective yet often underutilized treatment, especially in those unable to tolerate intensive therapy. RIT uses monoclonal antibodies bound to a radionuclide to deliver targeted cytotoxic radiation to lymphoma cells and the tumor microenvironment. 90Y-ibritumomab tiuxetan (90Y-IT, Zevalin) and 131I-tositumomab (131I-T, Bexxar) are anti-CD20 radioimmunoconjugates that were FDA approved in 2002 and 2003 for RR-FL, respectively.52,53 Unfortunately, the logistics of administration limited their initial uptake in clinical practice, and 131I-T was voluntarily withdrawn in 2013.54 90Y-IT remains commercially available. In a randomized study of patients with rituximab-naïve RR-FL, 90Y-IT vs rituximab had an ORR of 86% vs 55%, CR rate of 40% vs 17%, and a median DOR of 26.4 months vs 8.5 months in complete responders.55 In rituximab-refractory patients with RR-FL, the ORR was 74% (CR 15%) with a median DOR of 6.4 months.56 Approximately 60% of patients experienced grade 3/4 neutropenia or thrombocytopenia with duration of 1 to 4 weeks.52-55 Grade 3/4 infections occurred in approximately 7% of patients. 177Lu-lilotomab satetraxetan (177Lu-LS, Betalutin) is a novel anti-CD37 RIT with an ORR of 65% (CR 30%) and a median DOR of 13.6 months (32.0 months for complete responders) in early studies of patients with RR-FL.57 This is comparable to other targeted agents in this setting. The phase 2 LYMRIT-37-01 trial (NCT01796171) for patients with RR-FL with ≥2 lines of therapy including anti-CD20 based chemoimmunotherapy and the phase 1 LYMRIT-37-07 trial (NCT03806179) in those with ≥1 previous anti-CD20–based therapies will both provide more insight into the role of 177Lu-LS in the treatment of FL.
CAR T-Cell Therapy
While targeted agents have clinical activity in RR-FL, long-term remission is still lacking and most require prolonged treatment courses. CAR T-cell therapy has revolutionized the treatment of aggressive lymphomas like DLBCL, and is also now an option for RR-FL, although follow-up remains short. Axicabtagene ciloleucel (axi-cel; Yescarta) is an anti-CD19 CAR T-cell therapy that received accelerated approval in March 2021 for adult patients with RR-FL (≥ 2 lines of prior therapy) based on the results of the phase 2 study ZUMA-5.58 In a preliminary report of updated results (median follow-up of 31 months), 86 patients with RR-FL had an ORR of 94% (CR 79%), median DOR and PFS of 38.6 months and 39.6 months, respectively, while OS was not reached.59 The incidence of cytokine release syndrome (CRS) and neurotoxicity grade ≥ 3 were 6% and 15%, respectively.
The phase 2 ELARA trial (NCT03568461) evaluating tisagenlecleucel (tisa-cel) in patients with RR-FL (≥ 2 lines of prior therapy) had an ORR 86% (CR 69%) without any grade ≥ 3 CRS, and only 3% with grade ≥ 3 neurotoxicity.60 At a median follow-up of 16.9 months, the median DOR, PFS, and OS were not reached, but 1-year PFS was 67%. The phase 2 TRANSCEND FL trial (NCT04245839) using lisocabtagene maraleucel is ongoing. One of the most crucial challenges is patient selection for CAR T, which remains a costly and aggressive approach. Long-term follow-up and real-world data for CAR T-cell therapy from the commercial setting will be important guides influencing patient selection.
Emerging and Novel Therapies
Beyond the commercially approved targeted therapies in FL, there are multiple emerging agents that target the biology of FL (Figure 3). These are reviewed briefly in the following section, which also highlights novel investigational use of these treatments in FL (Table 2).
FIGURE 3. Approved and Investigational Targeted Agents in FL
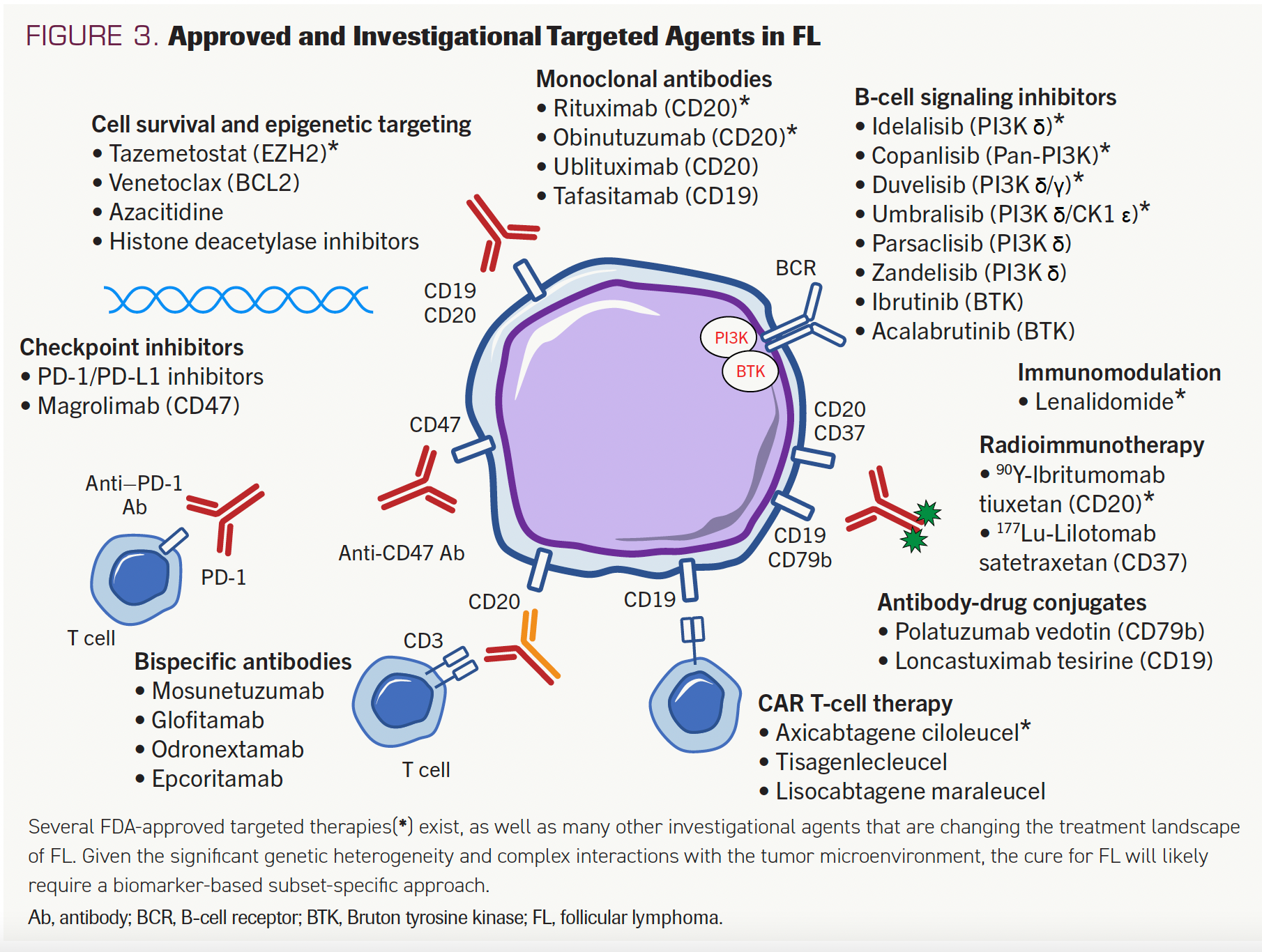
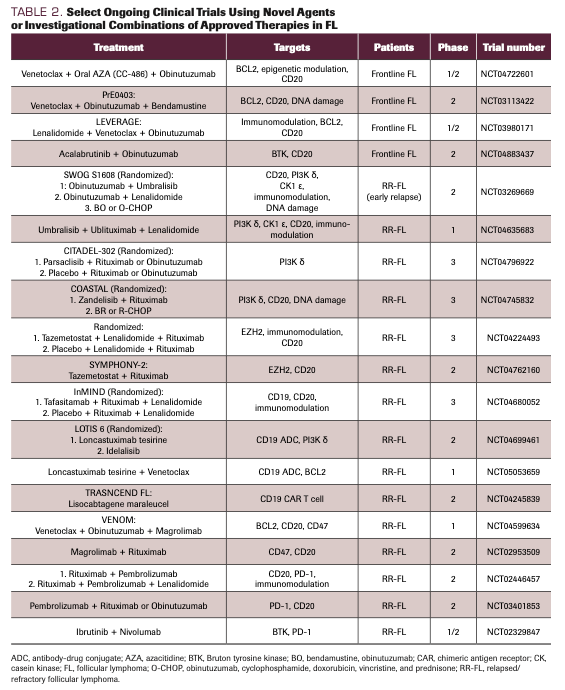
TABLE 2. Select Ongoing Clinical Trials Using Novel Agents or Investigational Combinations of Approved Therapies in FL
Antibody-Drug Conjugates
Antibody-drug conjugates (ADCs) offer an appealing means of antigen-based drug delivery, with several in development. In a phase 2 study in patients with RR-FL, the anti-CD79b ADC, polatuzumab vedotin, (pola; Polivy) was combined with rituximab and resulted in an ORR of 70% (CR 45%) with a 9.4-month DOR.61 The PFS was 15.3 months with a 2-year OS of 88%. The most common grade 3-4 adverse events were neutropenia (15%) and diarrhea (10%); however, although no grade 3-4 neuropathy was observed, 40% had grade 1-2 neuropathy.
In preliminary reports of early-phase studies evaluating pola combinations in RR-FL, pola with BR did not improve treatment response.62 Pola with obinutuzumab/lenalidomide had an ORR of 76% (CR of 65%), while pola with obinutuzumab/venetoclax had an ORR of 71% (CR of 57%), and long-term results with updated survival are anticipated.63.64 In a phase 1 study including 14 patients with RR-FL, the anti-CD19 ADC, loncastuximab tesirine (Zynlonta), had an ORR of 79% (CR of 65%), and cytopenias were the most common adverse effect.65
Checkpoint Inhibitors
Although checkpoint blockade monotherapy has low response rates in RR-FL, combinations may be more active. A phase 1/2 trial (NCT02631577) using obinutuzumab, atezolizumab (Tecentriq), and lenalidomide (G-atezo-len) in patients with RR-FL reported an ORR of 78% (CR of 72%), median DOR of 38 months, and 2-year PFS of 65%.66 Cytopenias were the most common grade ≥ 3 adverse event and occurred in 71% of patients. While the majority of toxicities were manageable, the discontinuation rate of any study drug was 29%.
In a preliminary report of pembrolizumab with rituximab in patients with RR-FL (NCT02446457), the ORR was 80% (CR of 60%), and although safe, the benefit of pembrolizumab (Keytruda) over rituximab monotherapy was unclear, as this trial included patients with rituximab-sensitive disease.67 In the frontline phase 2 trial (1st FLOR study; NCT03245021), immune priming with nivolumab (Opdivo), followed by rituximab and nivolumab had an ORR of 92% (CR of 54%), with a favorable toxicity profile.68 Larger studies and a longer follow-up are needed to clarify the role of checkpoint inhibitors as first-line nonchemotherapy options.
Novel Antibodies and Combinations
Antibodies with novel targets are also under investigation in FL. The anti-CD47 antibody, magrolimab (Hu5F9-G4), blocks CD47 on lymphoma cells to enhance macrophage-mediated phagocytosis. In a phase 1 study of patients with RR-NHL, which included 7 patients with RR-FL, magrolimab with rituximab resulted in an ORR of 71% (5/7) and CR rate of 43% (3/7).69 Although small, these numbers are encouraging, with many patients having rituximab-refractory disease. The phase 2 portion of this study (NCT02953509) is currently recruiting.
Another trial investigating venetoclax (Venclexta) with obinutuzumab and magrolimab (VENOM) in relapsed/refractory indolent lymphomas is recruiting, and the results are eagerly anticipated (NCT04599634). Tafasitamab (Monjuvi) is an anti-CD19 antibody approved in combination with lenalidomide for relapsed/refractory DLBCL, but has low activity as a monotherapy in FL.70 A phase 3 trial (InMIND) of tafasitamab plus lenalidomide/rituximab versus lenalidomide/rituximab alone in patients with RR-FL or marginal zone lymphoma will determine whether there is a role for tafasitamab in RR-FL (NCT04680052).
Bispecific Antibodies
Bispecific antibodies or bispecific T-cell engagers (BiTes) are novel protein constructs with separate B-cell (CD20) and T-cell targeting (CD3) domains. Mosunetuzumab, glofitamab, odronextamab, and epcoritamab are bispecific antibodies being investigated in early-phase RR-FL trials (Table 3), which have shown promising results with ORR ranging from 80% to 100% (CR from 50% to 75%) in heavily pretreated patients.71-75 Bispecific antibodies provide an off-the-shelf form of T-cell mediated therapy, with the goal of achieving the durable remissions seen with CAR T-cell therapy. Unlike CAR T-cell therapy, they appear to have a lower risk of CRS and neurotoxicity, and favorable responses in patients relapsing after CAR T-cell therapy. The optimal clinical use of bispecific antibodies remains unknown, and trials including novel combinations in FL are ongoing: mosunetuzumab and lenalidomide (NCT04246086); and epcoritamab with lenalidomide/rituximab or BR (NCT04663347).
BCL2 and Epigenetic Targeting
While BCL2 translocation and epigenetic dysregulation are both frequent features in FL, the efficacy of existing agents has been modest. The BCL2 inhibitor, venetoclax, had low monotherapy activity in FL with an ORR of 38% (CR of 14%),76 but combination strategies are in development. A preliminary report of the first trial to combine a Bruton tyrosine kinase (BTK) inhibitor, ibrutinib (Imbruvica), with venetoclax in RR-FL showed an ORR of 83% (CR of 33%) with manageable toxicity (NCT02956382).77 Several frontline trials using venetoclax-based combinations include the following: venetoclax, oral azacitidine (CC-486), and obinutuzumab (NCT04722601); venetoclax, lenalidomide, and obinutuzumab (NCT03980171); and venetoclax, ibrutinib, and obinutuzumab (NCT04450173).
The phase 2 PrECOG 0403 trial with frontline venetoclax, bendamustine, and obinutuzumab (NCT03113422) for patients with high tumor-burden FL (n = 56) showed an ORR of 93% (CR of 73%), 2-year estimated PFS of 86%, and 2-year estimated OS of 94% at a median follow-up of 21 months.78 Despite the efficacy, the rate of ≥ grade 3 adverse events was high, at 84%, most notably due to tumor lysis, cytopenias, and infections. Unfortunately, this toxicity will preclude its use, but alternative dosing strategies to mitigate adverse effects are being explored. Tazemetostat is also being evaluated in combination with rituximab (NCT04762160), and in combination with lenalidomide and rituximab (NCT04224493).
Conclusions
While chemoimmunotherapy, lenalidomide with rituximab, or rituximab alone are standard first or subsequent line options for advanced FL, the treatment choices for RR-FL have evolved over the last several years. Additional agents for multiply relapsed patients include PI3K inhibitors, tazemetostat, and CAR T-cell therapy. Patient selection for CAR T-cell therapy is evolving, and the optimal sequencing with other therapies remains unknown. There are many emerging investigational products, including ADCs, anti-CD47 monoclonal antibodies, bispecific antibodies, checkpoint-based therapy, and novel combination strategies that are being evaluated. Individualized approaches, trial end points with quality-of-life measures, and information to guide sequencing of available regimens and agents are all desperately needed. These efforts, coupled with ongoing discovery in the biology of FL, are imperative to improving outcomes for patients with FL.
AUTHOR AFFILIATIONS:
Kirk E. Cahill, MD1; and Sonali M. Smith, MD1
1Department of Medicine, Section of Hematology/Oncology, University of Chicago Medicine Comprehensive Cancer Center, Chicago, IL.
Funding: None
Corresponding author
Sonali M. Smith, MD; Elwood V. Jensen Professor in Medicine; Chief, Section of Hematology/Oncology; Department of Medicine; The University of Chicago Medicine; 5841 S. Maryland Ave., MC 2115; Chicago, IL 60637; Email: smsmith@medicine.bsd.uchicago.edu
References
- Link BK, Maurer MJ, Nowakowski GS, et al. Rates and outcomes of follicular lymphoma transformation in the immunochemotherapy era: a report from the University of Iowa/MayoClinic Specialized Program of Research Excellence Molecular Epidemiology Resource. J Clin Oncol. 2013;31(26):3272-3278. doi:10.1200/JCO.2012.48.3990
- Teras LR, DeSantis CE, Cerhan JR, Morton LM, Jemal A, Flowers CR. 2016 US lymphoid malignancy statistics by World Health Organization subtypes. CA Cancer J Clin. 2016;66(6):443-459. doi:10.3322/caac.21357
- Batlevi CL, Sha F, Alperovich A, et al. Follicular lymphoma in the modern era: survival, treatment outcomes, and identification of high-risk subgroups. Blood Cancer J. 2020;10(7):74. doi:10.1038/s41408-020-00340-z
- Casulo C, Byrtek M, Dawson KL, et al. Early relapse of follicular lymphoma after rituximab plus cyclophosphamide, doxorubicin, vincristine, and prednisone defines patients at high risk for death: an analysis from the National LymphoCare Study. J Clin Oncol. 2015;33(23):2516-2522. doi:10.1200/JCO.2014.59.7534
- Swerdlow SH, Campo E, Pileri SA, et al. The 2016 revision of the World Health Organization classification of lymphoid neoplasms. Blood. 2016;127(20):2375-2390. doi:10.1182/blood-2016-01-643569
- Vaidyanathan G, Czuczman MS. Follicular lymphoma grade 3: review and updates. Clin Lymphoma Myeloma Leuk. 2014;14(6):431-435. doi:10.1016/j.clml.2014.04.008
- Weiss LM, Warnke RA, Sklar J, Cleary ML. Molecular analysis of the t(14;18) chromosomal translocation in malignant lymphomas. N Engl J Med. 1987;317(19):1185-1189. doi:10.1056/NEJM198711053171904
- Limpens J, de Jong D, van Krieken JH, et al. Bcl-2/JH rearrangements in benign lymphoid tissues with follicular hyperplasia. Oncogene. 1991;6(12):2271-2276.
- Aster JC, Kobayashi Y, Shiota M, Mori S, Sklar J. Detection of the t(14;18) at similar frequencies in hyperplastic lymphoid tissues from American and Japanese patients. Am J Pathol. 1992;141(2):291-299.
- Roulland S, Navarro JM, Grenot P, et al. Follicular lymphoma-like B cells in healthy individuals: a novel intermediate step in early lymphomagenesis. J Exp Med. 2006;203(11):2425-2431. doi:10.1084/jem.20061292
- Morin RD, Mendez-Lago M, Mungall AJ, et al. Frequent mutation of histone-modifying genes in non-Hodgkin lymphoma. Nature. 2011;476(7360):298-303. doi:10.1038/nature10351
- Okosun J, Bodor C, Wang J, et al. Integrated genomic analysis identifies recurrent mutations and evolution patterns driving the initiation and progression of follicular lymphoma. Nat Genet. 2014;46(2):176-181. doi:10.1038/ng.2856
- Pasqualucci L, Dominguez-Sola D, Chiarenza A, et al. Inactivating mutations of acetyltransferase genes in B-cell lymphoma. Nature. 2011;471(7337):189-195. doi:10.1038/nature09730
- Pastore A, Jurinovic V, Kridel R, et al. Integration of gene mutations in risk prognostication for patients receiving first-line immunochemotherapy for follicular lymphoma: a retrospective analysis of a prospective clinical trial and validation in a population-based registry. Lancet Oncol. 2015;16(9):1111-1122. doi:10.1016/S1470-2045(15)00169-2
- Green MR, Kihira S, Liu CL, et al. Mutations in early follicular lymphoma progenitors are associated with suppressed antigen presentation. Proc Natl Acad Sci U S A. 2015;112(10):E1116-1125. doi:10.1073/pnas.1501199112
- Zhang J, Vlasevska S, Wells VA, et al. The CREBBP acetyltransferase is a haploinsufficient tumor suppressor in B-cell lymphoma. Cancer Discov. 2017;7(3):322-337. doi:10.1158/2159-8290.CD-16-1417
- Ortega-Molina A, Boss IW, Canela A, et al. The histone lysine methyltransferase KMT2D sustains a gene expression program that represses B cell lymphoma development. Nat Med. 2015;21(10):1199-1208. doi:10.1038/nm.3943
- Tazverik. Prescribing information. Epizyme; 2020. Accessed August 24, 2021. https://bit.ly/3fGgbQv
- Brice P, Bastion Y, Lepage E, et al. Comparison in low-tumor-burden follicular lymphomas between an initial no-treatment policy, prednimustine, or interferon alfa: a randomized study from the Groupe d'Etude des Lymphomes Folliculaires. Groupe d'Etude des Lymphomes de l'Adulte. J Clin Oncol. 1997;15(3):1110-1117. doi:10.1200/JCO.1997.15.3.1110
- NCCN Clinical Practice Guidelines in Oncology: B-Cell Lymphomas. Version 5.2021. Accessed January 20, 2022. https://www.nccn.org/professionals/physician_gls/pdf/b-cell.pdf
- Solal-Celigny P. Follicular Lymphoma International Prognostic Index. Curr Treat Options Oncol. 2006;7(4):270-275. doi: 10.1007/s11864-006-0036-3
- Federico M, Bellei M, Marcheselli L, et al. Follicular lymphoma international prognostic index 2: a new prognostic index for follicular lymphoma developed by the international follicular lymphoma prognostic factor project. J Clin Oncol. 2009;27(27):4555-4562. doi:10.1200/JCO.2008.21.3991
- Mozas P, Rivero A, Lopez-Guillermo A. Past, present and future of prognostic scores in follicular lymphoma. Blood Rev. 2021;50:100865. doi:10.1016/j.blre.2021.100865
- Mir F, Barrington SF, Brown H, et al. Baseline SUVmax did not predict histological transformation in follicular lymphoma in the phase 3 GALLIUM study. Blood. 2020;135(15):1214-1218. doi:10.1182/blood.2019001091
- Le Dortz L, De Guibert S, Bayat S, et al. Diagnostic and prognostic impact of 18F-FDG PET/CT in follicular lymphoma. Eur J Nucl Med Mol Imaging. 2010;37(12):2307-2314. doi:10.1007/s00259-010-1539-5
- Luminari S, Biasoli I, Arcaini L, et al. The use of FDG-PET in the initial staging of 142 patients with follicular lymphoma: a retrospective study from the FOLL05 randomized trial of the Fondazione Italiana Linfomi. Ann Oncol. 2013;24(8):2108-2112. doi:10.1093/annonc/mdt137
- Michallet AS, Lebras LL, Bauwens DD, et al. Early stage follicular lymphoma: what is the clinical impact of the first-line treatment strategy? J Hematol Oncol. 2013;6:45. doi:10.1186/1756-8722-6-45
- Nooka AK, Nabhan C, Zhou X, et al. Examination of the follicular lymphoma international prognostic index (FLIPI) in the National LymphoCare study (NLCS): a prospective US patient cohort treated predominantly in community practices. Ann Oncol. 2013;24(2):441-448. doi:10.1093/annonc/mds429
- Kahl BS, Hong F, Williams ME, et al. Rituximab extended schedule or re-treatment trial for low-tumor burden follicular lymphoma: eastern cooperative oncology group protocol e4402. J Clin Oncol. 2014;32(28):3096-3102. doi:10.1200/JCO.2014.56.5853
- Rummel MJ, Niederle N, Maschmeyer G, et al. Bendamustine plus rituximab versus CHOP plus rituximab as first-line treatment for patients with indolent and mantle-cell lymphomas: an open-label, multicentre, randomised, phase 3 non-inferiority trial. Lancet. 2013;381(9873):1203-1210. doi:10.1016/S0140-6736(12)61763-2
- Flinn IW, van der Jagt R, Kahl BS, et al. Randomized trial of bendamustine-rituximab or R-CHOP/R-CVP in first-line treatment of indolent NHL or MCL: the BRIGHT study. Blood. 2014;123(19):2944-2952. doi:10.1182/blood-2013-11-531327
- Salles G, Seymour JF, Offner F, et al. Rituximab maintenance for 2 years in patients with high tumour burden follicular lymphoma responding to rituximab plus chemotherapy (PRIMA): a phase 3, randomised controlled trial. Lancet. 2011;377(9759):42-51. doi:10.1016/S0140-6736(10)62175-7
- Marcus R, Davies A, Ando K, et al. Obinutuzumab for the first-line treatment of follicular lymphoma. N Engl J Med. 2017;377(14):1331-1344. doi:10.1056/NEJMoa1614598
- Hiddemann W, Barbui AM, Canales MA, et al. Immunochemotherapy with obinutuzumab or rituximab for previously untreated follicular lymphoma in the GALLIUM study: influence of chemotherapy on efficacy and safety. J Clin Oncol. 2018;36(23):2395-2404. doi:10.1200/JCO.2017.76.8960
- Messmer M, Wagner-Johnston N. COVID-19 vaccination in patients on rituximab: a survey of lymphoma physicians at NCI designated cancer centers. Leuk Lymphoma. 2021;62(12):3019-3022. doi:10.1080/10428194.2021.1941939
- Morschhauser F, Fowler NH, Feugier P, et al. Rituximab plus lenalidomide in advanced untreated follicular lymphoma. N Engl J Med. 2018;379(10):934-947. doi:10.1056/NEJMoa1805104.
- Rummel M, Kaiser U, Balser C, et al. Bendamustine plus rituximab versus fludarabine plus rituximab for patients with relapsed indolent and mantle-cell lymphomas: a multicentre, randomised, open-label, non-inferiority phase 3 trial. Lancet Oncol. 2016;17(1):57-66. doi:10.1016/S1470-2045(15)00447-7
- Tobinai K, Igarashi T, Itoh K, et al. Rituximab monotherapy with eight weekly infusions for relapsed or refractory patients with indolent B cell non-Hodgkin lymphoma mostly pretreated with rituximab: a multicenter phase II study. Cancer Sci. 2011;102(9):1698-1705. doi:10.1111/j.1349-7006.2011.02001.x
- Leonard JP, Trneny M, Izutsu K, et al. AUGMENT: A phase III study of lenalidomide plus rituximab versus placebo plus rituximab in relapsed or refractory indolent lymphoma. J Clin Oncol. 2019;37(14):1188-1199. doi:10.1200/JCO.19.00010
- Sehn LH, Chua N, Mayer J, et al. Obinutuzumab plus bendamustine versus bendamustine monotherapy in patients with rituximab-refractory indolent non-Hodgkin lymphoma (GADOLIN): a randomised, controlled, open-label, multicentre, phase 3 trial. Lancet Oncol. 2016;17(8):1081-1093. doi:10.1016/S1470-2045(16)30097-3
- Radford J, Davies A, Cartron G, et al. Obinutuzumab (GA101) plus CHOP or FC in relapsed/refractory follicular lymphoma: results of the GAUDI study (BO21000). Blood. 2013;122(7):1137-1143. doi:10.1182/blood-2013-01-481341
- Jurinovic V, Metzner B, Pfreundschuh M, et al. Autologous stem cell transplantation for patients with early progression of follicular lymphoma: a follow-up study of 2 randomized trials from the German Low Grade Lymphoma Study Group. Biol Blood Marrow Transplant. 2018;24(6):1172-1179. doi:10.1016/j.bbmt.2018.03.022
- Casulo C, Friedberg JW, Ahn KW, et al. Autologous transplantation in follicular lymphoma with early therapy failure: A National LymphoCare Study and Center for International Blood and Marrow Transplant research analysis. Biol Blood Marrow Transplant. 2018;24(6):1163-1171. doi:10.1016/j.bbmt.2017.12.771
- Gribben JG, Fowler N, Morschhauser F. Mechanisms of action of lenalidomide in B-cell non-hodgkin lymphoma. J Clin Oncol. 2015;33(25):2803-2811. doi:10.1200/JCO.2014.59.5363
- Burger JA, Wiestner A. Targeting B cell receptor signalling in cancer: preclinical and clinical advances. Nat Rev Cancer. 2018;18(3):148-167. doi: 10.1038/nrc.2017.121
- Gopal AK, Kahl BS, de Vos S, et al. PI3Kδinhibition by idelalisib in patients with relapsed indolent lymphoma. N Engl J Med. 2014;370(11):1008-1018. doi:10.1056/NEJMoa1314583
- Dreyling M, Santoro A, Mollica L, et al. Phosphatidylinositol 3-kinase inhibition by copanlisib in relapsed or refractory indolent lymphoma. J Clin Oncol. 2017;35(35):3898-3905. doi:10.1200/JCO.2017.75.4648
- Flinn IW, Miller CB, Ardeshna KM, et al. DYNAMO: a phase II study of duvelisib (IPI-145) in patients with refractory indolent non-Hodgkin lymphoma. J Clin Oncol. 2019;37(11):912-922. doi:10.1200/JCO.18.00915
- Fowler NH, Samaniego F, Jurczak W, et al. Umbralisib, a dual PI3Kdelta/CK1epsilon inhibitor in patients with relapsed or refractory indolent lymphoma. J Clin Oncol. 2021;39(15):1609-1618. doi:10.1200/JCO.20.03433
- Huet S, Xerri L, Tesson B, et al. EZH2 alterations in follicular lymphoma: biological and clinical correlations. Blood Cancer J. 2017;7(4):e555. doi:10.1038/bcj.2017.32
- Morschhauser F, Tilly H, Chaidos A, et al. Tazemetostat for patients with relapsed or refractory follicular lymphoma: an open-label, single-arm, multicentre, phase 2 trial. Lancet Oncol. 2020;21(11):1433-1442. doi:10.1016/S1470-2045(20)30441-1
- Zevalin (90Y-ibritumomab tiuxetan). Prescribing information. Accessed February 25, 2022. https://bit.ly/3hUVDEK
- Bexxar (131I- tositumomab) Prescribing information. Accessed February 25, 2022. https://bit.ly/3ME0Wqs
- Federal Register. FDA Bexxar withdrawal notification. October 23, 2013. Accessed February 25, 2022. https://bit.ly/3MxYMbM
- Gordon LI, Witzig TE, Molina A, et al. Yttrium 90-labeled ibritumomab tiuxetan radioimmunotherapy produces high response rates and durable remissions in patients with previously treated B-cell lymphoma. Clin Lymphoma. 2004;5(2):98-101. doi: 10.3816/clm.2004.n.015
- Witzig TE, Flinn IW, Gordon LI, et al. Treatment with ibritumomab tiuxetan radioimmunotherapy in patients with rituximab refractory follicular Non-Hodgkin’s lymphoma. J Clin Oncol. 2002;20(15):3262-3269. doi: 10.1200/JCO.2002.11.017
- Kolstad A, Illidge T, Bolstad N, et al. Phase 1/2a study of 177Lu-lilotomab satetraxetan in relapsed/refractory indolent non-Hodgkin lymphoma. Blood Adv. 2020;4(17):4091-4101. doi: 10.1182/bloodadvances.2020002583
- Jacobson C, Chavez JC, Sehgal AR, et al. Primary analysis of ZUMA-5: a phase 2 study of axicabtagene ciloleucel (axi-cel) in patients with relapsed/refractory (R/R) indolent non-Hodgkin lymphoma (iNHL). Blood. 2020;136(suppl 1):40-41. doi:10.1182/blood-2020-136834
- Neelapu SS, Chavez JC, Sehgal AR, et al. Long-term follow-up analysis of ZUMA-5: a phase 2 study of axicabtagene ciloleucel (axi-cel) in patients with relapsed/refractory (R/R) indolent non-Hodgkin lymphoma (iNHL). Blood. 2021;138(suppl 1):93-93. doi:10.1182/blood-2021-148473
- Fowler NH, Dickinson M, Dreyling M, et al. Tisagenlecleucel in adult relapsed or refractory follicular lymphoma: the phase 2 ELARA trial. Nat Med. Published online December 17, 2021. doi:10.1038/s41591-021-01622-0
- Morschhauser F, Flinn IW, Advani R, et al. Polatuzumab vedotin or pinatuzumab vedotin plus rituximab in patients with relapsed or refractory non-Hodgkin lymphoma: final results from a phase 2 randomised study (ROMULUS). Lancet Haematol. 2019;6(5):e254-e265. doi:10.1016/S2352-3026(19)30026-2
- Sehn LH, Kamdar M, Herrera AF, et al. Randomized phase 2 trial of polatuzumab vedotin (pola) with bendamustine and rituximab (BR) in relapsed/refractory (r/r) FL and DLBCL. J Clin Oncol. 2018;36(suppl 15):7507. doi:10.1200/JCO.2018.36.15_suppl.7507
- Diefenbach C, Kahl BS, Banerjee L, et al. Polatuzumab vedotin plus obinutuzumab and lenalidomide in patients with relapsed/refractory follicular lymphoma: primary analysis of the full efficacy population in a phase Ib/II trial. Blood. 2019;134(suppl 1):126. doi:10.1182/blood-2019-123669
- Bannerji R, Yuen S, Phillips TJ, et al. Polatuzumab vedotin + obinutuzumab + venetoclax in patients with relapsed/refractory (R/R) follicular lymphoma (FL): Primary analysis of a phase 1b/2 trial. J Clin Oncol. 2021;39(suppl 15):7534. doi:10.1200/JCO.2021.39.15_suppl.7534
- Hamadani M, Radford J, Carlo-Stella C, et al. Final results of a phase 1 study of loncastuximab tesirine in relapsed/refractory B-cell non-Hodgkin lymphoma. Blood. 2021;137(19):2634-2645. doi:10.1182/blood.2020007512
- Morschhauser F, Ghosh N, Lossos IS, et al. Obinutuzumab-atezolizumab-lenalidomide for the treatment of patients with relapsed/refractory follicular lymphoma: final analysis of a Phase Ib/II trial. Blood Cancer J. 2021;11(8):147. doi:10.1038/s41408-021-00539-8
- Nastoupil LJ, Westin JR, Fowler NH, et al. Response rates with pembrolizumab in combination with rituximab in patients with relapsed follicular lymphoma: Interim results of an on open-label, phase II study. J Clin Oncol. 2017;35(suppl 15):7519. doi:10.1200/JCO.2017.35.15_suppl.7519
- Hawkes EA, Lee ST, Chong G, et al. Immune priming with nivolumab followed by nivolumab and rituximab in first-line treatment of follicular lymphoma: The phase 2 1st FLOR study. J Clin Oncol. 2021;39(suppl 15):7560. doi:10.1200/JCO.2021.39.15_suppl.7560
- Advani R, Flinn I, Popplewell L, et al. CD47 Blockade by Hu5F9-G4 and rituximab in non-Hodgkin's lymphoma. N Engl J Med. 2018;379(18):1711-1721. doi:10.1056/NEJMoa1807315
- Jurczak W, Zinzani PL, Gaidano G, et al. Phase IIa study of the CD19 antibody MOR208 in patients with relapsed or refractory B-cell non-Hodgkin's lymphoma. Ann Oncol. 2018;29(5):1266-1272. doi:10.1093/annonc/mdy056
- Budde LE, Sehn LH, Matasar MJ, et al. Mosunetuzumab monotherapy is an effective and well-tolerated treatment option for patients with relapsed/refractory (R/R) follicular lymphoma (FL) who have received ≥2 prior lines of therapy: pivotal results from a phase I/II study. Blood. 2021;138(suppl 1):127. doi:10.1182/blood-2021-145872
- Morschhauser F, Bishton M, Eyre TA, et al. Mosunetuzumab in combination with lenalidomide has a manageable safety profile and encouraging activity in patients with relapsed/refractory follicular lymphoma: initial results from a phase Ib study. Blood. 2021;138(suppl 1):129. doi:10.1182/blood-2021-145694
- Morschhauser F, Carlo-Stella C, Dickinson M, et al. Glofitamab as monotherapy and in combination with obinutuzumab induces high complete response rates in patients (pts) with multiple relapsed or refractory (R/R) follicular lymphoma (FL). Blood. 2021;138(suppl 1):128. doi:10.1182/blood-2021-148778
- Hutchings M, Mous R, Clausen MR, et al. Dose escalation of subcutaneous epcoritamab in patients with relapsed or refractory B-cell non-Hodgkin lymphoma: an open-label, phase 1/2 study. Lancet. 2021;398(10306):1157-1169. doi:10.1016/S0140-6736(21)00889-8
- Bannerji R, Allan JN, Arnason JE, et al. Odronextamab (REGN1979), a Human CD20 x CD3 bispecific antibody, induces durable, complete responses in patients with highly refractory B-cell non-Hodgkin lymphoma, including patients refractory to CAR T therapy. Blood. 2020;136(suppl 1):42-43. doi:10.1182/blood-2020-136659
- Davids MS, Roberts AW, Seymour JF, et al. Phase I first-in-human study of venetoclax in patients with relapsed or refractory non-hodgkin lymphoma. J Clin Oncol. 2017;35(8):826-833. doi:10.1200/JCO.2016.70.4320
- Ujjani CS, Lai C, Leslie LA, et al. Ibrutinib and venetoclax in relapsed and refractory follicular lymphoma. Blood. 2020;136(suppl 1):46-47. doi:10.1182/blood-2020-136219
- Portell CA, Jegede O, Wagner-Johnston ND, et al. Phase II study of venetoclax in combination with obinutuzumab and bendamustine in patients with high tumor burden follicular lymphoma as front line therapy (PrECOG 0403). Blood. 2021;138(suppl 1):814. doi:10.1182/blood-2021-145217

Highlighting Insights From the Marginal Zone Lymphoma Workshop
Clinicians outline the significance of the MZL Workshop, where a gathering of international experts in the field discussed updates in the disease state.