Optimal Post-Treatment Surveillance in Cancer Survivors: Is More Really Better?
In this review, we discuss the established guidelines and current evidence regarding post-treatment surveillance, and we propose general management strategies in prostate, colorectal, and breast cancers.
Table 1: Published Prostate Cancer Surveillance Guidelines
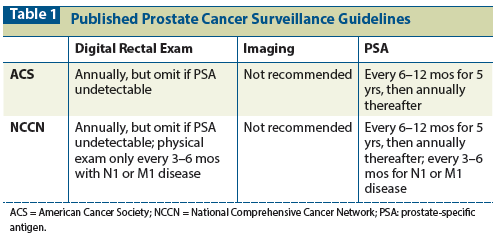
Table 2: Prostate Cancer Post-Treatment Surveillance: Common Practices, Data, and Author Recommendations Studies For or Against Use Author Recommendations
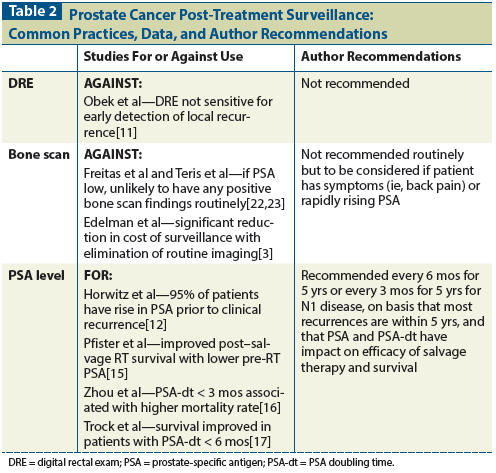
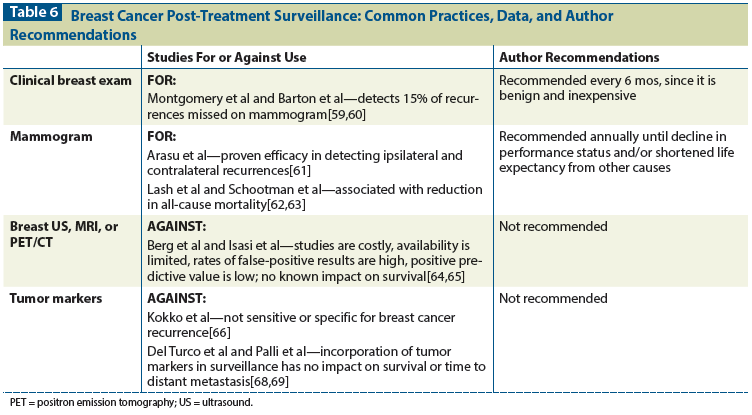
Table 3: Published Colorectal Cancer Surveillance Guidelines
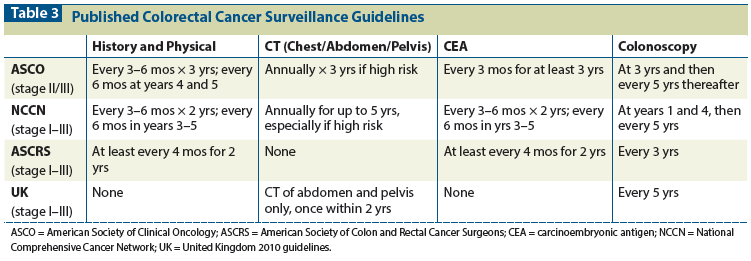
Table 4: Colorectal Cancer Post-Treatment Surveillance: Common Practices, Data, and Author Recommendations
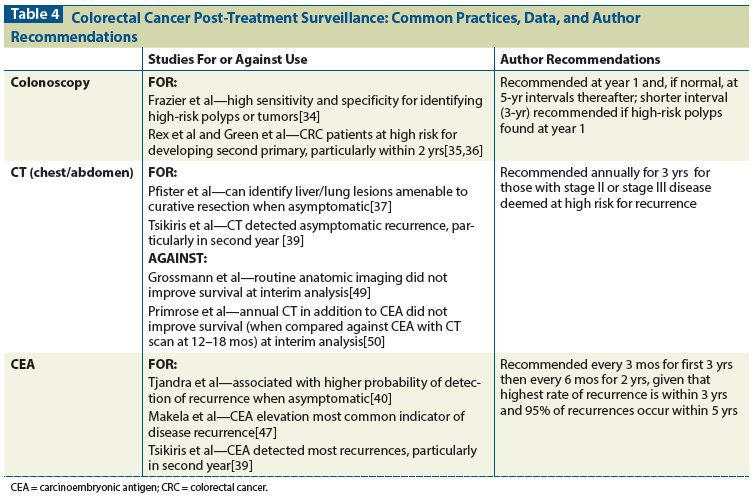
Table 5: Published Breast Cancer Surveillance Guidelines
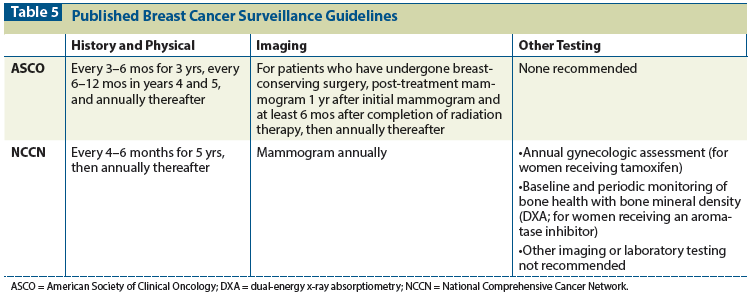
Table 6: Breast Cancer Post-Treatment Surveillance: Common Practices, Data, and Author Recommendations

A substantial rise in the number of cancer survivors has led to management questions regarding effective post-treatment surveillance strategies. Although a number of professional societies have proposed surveillance guidelines, clinical practice varies; the general trend is toward more intensive strategies. The evidence supporting intensive surveillance is relatively lacking, with most studies showing that more intense surveillance regimens have minimal, if any, impact on outcomes in terms of survival, quality of life, or overall cost-effectiveness. This has been demonstrated in breast cancer, and data supporting a similar conclusion may be evolving in colorectal cancer, where large prospective studies call into question the utility of intensive surveillance; in prostate cancer, retrospective data suggest a similar trend. In this review, we discuss the established guidelines and current evidence regarding post-treatment surveillance, and we propose general management strategies in prostate, colorectal, and breast cancers.
Introduction
Improvements in the diagnosis and treatment of several cancers have resulted in a substantial population of cancer survivors. There are at least 14 million cancer survivors in the United States alone, with estimates projected to increase to at least 18 million as the general population ages and post-treatment survival rates continue to improve.[1,2] The growth of this population raises a new management question: that of optimal post-treatment surveillance. While there are guidelines that serve to direct this type of care, the data are not always clear and clinical practice often varies.
In common clinical practice, suspicion for cancer recurrence is often signaled by the development of symptoms or changes in physical examination findings, with supplemental testing used for confirmation. While this strategy is largely effective, patients in whom it is employed may have asymptomatic potentially treatable disease, and thus run the risk of presenting late in the disease course and ultimately not being candidates even for palliative therapy. While treatment after recurrence is unlikely to result in cure in the majority of cancers, efficacious therapies do exist that can provide palliation of symptoms and, in many cases, prolong life.[3]
The proposed benefits and risks of routine post-treatment surveillance must be weighed carefully for each patient and are likely to vary between cancer types. Arguments for routine surveillance include the detection of recurrent cancers when patients potentially are minimally or completely asymptomatic and may have better options for management, some of which could be curative. With this advantage, however, come concerns regarding cost-effectiveness in the current era of stricter insurance regulations, risks related to additional radiation exposure, and the possibility of additional tests or invasive procedures being conducted after potentially false-positive results.[4,5] The psychosocial effects of routine surveillance are also less clear; while patients and providers alike may be reassured by the persistence of a “disease-free” status, testing itself can cause a significant amount of anxiety and stress.
Edelman et al have proposed general principles that could potentially be used to guide the most appropriate selection of surveillance tests:
1) The interval between examinations and the duration of testing should align with the time of maximal recurrence risk and natural tumor history.
2) Studies should be directed to the most likely sites of recurrence and should have a high predictive value.
3) Therapies for recurrence that may cure, prolong life, or provide appropriate palliation should be available.
4) The potential increased risk of secondary malignancy based on shared etiologic risk should be incorporated into consideration of testing strategies.[3]
Here we present an overview of the data on surveillance after definitive treatment (ie, treatment with curative intent) in three of the most common malignancies: prostate cancer, colorectal cancer, and breast cancer. We highlight what we believe are likely the most effective surveillance strategies in each setting.
Prostate Cancer
Prostate cancer is the second most common cancer in men worldwide. Despite being the second highest cause of cancer-related death (after lung cancer), there are almost 3 million survivors in the United States, comprising nearly 45% of the country’s total male cancer survivor population. It is estimated that this number will exceed 4 million survivors by 2024. Indeed, largely because of older age at diagnosis, earlier detection, effective treatment strategies, and protracted clinical courses, most men in whom prostate cancer is diagnosed have a higher risk of death from noncancer causes than from prostate cancer.[6,7]
Management of early-stage prostate cancer can vary from observation to androgen deprivation to radiation or surgery. When treated definitively (ie, with radiation or prostatectomy), the highest risk of recurrence is within the 5 years following treatment, although patients can be at risk for recurrence for up to and even more than 10 years.[8] Post-treatment surveillance in prostate cancer may include clinical visits, with a combination of physical examination, prostate-specific antigen (PSA) testing, and imaging, as appropriate. Current National Comprehensive Cancer Network (NCCN) guidelines recommend checking PSA level every 6 to 12 months for 5 years, then annually as indicated based on age, comorbidities, and anticipated life expectancy. A digital rectal examination (DRE) can be performed annually but may be omitted if the PSA level is undetectable. In patients with N1 or M1 disease, a physical examination should be performed and a PSA level obtained every 3 to 6 months. [9] The American Cancer Society (ACS) has similar guidelines, although these are mainly geared toward primary care providers (Table 1).[10]
While routine physician visits may serve to decrease anxiety and reassure the patient, most prostate cancer recurrences initially are asymptomatic. The role of the DRE in serial physical examinations is unclear. After radical prostatectomy, the prostatic fossa should be empty. Despite this, DRE is not sensitive for the early detection of local recurrence. In a retrospective study of 501 men, only 4 of the 501 had an abnormal DRE, although 72 of the 501 were suspected to have disease recurrence based on a rise in the PSA level.[11] This suggests that inclusion of the DRE, which is inexpensive and largely low-risk, is not necessarily imperative in the post-treatment surveillance setting.
The PSA level is the gold standard for the detection of recurrence. While use of the PSA level in screening is controversial, its utility in post-treatment surveillance is clearer, with as many as 95% of men showing a rise in PSA level prior to clinical recurrence.[12] The definition of PSA recurrence, or biochemical failure, depends on the initial treatment. There are two sets of classically accepted guidelines defining biochemical failure; one comes from the American Society for Radiation Oncology, and the other is the Phoenix criteria.[13] In patients who undergo radical prostatectomy, the PSA level is expected to approach almost zero 4 to 6 weeks after surgery, based on a normal half-life of 48–72 hours. Although the American Urological Association defines biochemical failure as a PSA of > 0.2 ng/mL on two or more measurements, many clinicians consider any consistent value of > 0.1 ng/mL (the typical limit of detection using standard immunoassays) to be indicative of recurrence.[14] The definition of biochemical failure post-radiotherapy (RT) is more challenging, since the PSA nadir, characterized as the lowest post-treatment PSA level, varies considerably. Transient post-RT increases in PSA not associated with recurrence, known as “the PSA bounce,” further complicates this. Overall, PSA instability, rather than absolute values, is more concerning for recurrent disease.
While early detection of prostate cancer recurrence using PSA levels is possible, the utility of this measure depends on whether interventions performed based on the values obtained will have an impact on outcomes. Prospective data pertinent to this question are absent, but retrospective data do potentially support a role for the salvage therapies that are often initiated on the basis of PSA level (along with subsequent imaging, biopsy, etc). Initiation of salvage RT after radical prostatectomy appears to be more effective when the serum PSA level is < 0.5 ng/mL. In addition, one study suggests that better post–salvage RT survival is associated with lower pre-RT PSA levels, implying that earlier intervention may be more efficacious.[15]
Also of significance is the role of the PSA doubling time (PSA-dt). A large retrospective study of more than 1,000 men after radical prostatectomy or post-radiation showed that a PSA-dt of less than 3 months was significantly associated with a high risk for prostate cancer–specific mortality at 5 years.[16] A study from Johns Hopkins, comprised of 635 patients, similarly showed improvement in cancer-related survival with salvage RT (compared with observation) in patients with a short PSA-dt (< 6 months).[17] Together, these studies imply that close monitoring of the PSA level and the PSA-dt can effectively identify patients with more aggressive disease who may benefit from early salvage intervention.
Improvements in relapse rates and overall survival with salvage therapy after biochemical recurrence have also been shown in other retrospective studies. Post–salvage RT relapse was significantly decreased in a series of approximately 3,000 men, and a similar study showed an improvement in all-cause mortality, regardless of PSA-dt.[18,19] The efficacy of salvage radical prostatectomy after initial RT has been shown in a study involving 400 patients, with cancer-related survival reaching 95% at 10 years. [20] The optimal frequency for checking PSA levels, however, is debatable. A recent study looking at the association between the number of PSA tests during follow-up and outcomes showed no improvement in survival with an increased number of tests.[21] Overall, while the data are limited by their retrospective nature and the lack of consistent comparisons against observation alone, there appears to be a role for salvage therapies after biochemical recurrence, with a trend towards improvement in outcomes.
The use of imaging studies such as MRI and bone scanning in routine post-treatment prostate cancer surveillance should be limited to patients who are symptomatic, have physical examination findings, or have a rapidly rising PSA level that would suggest a later, more systemic recurrence. Studies have shown that the PSA level can be correlated with bone scan findings and that lower PSA values excluded the possibility of positive scans, with negative predictive values reaching almost 99%.[22,23] From a cost perspective, eliminating routine imaging studies as part of post-treatment surveillance significantly reduces cost, with estimates per 1,000 patients for a 10-year period ranging from $339 million for intensive radiographic surveillance down to $1.4 million for symptom-directed surveillance.[3]
Of note, while routine clinician visits likely have a limited role in early detection of recurrence, these visits may have a role in reducing anxiety and also are useful in the management of treatment-related complications such as impotence and incontinence, all significant in the assessment of quality-of-life outcomes. The development of cancer survivorship programs can assist in addressing these needs and identifying provider roles in their management. The Michigan Cancer Consortium and the ACS both recently published guidelines to assist primary care physicians in the management of long-term prostate cancer survivors and that can also be used synergistically to improve outcomes of specialist care.[10,24]
While active surveillance, treatment with androgen-deprivation only, and metastatic disease are not addressed here, principles similar to those used in post-treatment surveillance could be applied in these settings as well, with the PSA level playing a key role in identification of progression of disease.
In sum, while there is an obvious need for more standardized, evidence-based surveillance practices in prostate cancer, a reasonable approach to post-treatment surveillance after initial definitive therapy would include a clinician visit, physical examination, and measurement of PSA level every 6 months (with imaging and DRE used only in patients with rapid PSA rises or symptoms). In patients with N1 disease, measurement of PSA level every 3 months would be appropriate. Given that most recurrences occur within 5 years of the completion of treatment, this duration would be reasonable. After 5 years, the decision of whether to continue annual PSA testing should be based on patient age, comorbidities, and life expectancy (Table 2).
Colorectal Cancer
Approximately 150,000 new cases of colorectal cancer are diagnosed in the United States each year, with global estimates reaching 1 million.[25] In the United States alone, there are currently approximately 1.2 million colorectal cancer survivors. [26] Surgical resection is the primary treatment for up to 80% of nonmetastatic colorectal cancers, but despite advances in adjuvant management with RT and chemotherapy, colorectal cancer remains the third most common cause of cancer death in the United States. Data from the analysis of 20,898 patients enrolled in 18 large randomized trials of adjuvant therapy for colon cancer demonstrate that 80% of recurrences occur in the first 3 years after surgical resection of the primary tumor, and a more recent study showed that 95% of recurrences occur in the first 5 years after initial curative-intent surgery.[27,28]
The majority of colorectal cancer survivors undergo post-treatment surveillance, the rationale for which is that early detection of recurrent or metachronous disease amenable to other curative therapies improves survival outcomes. Other reasons include detection for potential use of palliative therapies (even prior to symptom onset) and improvement in overall quality of life. Most surveillance guidelines (Table 3) include a combination of: clinician visits with history and physical examination; imaging; colonoscopy; and laboratory tests, including measurement of the carcinoembryonic antigen (CEA). Current NCCN guidelines for stages I-III colorectal cancer recommend a history and physical examination, along with measurement of CEA every 3 to 6 months for 2 years and then every 6 months for years 3 through 5. Imaging, including CT scanning of the chest, abdomen, and pelvis in select high-risk survivors is recommended annually for up to 5 years, and colonoscopy is recommended in years 1 and 4, and then every 5 years thereafter (or more frequently, depending on colonoscopy findings).[29,30] There is modest variation in the guidelines of other national societies, such as those of the American Society of Clinical Oncology (ASCO; which recommend a shorter duration of surveillance overall [3 years for most studies]) and those of the American Society of Colon and Rectal Surgeons (which make no recommendation for routine imaging unless indicated per symptoms). Interestingly, European societies in general tend to subscribe to a much less intense surveillance program than those commonly used in the United States.[31-33]
Each of the surveillance tools recommended in various guidelines does, to some extent, have utility. While a history and physical examination alone are insufficient for detecting disease recurrence, periodic clinician visits are important for the assessment of symptoms that could suggest disease recurrence, for management of side effects related to initial treatment, for promotion of healthy behaviors that may impact colorectal cancer outcomes (such as physical activity and diet), and for maintenance of a patient-provider rapport that may assuage anxiety. Colonoscopy can be useful for the detection of second primary colorectal cancers and anastomotic recurrences of the initial primary tumor at a stage that could be amenable to curative treatment. The procedure has a sensitivity of 95% and a specificity of 100% for detecting high-risk polyps or tumors.[34] The chief purpose of surveillance colonoscopies is the identification and removal of metachronous polyps, since patients with a history of colorectal cancer have an increased risk for the development of second primary colorectal cancers, particularly in the first 2 years after resection.[35,36]
An argument for routine CT scans post-treatment can be made, since liver and lung metastases can be asymptomatic early in their natural history, the time when they may be most amenable to surgical resection, particularly in patients with high-risk stage II or stage III disease.[37] Serum CEA levels, while controversial in cancer screening, correlate well with disease burden and are of prognostic value in established disease.[38] A secondary analysis from the Clinical Outcomes of Surgical Therapy (COST) trial showed that CEA levels detected the most recurrences (followed by CT scans), particularly in the second year after diagnosis.[39] The CEA assay is the only test whose increased use is associated with a higher probability of detection of asymptomatic recurrence, a higher curative reoperation rate, and greater mortality reduction on meta-analysis.[40] Ironically, in studies evaluating guideline adherence, adherence to scheduled CEA testing is among the lowest.[41]
Although post-treatment surveillance has been associated with some, if modest, overall survival benefit, improvement in cancer-specific outcomes has not been demonstrated, and as discussed above, the optimal intensity of surveillance regimens has not been standardized. While there is a substantial subset of randomized controlled trial data in the area of colorectal cancer surveillance, studies are small and span a period of more than 20 years, resulting in heterogeneity in the surveillance regimens studied. Two older studies showed an overall survival benefit for more intensive surveillance strategies, although notably these improvements were in all-cause mortality, and in one of the studies, colonoscopy was considered an intensive surveillance tool, even though it is now routinely incorporated into surveillance strategies.[42,43] A meta-analysis by Renehan et al of these and other earlier randomized controlled trials showed that intensive follow-up was associated with a reduction in all-cause mortality.[44] Two later meta-analyses, by Tjandra et al and Jeffery et al, also detected statistically significant improvements in all-cause mortality for intensive surveillance, with odds ratios of 0.74 and 0.73, respectively. Additionally, they found that while both intensive and less intensive surveillance led to detection of a similar number of recurrences, detection occurred 6 to 7 months earlier with intensive surveillance, and curative reoperation (“salvage surgery”) was more likely in patients who underwent intensive surveillance.[40,45]
Although some early studies showed an improvement in overall survival, several others have not shown this effect.[46-48] A study by Makela et al of patients who had undergone resection for colorectal cancer showed that while recurrences were identified earlier in the intensive surveillance group, earlier detection did not lead to either significant improvements in resectability or improved 5-year survival. Notably, most patients were asymptomatic at the time of recurrence in both groups, with CEA elevation the most common finding heralding recurrence.[47] The meta-analysis by Renehan et al also estimated that only about one-fifth of the survival benefit of intensive surveillance was due to curative treatment of recurrence. Notably, none of the meta-analyses previously discussed found an improvement in cancer-specific mortality with intensive surveillance.[40,44,45] Thus, the increased rates of overall survival, earlier detection of recurrence, and higher re-operation rates seen in some early trials may only be circumstantial and not clear evidence that intensive surveillance prolongs life.
Several more recent, large prospective trials are currently assessing the utility of intensive vs less intensive post-treatment surveillance in colorectal cancer. In an attempt to avoid the heterogeneity of previous studies, these trials are by and large incorporating common surveillance tools and clinical practices. In a trial by the GILDA (Gruppo Italiano di Lavaro per la Diagnosi Anticipata) group of investigators, patients with Dukes B2-C colorectal cancer are being randomly assigned to study arms with varying frequencies of office visits, colonoscopies, imaging (liver ultrasound, chest x-ray, and in the case of rectal cancer survivors, proctoscopy and abdominal-pelvic CT), and CEA measurement. With an overall projected accrual of 1,500 patients across 45 centers, an interim analysis at 14 months showed no improvement in survival in any of the different cohorts.[49] In the Follow-up After Colorectal Surgery (FACS) trial, patients were randomly assigned to minimal follow-up (a single CT at 12–18 months and no further scheduled follow-up), CEA follow-up (CT at 12–18 months and scheduled CEA testing every 3 months for 2 years, then every 6 months for 3 years), CT follow-up (scheduled CT every 6 months for 2 years, then annually for 3 years, for a total of 5 years), or both (scheduled CEA testing and CT scans). The primary outcome was surgical treatment of recurrence with curative intent, with secondary outcomes of mortality and survival after treatment of recurrence for cure. Similar to the GILDA trial, after a mean 3.7 years of follow-up, no differences between the groups in overall or cancer-specific mortality were reported in the recently published interim analysis. Scheduled CEA testing demonstrated a 3% improvement in detected recurrences amenable to surgical therapy, with similar improvements seen in the group undergoing combined surveillance with scheduled CEA testing and CT imaging. It is notable that two-thirds of recurrences in the study participants were detected through scheduled follow-up testing, and that significantly more patients underwent resection with curative intent in the groups undergoing intensive surveillance.[50] A third trial, Assessment of Frequency of Surveillance after Curative Resection in Patients with Stage II and III Colorectal Cancer (COLOFOL), is comparing two surveillance regimens involving imaging and CEA testing at various intervals, with primary mortality outcomes, as well as secondary outcomes of recurrence-free survival, quality of life, and cost. Results of this trial are pending.[51]
Given the variability in guidelines, the natural course of colorectal cancer, and potential patient comorbidities, surveillance decisions in colorectal cancer may need to be tailored to the characteristics of the individual patient. A risk-adapted strategy was evaluated by Secco et al in which patients who had recently undergone curative treatment for colorectal cancer were divided into “high recurrence risk” and “low recurrence risk” groups on the basis of a number of prognostic factors. These groups were then subdivided into a cohort in which a risk-adapted protocol was used vs a cohort that received minimal follow-up. Within each risk group, the patients who were followed with the risk-adapted protocol showed significantly better 5-year overall survival, presumably achieved through the identification of patients who were eligible for curative reoperation. This strategy also reduced the costs of follow-up in patients who remained disease-free, particularly in the low-recurrence-risk group.[52] Additional data on the utility of a risk-adapted colorectal cancer surveillance strategy are minimal, however, and further studies are needed.
Overall, post-treatment surveillance in colorectal cancer is intended for the early detection of recurrence, with the goal of improving long-term outcomes by identifying potentially curative recurrences when a patient is asymptomatic. Indeed, studies show that patients with asymptomatic recurrences are more likely to be eligible for potentially curative resection, with a greater likelihood of completely resected disease at re-exploration, which may lead to better progression-free and overall survival.[53] While the benefit of salvage therapies for metastatic or recurrent disease is not in question, the optimal intensity of the surveillance regimen for identifying those in need of salvage therapy remains unclear, with earlier studies showing no absolute improvement in cancer-related mortality for more intensive surveillance regimens, and interim analyses from more recent randomized trials showing no survival benefit. While we await final results of these important studies-and until more standardized, evidence-based practices are finalized-a less intensive and reasonable approach to colorectal cancer surveillance may be to limit the duration of surveillance to up to 5 years, with clinician visits, physical examination, and CEA testing every 3 to 6 months, and colonoscopy at year 1 and, if normal, at 3- to 5-year intervals thereafter. For those deemed to be at high risk for recurrence based on tumor-specific clinical and pathologic factors, the use of radiographic imaging in addition to CT scans annually for up to 5 years is reasonable. The value of routine radiographic surveillance in patients with low-risk colorectal cancer is likely low, however; thus, use of radiographic surveillance should be tailored to the individual patient (Table 4).
Breast Cancer
There are more than 3 million breast cancer survivors in the United States alone. The introduction of effective screening and adjuvant therapies has significantly improved survival rates; current 5-year survival rates are near 90%.[54] Despite advances in the management of local recurrence, metastatic disease continues to be a concern; the average survival of patients with metastatic breast cancer is just under 2 years.[55] Detection of asymptomatic breast cancer recurrence carries a more favorable prognosis and, together with poor overall outcomes in the metastatic setting, could be an argument for more intensive surveillance post-treatment, in order to enable earlier detection.[56] The data, though, indicate otherwise. Both NCCN and ASCO surveillance guidelines (Table 5) recommend only clinical visits twice a year for 5 years, along with annual mammography, supporting the conclusion that intensive follow-up with additional imaging studies and routine tumor marker tests does not improve overall survival.[57,58]
The utility of scheduled histories and physical examinations can be seen in data on symptom assessment via clinical breast exam (CBE). Although benign and inexpensive, the CBE is limited by the fact that numerous variables affect the overall assessment, including the characteristics and size of the tumor itself, breast density based on age, and provider exam skills. Despite this, CBE is useful in detecting recurrences in up to 15% of patients and potentially can be used as a safeguard against false negatives, as mammography may miss up to 15% of palpable lesions.[59,60]
The mainstay of breast cancer surveillance imaging is mammography, with up to 50% of ipsilateral recurrences and 80% of contralateral recurrences detected on mammograms alone.[61] While evidence is limited, surveillance mammography appears to be associated with a reduction in all-cause mortality. In a case-controlled study that compared mammography use in women over 65 years of age who died or did not die of breast cancer and who lived at least 30 months following breast cancer diagnosis, women who had undergone a surveillance mammogram within 1 year of completion of treatment were less likely to die of breast cancer.[62,63] However, even though mammography itself is efficacious, there are limited data on the optimal surveillance interval and duration. Still, most professional societies recommend annual mammography for as long as there is good performance status and reasonable life expectancy.
There are no randomized controlled trials evaluating the effectiveness of breast MRI, ultrasound, or positron emission tomography (PET)/CT in breast cancer surveillance, and these modalities are not recommended in general surveillance guidelines. A trial with approximately 3,000 patients that evaluated the addition of breast ultrasound or MRI to screening mammography found that while these studies increased the diagnostic yield overall, they also increased the rate of false-positive results and therefore lowered the positive predictive value.[64] This, along with the additional associated costs and limited availability of these modalities, restricts their utility in routine surveillance. There also is no role for PET scanning in post-treatment surveillance. While a meta-analysis of 16 studies showed that PET imaging was consistently more sensitive for the detection of early recurrent disease, its subsequent impact on survival and quality of life has not been addressed.[65]
The use of tumor markers, including cancer antigen (CA) 27.29, CA 15-3, and CEA, is not recommended in routine post-treatment surveillance. These markers are neither sensitive nor specific for breast cancer recurrence.[66] The use of tumor markers was included in two separate prospective studies looking at intensive surveillance (which included bone scans, liver ultrasound, and chest x-ray, along with tumor marker testing plus physician visits and annual mammography) vs minimal surveillance (physician visits and annual mammography only). In one study, guidelines for treatment of the initial breast cancer, as well as recurrence, were the same in both arms, and adherence was high. Health-related quality of life was evaluated by validated surveys. With a median follow-up of 71 months, there was no difference in overall survival or time to distant metastasis between the intensive surveillance and minimal surveillance groups. The average time to detection of recurrence was approximately 53 months, and the patterns of recurrence were the same in both arms. In addition, although the majority of women indicated that they would want diagnostic testing in the absence of symptoms, there was no difference in health-related quality of life between the two groups. In fact, intensive surveillance did not improve emotional function or satisfaction with care scores compared with the control arm. The second study, similarly designed, also showed no survival benefit for intensive surveillance compared with minimal surveillance at 5 and 10 years of follow-up.[67-69] A retrospective study reflecting the US population also showed no advantage for intensive surveillance with regard to time to detection of recurrence or survival.[70]
Interestingly, despite established, largely concordant guidelines (of those issued by professional societies), and despite the above-mentioned randomized controlled trials refuting the survival benefit of routine intensive surveillance methods, oncologists continue to engage in intensive surveillance approaches. Surveillance, Epidemiology and End Results (SEER) data from 44,511 women over the age of 65 who were diagnosed with early-stage breast cancer between 1992 and1999 and who were followed until 2001 demonstrate continued use by medical oncologists of surveillance bone scans (19%), tumor antigen testing (47%), chest x-rays (65%), and CT scans (15%) in the first year of follow-up. Although the rates for nonrecommended testing declined over time, maintaining follow-up with an oncologist was associated with higher rates of receipt of these tests.[71] A study by Ramsey et al using SEER records of patients diagnosed with early-stage breast cancer between 2001 and 2007 showed that 42% of patients (out of approximately 40,000 eligible patients) received at least one tumor marker assessment within 2 years of diagnosis, with an associated increase in overall medical costs of 29%.[72]
A population-based study of approximately 10,000 patients in Ontario, Canada, showed a substantial variation in adherence to guideline recommendations. In particular, the investigators noted that a substantial portion of patients received more than the recommended imaging for detection of metastatic disease-but also that a substantial portion of patients received fewer than the recommended number of surveillance mammograms for detection of disease recurrence or a new primary.[73] A more recent survey of ASCO members whose clinical focus was reported as breast cancer suggested that surveillance practices vary markedly by practitioner. Respondents were given 4 surveillance scenarios and a list of 12 modalities for surveillance for use over a 5-year time period. Although the response rate was only 31%, most providers recommended mammography. However, 80% used laboratory studies at least annually for surveillance, and up to 15% recommended radiographic imaging despite guidelines suggesting that it does not improve outcomes.[74]
In sum, advances in screening and adjuvant therapies have improved breast cancer outcomes overall. While outcomes with recurrent disease are best when patients are asymptomatic at the time of recurrence detection, there are no current data to suggest that intensive surveillance strategies using various imaging modalities and tumor marker tests improve those outcomes. Thus, adherence to the guidelines that recommend routine clinician visits with physical and clinical breast exam and annual mammography would reflect the optimal strategy in post-treatment breast cancer surveillance (Table 6).
Conclusion
In this article, we have presented a comprehensive review of the currently available post-treatment surveillance data for three of the most common malignancies and have offered recommendations that also take into account guidelines from professional societies. While the value of aggressive surveillance strategies in any of these cancer types is questionable, they often continue in clinical practice. The Choosing Wisely campaign, an initiative of the American Board of Internal Medicine, not only endorses evidence-based practices but also promotes patient-provider discussions about healthcare options in an effort to decrease costs, improve outcomes, and prevent unnecessary testing. ASCO actively participates in this program, with the goal of reducing cancer care costs.[75] This program, along with the development of interdisciplinary survivorship plans, which often play to the strengths of both primary care providers and specialists, may be key in managing post-treatment surveillance. As the survivor population continues to grow, however, it is clear that more prospective, evidence-based data are needed that can not only ascertain the impact of different medical interventions on outcomes, but that will also take into account cost-effectiveness, exposure risks, psychosocial stressors, and overall quality-of-life issues.
Financial Disclosure:The authors have no significant financial interest in or other relationship with the manufacturer of any product or provider of any service mentioned in this article. Both Dr. Shah and Dr. Denlinger are supported by Fox Chase Cancer Center P30 CA006927.
References:
1. Hartigan-Blanche D, Forsythe LP, Alfano CM, et al. Provision and discussion of survivorship care plans among cancer survivors: results of a nationally representative survey of oncologists and primary care physicians. J Clin Oncol. 2014;32:1578-85.
2. de Moor JS, Mariotto AB, Parry C, et al. Cancer survivors in the United States: prevalence across the survivorship trajectory and implications for care. Cancer Epidemiol Biomark Prevent. 2013;23:561-7.
3. Edelman MJ, Meyers FJ, Siegel D. The utility of follow-up testing after curative cancer therapy: a critical review and economic analysis. J Gen Int Med. 1997;12:318-31.
4. Virgo KS, Lerro CC, Klabunde CN, et al. Barriers to breast and colorectal cancer survivorship care. Perceptions of US primary care physicians and medical oncologists. J Clin Oncol. 2013;31:2322-36.
5. Sodickson A, Baeyens PF, Andriole KP, et al. Recurrent CT, cumulative radiation exposure, and associated radiation-induced cancer risks from CT of adults. Radiology. 2009;251:175-84.
6. Ketchandji M, Kuo YF, Shahinian VB, et al. Cause of death in older men after the diagnosis of prostate cancer. J Am Geriatr Soc. 2009;57:24-30.
7. DeSantis CE, Lin CC, Mariotto AB, et al. Cancer treatment and survivorship statistics, 2014. CA Cancer J Clin. 2014;64:252-71.
8. Hanks GE, Hanlon A, Schultheiss T, et al. Early prostate cancer: the national results of radiation treatment from the patterns of care and radiation therapy oncology group studies with prospects for improvement with conformal radiation and adjuvant androgen deprivation. J Urol. 1994;152:1775-80.
9. National Comprehensive Cancer Network (NCCN). Clinical practice guidelines in oncology: prostate cancer. Version 1.2015. Available from: http://www.nccn.org./professionals/physician_gls/pdf/prostate.pdf. Accessed March 11, 2015.
10. Skolarus TA, Wolf A, Erb NL, et al. American Cancer Society prostate cancer survivorship care guidelines. CA Cancer J Clin. 2014;64:225-49.
11. Obek C, Neulander E, Sadek S, et al. Is there a role for digital rectal examination in the follow-up of patients after radical prostatectomy? J Urol. 1999;162(3 Pt 1):762-64.
12. Horwitz EM, Thames HD, Kuban DA, et al. Definitions of biochemical failure that best predict clinical failure in patients with prostate cancer treated with external beam radiation alone: a multi-institutional pooled analysis. J Urol. 2005;173:797-802.
13. Wallace TJ, Torre T, Grob M, et al. Current approaches, challenges, and future directions for monitoring treatment response in prostate cancer. J Cancer. 2014;5:3-24.
14. Carroll P, Albertsen PC, Greene K, et al. PSA testing for the pretreatment staging and posttreatment management of prostate cancer: 2013 revision of 2009 best practice statement. Available from: https://www.auanet.org/common/pdf/education/clinical-
guidance/Prostate-Specific-Antigen.pdf. Accessed March 11, 2015.
15. Pfister D, Bolla M, Briganti A, et al. Early salvage radiotherapy following radical prostatectomy. Eur Urol. 2014;65:1034.
16. Zhou P, Chen MH, McLeod D, et al. Predictors of prostate cancer-specific mortality after radical prostatectomy or radiation therapy. J Clin Oncol. 2005;28:6992-8.
17. Trock BJ, Han M, Freedland, et al. Prostate cancer-specific survival following salvage radiotherapy vs observation in men with biochemical recurrence after radical prostatectomy. JAMA. 2008;299:2760-9.
18. Boorjian SA, Karnes RJ, Crispen PL, et al. Radiation therapy after radical prostatectomy: impact on metastasis and survival. J Urol. 2009;182: 2708-14.
19. Cotter SE, Chen MH, Moul JW, et al. Salvage radiation in men after prostate-specific antigen failure and the risk of death. Cancer. 2011;117:3925-32.
20. Chade DC, Shariat SF, Cronin AM, et al. Salvage radical prostatectomy for radiation-recurrent prostate cancer: a multi-institutional collaboration. Eur Urol. 2011;60:205-10.
21. Nabhan M, Kim SP, Shah ND, et al. The relationship of the intensity of posttreatment prostate-specific antigen surveillance and prostate cancer outcome: results from a population-based cohort. Mayo Clin Proc. 2012;87:540-7.
22. Freitas JE, Gilvydas R, Ferry JD, et al. The clinical utility of bone scintigraphy in prostate cancer followup. J Nucl Med. 1991;32:1387-90.
23. Teris MK, Klonecke AS, McDougall IR, et al. Utilization of bone scans in conjunction with prostate specific antigen levels in the surveillance for recurrence of adenocarcinoma after radical prostatectomy. J Nucl Med. 1991;32:1713-7.
24. Skolarus TA, Wittmann D, Laurel N, et al. Recommendations for prostate cancer survivorship care: an update to the 2009 Michigan Cancer Consortium guidelines for the primary care management of prostate cancer post-treatment sequelae. J Men’s Health. 2014;11:95-107.
25. Parkin DM, Bray F, Ferlay J, et al. Global cancer statistics, 2002. CA Cancer J Clin. 2005;55:74-108.
26. American Cancer Society. Colorectal cancer facts and figures 2014-2016. Available from: http://www.cancer.org/acs/content/documents/document/acspc-042280.pdf. Accessed March 11, 2015.
27. Sargent D, Sobrero A, Grothey A, et al. Evidence for cure by adjuvant therapy in colon cancer: observations based on individual patient data from 20,898 patients on 18 randomized trials. J Clin Oncol. 2009;27:872-7.
28. Seo SI, Lim SB, Yoon YS, et al. Comparison of recurrence patterns between </=5 years and >5 years after curative operations in colorectal cancer patients. J Surg Oncol. 2013;108:9-13.
29. National Comprehensive Cancer Network. Clinical practice guidelines in oncology: colon cancer. Version 2.2015. Available from: http://www.nccn.org/professionals/physician_gls/pdf/colon.pdf. Accessed March 11, 2015.
30. National Comprehensive Cancer Network. Clinical practice guidelines in oncology: rectal cancer. Version 2.2015. Available from: http://www.nccn.org/professionals/physician_gls/pdf/rectal.pdf. Accessed March 20, 2015.
31. Desch CE, Benson AB, Somerfield MR, et al. Colorectal cancer surveillance: 2005 update of an American Society of Clinical Oncology practice guideline. J Clin Oncol. 2005;23:8512-9.
32. Anthony T, Simmang C, Hyman N, et al. Practice parameters for the surveillance and followup of patients with colon and rectal cancer. Dis Colon Rectum. 2004;47:807-17.
33. Cairns SR, Scholefield JH, Steele RJ, et al. Guidelines for colorectal cancer screening and surveillance in moderate and high-risk groups (update from 2002). Gut. 2010;59:666-89.
34. Frazier AL, Colditz GA, Fuchs CS, Kuntz KM. Cost-effectiveness of screening for colorectal cancer in the general population. JAMA. 2000;284:1954-61.
35. Rex DK, Kahi CJ, Levin B, et al. Guidelines for colonoscopy surveillance after cancer resection: a consensus update by the American Cancer Society and US Multi-Society Task Force on Colorectal Cancer. CA Cancer J Clin 2006;56:160-7.
36. Green RJ, Metlay JP, Propert K, et al. Surveillance for second primary colorectal cancer after adjuvant chemotherapy: an analysis of Intergroup 0089. Ann Intern Med. 2002;136:261-9.
37. Pfister DG, Benson AB, Somerfield MR. Clinical practice. Surveillance strategies after curative treatment of colorectal cancer. N Engl J Med 2004;350:2375-82.
38. Arnaud JP, Koehl C, Adloff M, et al. Carcinoembryonic antigen (CEA) in diagnosis and prognosis of colorectal carcinoma. Dis Colon Rectum. 1980;23:141-4.
39. Tsikiris VL, Malireddy K, Green EA, et al. Postoperative surveillance recommendations for early stage colon cancer based on results from the clinical outcomes of surgical therapy (COST) trial. J Clin Oncol. 2009;27:3671-6.
40. Tjandra JJ, Chan MK. Follow-up after curative resection of colorectal cancer: a meta-analysis. Dis Colon Rectum. 2007;50:1783-99.
41. Carpentier MY, Vernon SW, Bartholomew LK, et al. Receipt of recommended surveillance among colorectal cancer survivors: a systematic review. J Cancer Surviv. 2013;7:464-83.
42. Pietra N, Sarli L, Costi R, et al. Role of follow-up in management of local recurrences of colorectal cancer: a prospective, randomized study. Dis Colon Rectum 1998;41:1127-33.
43. Rodriguez-Moranta F, Salo J, Arcusa A, et al. Postoperative surveillance in patients with colorectal cancer who have undergone curative resection: a prospective, multicenter, randomized, controlled trial. J Clin Oncol 2006;24:386-93
44. Renehan AG, Egger M, Saunders MP, et al. Impact on survival of intensive follow up after curative resection for colorectal cancer: systemic review and meta-analysis of randomized trials. BMJ. 2002;324:813.
45. Jeffery M, Hickey BE, Hider PN. Follow-up strategies for patients treated for non-metastatic colorectal cancer. Cochrane Database Syst Rev. 2002;(1):CD002200
46. Ohlsson B, Breland U, Ekberg H, et al. Follow-up after curative surgery for colorectal carcinoma. Randomized comparison with no follow-up. Dis Colon Rectum. 1995;38:619-26.
47. Mäkelä JT, Laitinen SO, Kairaluoma MI. Five-year follow-up after radical surgery for colorectal cancer. Results of a prospective randomized trial. Arch Surg. 1995;130:1062-7.
48. Schoemaker D, Black R, Giles L, et al. Yearly colonoscopy, liver CT, and chest radiography do not influence 5-year survival of colorectal cancer patients. Gastroenterology. 1998;114:7-14.
49. Grossmann EM, Johnson FE, Virgo KS, et al. Follow-up of colorectal cancer patients after resection with curative intent-the GILDA trial. Surg Oncol. 2004;13:119-24.
50. Primrose JN, Perera R, Alastair G, et al. Effect of 3 to 5 years of scheduled CEA and CT follow-up to detect recurrence of colorectal cancer. The FACS randomized clinical trial. JAMA. 2014;311:263-70.
51. Wille-Jorgensen P, Lauerberg S, Pahlman L, et al. An interim analysis of recruitment to the COLOFOL trial. Colorectal Dis. 2009;11:756-8.
52. Secco GB, Fardelli R, Gianquinto D, et al. Efficacy and cost of risk-adapted follow-up in patients after colorectal cancer surgery: a prospective, randomized and controlled trial. Eur J Surg Oncol. 2002;28:418-23.
53. Bruinvels DJ, Stiggelbout AM, Kievit J, et al. Follow-up of patients with colorectal cancer. A meta-analysis. Ann Surg. 1994;219:174-82.
54. Berry DA, Cronin KA, Plevritis SK, et al. Effect of screening and adjuvant therapy on mortality from breast cancer. N Engl J Med. 2005;353:1784-92.
55. Piccart-Gebhart MJ, Burzykowski T, Buyse M, et al. Taxanes alone or in combination with anthracyclines as first-line therapy of patients with metastatic breast cancer. J Clin Oncol. 2008;26:1980-6.
56. van der Sangen MJ, Poortmans PM, Scheepers SW, et al. Prognosis following local recurrence after breast conserving treatment in young women with early breast cancer. Eur JS Surg Oncol. 2013;39:892-8.
57. National Comprehensive Cancer Network (NCCN). Clinical practice guidelines in oncology: breast cancer. Available from: http://www.nccn.org/professionals/physician_gls/pdf/breast.pdf. Accessed March 11, 2015.
58. Khatcheressian JL, Hurley P, Bantug E, et al. Breast cancer follow-up and management after primary treatment: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol. 2013;31;961-5.
59. Montgomery DA, Krupa A, Cooke TG. Follow-up in breast cancer: Does routine clinical examination improve outcome? A systematic review of the literature. Br J Cancer. 2007;97:1632-41.
60. Barton MB, Harris R, Fletcher SW. The rational clinical examination. Does this patient have breast cancer? The screening clinical breast examination: Should it be done? How? JAMA. 1999;282:1270-80.
61. Arasu VA, Joe BN, Lvoff NM, et al. Benefit of semiannual ipsilateral mammographic surveillance following breast conservation therapy. Radiology. 2012;264:371-7.
62. Lash TL, Fox MP, Silliman RA, et al. Reduced mortality rate associated with annual mammograms after breast cancer therapy. Breast J. 2006;12:2-6.
63. Schootman M, Jeffe DB, Lian M, et al. Surveillance mammogram and the risk of death among elderly breast cancer patients. Breast Cancer Res Treat. 2008;111:489-96.
64. Berg WA, Zhang Z, Lehrer D, et al. Detection of breast cancer with addition of annual screening ultrasound or a single screening MRI to mammography in women with elevated breast cancer risk. JAMA. 2012;307:1394-1404.
65. Isasi CR, Moadel RM, Blaufox MD, et al. A meta-analysis of FDG-PET for the evaluation of breast cancer recurrence and metastases. Breast Cancer Res Treat. 2005;90:105-12.
66. Kokko R, Holli K, Hakama M, et al. CA 15-3 in the follow-up of localised breast cancer: a prospective study. Eur J Cancer. 2002;38:1189-93.
67. GIVIO Investigators. Impact of follow-up testing on survival and health-related quality of life in breast cancer patients. A multicentre randomized controlled trial. JAMA. 1994;271:1587-92.
68. Del Turco RM, Palli D, Cariddi A, et al. Intensive diagnostic follow-up after treatment of primary breast cancer. A randomized trial. National Research Council Project on Breast Cancer Follow-up. JAMA. 1994;271:1593-7.
69. Palli D, Russo A, Saieva C, et al. Intensive vs clinical follow-up after treatment of primary breast cancer: 10 year update of a randomized trial. National Research Council Project on Breast Cancer Follow-up. JAMA. 1999;281:1586.
70. Joseph E, Hyacinthe M, Lyman GH, et al. Evaluation of an intensive strategy for follow-up and surveillance of primary breast cancer. Ann Surg Onc. 1998;5:522-8.
71. Keating NL, Landrum MB, Guadagnoli E, et al. Surveillance testing among survivors of early-stage breast cancer. J Clin Oncol. 2007;25:1074-81.
72. Ramsey SD, Henry NL, Gralow JR, et al. Tumor marker usage and medical care costs among older early-stage breast cancer survivors. J Clin Oncol. 2014;33:149-55.
73. Grunfeld E, Hodgson DC, Del Giudice ME, et al. Population-based longitudinal study of follow-up care for breast cancer survivors. J Oncol Pract. 2010;6:174-81.
74. Margenthaler JA, Allam E, Chen L, et al. Surveillance of patients with breast cancer after curative-intent primary treatment: current practice patterns. J Oncol Pract. 2012;8:79-83.
75. American Board of Internal Medicine. Choosing Wisely Campaign. Available from: http://www.choosingwisely.org. Accessed March 11, 2015.