Reviving the Acid Phosphatase Test for Prostate Cancer
Prostatic acid phosphatase (PAP) emerged as the world's first clinically useful tumor marker in the 1940s and 1950s. With the introduction of the prostate-specific antigen (PSA) test in the 1980s, which performed significantly better than PAP in terms of screening and monitoring response to treatment, PAP fell into disfavor. An increasing number of recent studies have identified PAP as a significant prognostic factor for patients with intermediate- and high-risk prostate cancer. PAP appears to be particularly valuable in predicting distant failure in higher-risk patients for whom high levels of local control are achieved with aggressive initial local treatment. As prostate cancer care becomes increasingly focused on identifying the minority of patients who would benefit from aggressive systemic therapy, a reevaluation of the potential contribution of the prostatic acid phosphatase test seems timely.
ABSTRACT: Prostatic acid phosphatase (PAP) emerged as the world's first clinically useful tumor marker in the 1940s and 1950s. With the introduction of the prostate-specific antigen (PSA) test in the 1980s, which performed significantly better than PAP in terms of screening and monitoring response to treatment, PAP fell into disfavor. An increasing number of recent studies have identified PAP as a significant prognostic factor for patients with intermediate- and high-risk prostate cancer. PAP appears to be particularly valuable in predicting distant failure in higher-risk patients for whom high levels of local control are achieved with aggressive initial local treatment. As prostate cancer care becomes increasingly focused on identifying the minority of patients who would benefit from aggressive systemic therapy, a reevaluation of the potential contribution of the prostatic acid phosphatase test seems timely.
Most prostate cancers are detected at an early stage, and most patients are cured by surgery or radiation. However, nearly 30% of patients with early-stage disease go on to develop biochemical failure, and many of these men will eventually die from hormone-refractory disease.[1,2] In absolute terms, prostate cancer is still the third leading cause of cancer mortality among men in the United States, with an estimated 27,000 deaths in 2006.[2] Thus, while most men are cured by primary treatment, a subset would likely benefit from more aggressive (adjuvant) treatment.
Systemic therapeutic options for prostate cancer are improving.[3] But because adjuvant therapies often entail significant adverse side effects, it is important to identify patients who are most likely to benefit. The use of higher prostate-specific antigen (PSA) levels or higher Gleason scores as criteria for adjuvant therapy is suboptimal for this purpose, because the majority of patients with markedly elevated PSA or Gleason scores are still curable with effective local therapy.[4,5] A number of older and more recent studies suggest that prostatic acid phosphatase (PAP) could play a role in determining which early-stage patients are likely to benefit from more aggressive adjuvant therapy.
Measuring Prostatic Acid Phosphatase
Acid phosphatases are a group of five ubiquitous tissue isoenzymes that hydrolyze organic monophosphate esters. They are present in many human tissues including platelets, lung, osteoclasts, erythrocytes, liver, and kidney.[6,7] However, prostate-specific acid phosphatase is over 100 times more abundant in the prostate than in other tissue types.[8]
Enzymatic reactions using phosphomonoester substrates were developed to measure serum acid phosphatase concentrations. The original tests were unable to differentiate between prostatic and other tissue sources. A variety of techniques were developed to improve sensitivity, such as adding L-tartrate, which somewhat selectively inhibited prostatic acid phosphatase. In 1971, Roy developed what is considered to be the most prostate-specific of the enzymatic reactions utilizing thymolphthalein phosphate.[9]
The enzymatic assays have recognized technical limitations. They are unstable at room temperature, requiring immediate freezing or buffering. There is diurnal and random variability. And there is a low sensitivity for early-stage disease.[9,10] Radioimmunoassays were developed in the 1970s with somewhat greater sensitivity and in vitro specificity, but they are subject to some of the same limitations as the enzymatic tests.[7,10]
A significant perceived limitation of PAP as a cancer marker is the fact that levels can be artificially elevated in the setting of nonprostatic disease or benign conditions of the prostate. Paget's disease, hyperparathyroidism, Gaucher's disease, multiple myeloma, and other malignancies associated with skeletal metastases, prostatitis, and prostatic infarcts can cause increases in serum PAP.[6,11] There are also conflicting reports of prostatic massage leading to transient PAP elevation that returns to normal within 24 to 48 hours. Other research suggests that less aggressive routine digital rectal exams may not cause this transient rise.[6,8] Modest PAP elevations have been identified in a minority of men with benign prostatic hypertrophy (BPH),[12] although this is more common with the radioimmunoassays than the enzymatic tests.[11,13] Overall, the clinical significance of these potentially artificially elevated levels is probably not great, but needs to be better defined.
Pre-PSA Era
FIGURE 1

Prostatic Acid Phosphatase Timeline
In 1938, Gutman and Gutman reported increased levels of acid phosphatase in patients with metastatic prostate cancer.[14] Shortly thereafter, Huggins and Hodges[15] discovered that men with prostate cancer treated by orchiectomy or estrogen injections experienced regression of their clinical disease, correlated with a significant decrease in their acid phosphatase levels. These findings formed the foundation of current androgen deprivation strategies. They also established acid phosphatase as a tumor marker for prostate cancer (Figure 1).
From the 1950s through the 1980s, acid phosphatase was widely used to detect, stage, and monitor prostate cancer treatment response, with some success.[8] In 1984, Whitesel and colleagues reported that elevated PAP levels corresponded with a high risk of occult pelvic metastases and subsequent bone metastases.[16] They recommended creating a new clinical stage for prostate cancer (D0) for patients with elevated PAP but no clinical evidence of metastasis. Elevated pretreatment PAP levels were considered to be a relative contraindication to surgery. National Prostatic Cancer Project investigators reported that survival was significantly shorter for patients with elevated acid phosphatase.[17] Several investigators demonstrated that posttreatment PAP could also be used to monitor response to therapy.[18,19] Although PAP proved moderately useful, researchers were interested in finding more sensitive markers that could identify patients at an earlier stage, when disease was curable.
Prostate-specific antigen was first isolated in seminal plasma in 1971. By the 1980s, investigators at the Roswell Park Memorial Institute demonstrated that elevated serum PSA levels were associated with BPH and prostate cancer.[12] PSA was quickly compared against PAP as a prostate cancer biomarker.
Screening With PSA vs PAP
PAP had long been known to have a low sensitivity for diagnosing new disease.[8] Stamey compared PSA to PAP and found a 45% sensitivity for PAP compared to 96% for PSA. PAP sensitivity was particularly low for patients with early-stage disease (0% for stage A, 9% for stage B1).[12] Since the goal of prostate cancer screening is to identify early-stage treatable disease, PAP was rightly dropped as a screening tool.
Staging With PSA vs PAP
In older series from the pre-PSA era, elevated pretreatment PAP had a high specificity for advanced-stage disease. However, PAP's sensitivity for advanced disease was only 50% to 80%,[10,20] meaning that normal serum PAP levels were not accepted as convincing proof of early-stage disease. Staging comparisons of PAP vs PSA showed that the latter was a better predictor of primary tumor volume, extent of capsular penetration and pretreatment clinical stage.[21]
Questions were raised regarding how much additional staging information PAP provided beyond PSA and clinical exam. Johns Hopkins investigators[22] reported that only 4.6% of 460 patients evaluated for prostatectomy had an elevated PAP. All patients with an elevated PAP were found to have extracapsular disease at the time of prostatectomy. However, 81% of patients with an elevated PAP were also identified as having extracapsular spread by either a PSA greater than 100 ng/mL or unequivocal extracapsular extension by digital rectal exam. Hence, PAP provided unique information on only 0.9% of the 460 patients.
In 1987, Stamey et al demonstrated the advantages of PSA over PAP to evaluate and monitor newly diagnosed prostate cancer patients.[12] In 1984, 62% of men worked up for prostate cancer had a PAP serum level drawn vs 5% who had PSA tested. By 1990, only 3 years after the Stamey article, the number of men having PAP included in their initial evaluation was down to 47%, whereas PSA was checked in 66%.[23] By the mid-1990s, serum PAP was declared to have "no practical role in the clinical staging of newly diagnosed prostate cancer."[24]
Monitoring Disease Recurrence
PAP also is clearly inferior to PSA in identifying subclinical disease persistence after prostatectomy or radiation therapy.[10] After prostatectomy, PSA levels nearly always drop to undetectable levels in the absence of residual disease. PAP, on the other hand, commonly remains in the detectable range after prostatectomy, because of other tissue sources. As a result, PAP is not a sensitive marker for residual, subclinical disease.
Clinical recurrence is almost always preceded by a rising PSA. PAP, on the other hand, frequently remains in the normal range, even in the presence of clinically evident metastases. Oesterling and colleagues reported that 100% of patients with clinically evident recurrence had elevated PSA levels, while only 50% had an elevated PAP.[25] National Prostatic Cancer Project investigators reported that almost a quarter of patients with clinically evident metastatic disease had normal PAP.[17]
Demise of PAP
PAP's fall from favor was primarily due to its poor sensitivity for screening or as an indicator of persistent disease. In the process of substituting PSA as a screening and monitoring tool, PAP's strength as a prognostic marker was overlooked. Recently published predictive nomograms and risk categorization models ignore it.[26-29] But PAP may still turn out to be a clinically valuable tool.
Predicting Biochemical Control
FIGURE 2
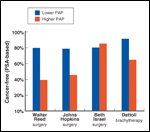
Freedom From Biochemical FailureFIGURE 3
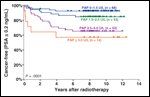
Freedom From Biochemical Failure After Radiotherapy
In contrast to PAP's inferiority in staging and posttreatment monitoring functions, an elevated pretreatment PAP has consistently been identified as a significant prognostic factor.[17,30,31] In the PSA era, Walter Reed investigators studied 295 higher-risk prostatectomy patients. Those with an elevated preprostatectomy PAP had only a 39% 4-year biochemical disease-free survival vs 79% for patients with a normal PAP. Patients with elevated PAP had significantly lower disease-free survival across all PSA levels.[32] Johns Hopkins investigators reviewed 1,600 patients and also identified pretreatment PAP as an independent prognostic factor, with a hazard ratio for biochemical failure similar to that of PSA.[33] The only recent surgical series that did not identify PAP as a predictor of cancer recurrence was one from Beth Israel Deaconess (Figure 2).[34] However, their negative finding was in a homogeneously low-risk population of 180 patients with very few recurrences.
Similar to the surgical series, Dattoli and colleagues reported in 2003 that pretreatment PAP was a stronger predictor of biochemical failure than PSA or Gleason score after palladium (Pd)-103 brachytherapy in 161 higher-risk patients.[35] PAP was particularly useful in stratifying risk level of patients with PSAs between 4 and 20 ng/mL. Recently published long-term follow-up of this cohort confirms the initial findings (Figure 3).[36]
Predicting Clinical Recurrence and Prostate Cancer Death
Most patients with prostate cancer, regardless of therapy, die of other causes. With concern for overtreatment of early-stage patients, there is increasing emphasis on identifying long-term risk of clinical recurrence and prostate cancer-specific death. Fowler evaluated 138 veterans treated surgically between 1980 and 1991, and found that PAP was a significant predictor of biochemical failure and clinical recurrence.[37] In a 1993 analysis of 874 patients treated at M.D. Anderson,[38] PAP was found to be an independent predictor of clinical recurrence and distant metastasis.
A more recent study of a 938 men treated with radiation-only at M.D. Anderson[39] found PAP to be predictive for biochemical disease-free survival in univariate but not multivariate analysis. Interestingly, in the more recent study (as opposed to the earlier M.D. Anderson series), local recurrence-not metastatic disease-was the dominant cause of failure. However, even in that study, patients with elevated PAP remained at much higher risk for developing metastatic disease (38%) than patients with high-normal (14%) or low (3%) PAP levels. A review of long-term survival in four Radiation Therapy Oncology Group trials showed that elevated PAP was significantly associated with decreased disease-specific and overall survival.[40]
FIGURE 4
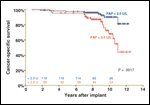
Prostate Cancer-Specific Survival
Dattoli and colleagues have recently found that an elevated PAP is the single strongest independent predictor of prostate cancer-specific death.[41,51] Patients with elevated pretreatment PAP had a 12-year cancer-specific survival of 45% vs 82% for those with a lower PAP (Figure 4). Of note, the Dattoli cohort was a higher-risk group with particularly good local control. It appears that, in reviewing the above studies, PAP performs best in patients who, if they fail, are most likely to fail distantly.
PAP in Staging
FIGURE 5
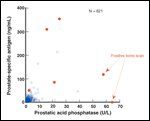
Scatter Plot of Prostate-Specific Antigen vs Prostatic Acid Phosphatase
Bone scans have become a less routine part of prostate cancer evaluation, as PSA screening has led to detection of earlier-stage disease.[42] Although PAP is not useful for predicting extracapsular (periprostatic) disease, it appears to provide useful information regarding the use of bone scans. For patients with double-digit PSA at diagnosis, PAP may be a valuable adjunctive tool with which to detect bone metastases. Merrick and colleagues[43] showed that PAP may, in fact, be a better discriminator of bone metastases than PSA (Figure 5). The precise role of PAP in conjunction with PSA and bone scans needs to be clarified. It seems likely that both serum markers could be useful in guiding the judicious use of bone scans in patients with higher-risk features.
Is PAP a Marker for Today's Challenges?
In past reports, PAP was most effective as a prognostic factor in patient cohorts with a relatively high proportion of distant failures. In studies from the pre-PSA era that identified PAP as a prognostic factor, patients presented with more advanced disease and a significant distant failure rate. In more recent literature, PAP was most significant in patients at higher risk for both local and distant failure but who achieved high rates of local control. PAP was less useful in low-risk patients who had little likelihood of developing distant disease (eg, San Francisco et al[34]) or in higher-risk patients with high local recurrence rates after external-beam radiotherapy (eg, Zagars et al[39]). Given the improved local control rates now attainable with intensity-modulated radiation therapy or brachytherapy, the predictive ability of PAP for distant failure should become increasingly evident.
Technical advances over the past 15 years have led to remarkably high cure rates for early-stage prostate cancer.[44,45] Patients with PSA levels above 20 ng/mL and/or Gleason scores ≥ 8 have not fared as well in many series, but the cure rate even for these higher-risk patients has been encouragingly high, particularly in recent brachytherapy cohorts.[4,5] It appears that with improved local treatment, patterns of failure are changing. Failures in these patients tend to be distant and exhibit biologically aggressive behavior.[5] Thus, while many higher-risk patients may not need adjuvant treatment, the subset of patients who are destined to fail will have increasingly aggressive disease.
In the setting of more effective local therapy, a specific indicator like PAP may be increasingly valuable in identifying the small minority of higher-risk patients who harbor occult metastases and could benefit from adjuvant systemic therapy. The specificity of PSA and Gleason scores for micrometastatic disease is limited. In contrast, old and new studies suggest that PAP appears to be particularly correlated with the likelihood of developing systemic disease. PAP is the only prognostic marker that does not predict for local recurrence or periprostatic extracapsular extension, but continues to significantly predict overall disease recurrence.[32,33,38] Based on PAP's poor performance in predicting local recurrence or extension but its significance as a predictor of disease relapse, it appears that PAP is serving as a marker primarily for relapses secondary to pretreatment occult disease.
What Is PAP Measuring?
While PAP is predictive of patients' propensity to develop distant metastases, it is unlikely that PAP is actually measuring subclinical metastases. We know that PSA is more sensitive to small-volume disease, and occult metastases are by definition small volume. And PAP levels typically return to normal after local treatment, suggesting that the source of the measured PAP is mainly from the primary tumor. PAP is a more specific marker for the potential of a tumor to have already spread microscopically prior to treatment. In this regard, PAP seems to be more akin to Gleason score than to PSA.
FIGURE 6
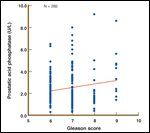
Scatter Plot of Prostatic Acid Phosphatase and Gleason Score
Investigators have reported only a weak relationship between PSA/Gleason score and PAP.[46] Zagars calculated the correlation coefficient between PSA and PAP to be only 0.35.[47] Dattoli found the correlation coefficient between Gleason score and PAP to be only 0.34 (Figure 6).[41,48] This suggests that there is the potential to garner unique information from each. In particular, there will be many patients who are classified as moderate to high risk by PSA and Gleason for whom PAP levels may be able to more accurately stratify risk categories.
Outstanding Issues
Our purpose in writing this review is to bring attention to PAP as a useful marker. If the test is reintroduced, there are several issues that need to be addressed. First, more clinical series need to be published, to corroborate the few series with relatively contemporary treatment.
A second issue needing more effort is better standardization and characterization of how PAP is measured. Several serum quantification methods have been reported to have some prognostic ability. Immunologic assays, rather than the Roy enzymatic assay used in most reports, have been more sensitive but less clinically specific than the Roy technique.[49] Quantitative PAP tissue-staining has also been shown to significantly predict survival.[50] No studies have compared these alternative methods to the enzymatic method in terms of prostate cancer deaths or biochemical failure. The merits of alternative serum assays or tissue-staining relative to the Roy method for identifying patients at high risk for recurrent disease needs to be better worked out. Current, more sophisticated immunologic technologies available today may also give a clearer, more specific quantification of prostate-specific acid phosphatase.
Finally, if PAP is to be reintroduced in the initial diagnostic work-up of prostate cancer patients, it probably should only be used in patients who are deemed intermediate to high risk by other criteria (PSA, Gleason score, and stage). Based on our review of the literature, PAP will not be meaningfully discerning for patients at baseline low risk of occult metastatic disease.
Financial Disclosure:The authors have no significant financial interest or other relationship with the manufacturers of any products or providers of any service mentioned in this article.
References:
1. Lu-Yao GL, Potosky AL, Albertsen PC, et al: Follow-up prostate cancer treatments after radical prostatectomy: A population-based study. J Natl Cancer Inst 88:166-173, 1996.
2. Jemal A, Siegel R, Ward E, et al: Cancer statistics, 2006. CA Cancer J Clin 56:106-130, 2006.
3. Pienta KJ, Smith DC: Advances in prostate cancer chemotherapy: A new era begins. CA Cancer J Clin 55:300-318, 2005.
4. Copp H, Bissonette EA, Theodorescu D: Tumor control outcomes of patients treated with trimodality therapy for locally advanced prostate cancer. Urology 65:1146-1151, 2005.
5. Stock RG, Ho A, Cesaretti JA, et al: Changing the patterns of failure for high-risk prostate cancer patients by optimizing local control. Int J Radiat Oncol Biol Phys 66:389-394, 2006.
6. Romas NA: Prostatic acid phosphatase: Current concepts. Semin Urol 1:177-185, 1983.
7. Foti AG, Herschman H, Cooper JF: Comparison of human prostatic acid phosphatase by measurement of enzymatic activity and by radioimmunoassay. Clin Chem 23:95-99, 1977.
8. Heller JE: Prostatic acid phosphatase: Its current clinical status. J Urol 137:1091-1103, 1987.
9. Roy AV, Brower ME, Hayden JE: Sodium thymolphthalein monophosphate: A new acid phosphatase substrate with greater specificity for the prostatic enzyme in serum. Clin Chem 17:1093-1102, 1971.
10. Lowe FC, Trauzzi SJ: Prostatic acid phosphatase in 1993. Its limited clinical utility. Urol Clin North Am 20:589-595, 1993.
11. Gutman AB: The development of the acid phosphatase test for prostatic carcinoma: The sixth Ferdinand C. Valentine memorial lecture. Bull N Y Acad Med 44:63-76, 1968.
12. Stamey TA, Yang N, Hay AR, et al: Prostate-specific antigen as a serum marker for adenocarcinoma of the prostate. N Engl J Med317:909-916, 1987.
13. Foti AG, Cooper JF, Herschman H, et al: Detection of prostatic cancer by solid-phase radioimmunoassay of serum prostatic acid phosphatase. N Engl J Med 297:1357-1361, 1977.
14. Gutman AB, Gutman EB: An "acid" phosphatase occurring in the serum of patients with metastasizing carcinoma of the prostate gland. J Clin Invest 17:473-478, 1938.
15. Huggins C, Hodges CV: Studies on prostatic cancer. I. The effect of castration, of estrogen and androgen injection on serum phosphatases in metastatic carcinoma of the prostate. Cancer Res 1:293-297, 1941.
16. Whitesel JA, Donohue RE, Mani JH, et al: Acid phosphatase: Its influence on the management of carcinoma of the prostate. J Urol 131:70-72, 1984.
17. Johnson DE, Prout GR, Scott WW, et al: Clinical significance of serum acid phosphatase levels in advanced prostatic carcinoma. Urology 8:123-126, 1976.
18. Paulson DF, Berry WR, Cox EB, et al: Treatment of metastatic endocrine-unresponsive carcinoma of the prostate gland with multiagent chemotherapy: Indicators of response to therapy. J Natl Cancer Inst 63:615-622, 1979.
19. Vihko P, Kontturi M, Lukkarinen O, et al: Immunoreactive prostatic acid phosphatase in prostatic cancer: Diagnosis and followup of patients. J Urol 133:979-982, 1985.
20. Reif AE, Schlesinger RM, Fish CA, et al: Acid phosphatase isozymes in cancer of the prostate. Cancer 31:689-699, 1973.
21. Stamey TA, Kabalin JN, McNeal JE, et al: Prostate specific antigen in the diagnosis and treatment of adenocarcinoma of the prostate. II. Radical prostatectomy treated patients. J Urol 141:1076-1083, 1989.
22. Burnett AL, Chan DW, Brendler CB, et al: The value of serum enzymatic acid phosphatase in the staging of localized prostate cancer. J Urol 148:1832-1834, 1992.
23. Jones GW, Mettlin C, Murphy GP, et al: Patterns of care for carcinoma of the prostate gland: Results of a national survey of 1984 and 1990. J Am Coll Surg 180:545-554, 1995.
24. O'Dowd GJ, Veltri RW, Orozco R, et al: Update on the appropriate staging evaluation for newly diagnosed prostate cancer. J Urol 158:687-698, 1997.
25. Oesterling JE: Prostate specific antigen: A critical assessment of the most useful tumor marker for adenocarcinoma of the prostate. J Urol 145:907-923, 1991.
26. Cooperberg MR, Pasta DJ, Elkin EP, et al: The University of California, San Francisco cancer of the prostate risk assessment score: A straightforward and reliable preoperative predictor of disease recurrence after radical prostatectomy. J Urol 173:1938-1942, 2005.
27. Freedland SJ, Terris MK, Csathy GS, et al: Preoperative model for predicting prostate specific antigen recurrence after radical prostatectomy using percent of biopsy tissue with cancer, biopsy gleason grade and serum prostate specific antigen. J Urol 171:2215-2220, 2004.
28. Nelson CP, Rubin MA, Strawderman M, et al: Preoperative parameters for predicting early prostate cancer recurrence after radical prostatectomy. Urology 59:740-746, 2002.
29. Stephenson AJ, Scardino PT, Eastham JA, et al: Preoperative nomogram predicting the 10-year probability of prostate cancer recurrence after radical prostatectomy. J Natl Cancer Inst 98:715-717, 2006.
30. Berry WR, Laszlo J, Cox E, et al: Prognostic factors in metastatic and hormonally unresponsive carcinoma of the prostate. Cancer 44:763-775, 1979.
31. Ganem EJ: The prognostic significance of an elevated serum acid phosphatase level in advanced prostatic carcinoma. J Urol 76:179-181, 1956.
32. Moul JW, Connelly RR, Perahia B, et al: The contemporary value of pretreatment prostatic acid phosphatase to predict pathological stage and recurrence in radical prostatectomy cases. J Urol 159:935-940, 1998.
33. Han M, Piantadosi S, Zahurak ML, et al: Serum acid phosphatase level and biochemical recurrence following radical prostatectomy for men with clinically localized prostate cancer. Urology 57:707-711, 2001.
34. San Francisco IF, Olumi AF, Yoon JH, et al: Preoperative serum acid phosphatase and alkaline phosphatase are not predictors of pathological stage and prostate-specific antigen failure after radical prostatectomy. BJU Int 92:924-928, 2003.
35. Dattoli M, Wallner K, True L, et al: Long-term outcomes after treatment with external beam radiation therapy and palladium 103 for patients with higher risk prostate carcinoma: Influence of prostatic acid phosphatase. Cancer 97:979-983, 2003.
36. Dattoli M, Wallner K, True L, et al: Long-term prostate cancer control using palladium-103 brachytherapy and external beam radiotherapy in patients with a high likelihood of extracapsular cancer extension. Urology 69:334-337, 2007.
37. Fowler JE Jr, Braswell NT, Pandey P, et al: Experience with radical prostatectomy and radiation therapy for localized prostate cancer at a Veterans Affairs Medical Center. J Urol 153:1026-1031, 1995.
38. Zagars GK, von Eschenbach AC, Ayala AG: Prognostic factors in prostate cancer. Analysis of 874 patients treated with radiation therapy. Cancer 72:1709-1725, 1993.
39. Zagars GK, Pollack A, von Eschenbach AC: Prognostic factors for clinically localized prostate carcinoma: Analysis of 938 patients irradiated in the prostate specific antigen era. Cancer 79:1370-1380, 1997.
40. Roach M 3rd, Lu J, Pilepich MV, et al: Long-term survival after radiotherapy alone: Radiation Therapy Oncology Group prostate cancer trials. J Urol 161:864-868, 1999.
41. Wallner K, Merrick G, Blasco J, et al: Prostate Brachytherapy Made Complicated, 3rd ed. Seattle, SmartMedicine Press, 2007.
42. Oesterling JE, Martin SK, Bergstralh EJ, et al: The use of prostate-specific antigen in staging patients with newly diagnosed prostate cancer. JAMA 269:57-60, 1993.
43. Merrick GS, Butler WM, Wallner K, et al: Enzymatic prostatic acid phosphatase in the clinical staging of patients diagnosed with prostate cancer. W V Med J 101:116-119, 2005.
44. Kupelian PA, Buchsbaum JC, Elshaikh MA, et al: Improvement in relapse-free survival throughout the PSA era in patients with localized prostate cancer treated with definitive radiotherapy: Year of treatment an independent predictor of outcome. Int J Radiat Oncol Biol Phys 57:629-634, 2003.
45. Han M, Partin AW, Piantadosi S, et al: Era specific biochemical recurrence-free survival following radical prostatectomy for clinically localized prostate cancer. J Urol 166:416-419, 2001.
46. Shih WJ, Gross K, Mitchell B, et al: Prostate adenocarcinoma using gleason scores correlates with prostate-specific antigen and prostate acid phosphatase measurements. J Natl Med Assoc 84:1049-1050, 1992.
47. Zagars GK, Pollack A, Kavadi VS, et al: Prostate-specific antigen and radiation therapy for clinically localized prostate cancer. Int J Radiat Oncol Biol Phys 32:293-306, 1995.
48. Dattoli M, Wallner K, True L, et al: Prognostic role of serum prostatic acid phosphatase for 103Pd-based radiation for prostatic carcinoma. Int J Radiat Oncol Biol Phys 45:853-856, 1999.
49. Griffiths JC: Prostate-specific acid phosphatase: Re-evaluation of radioimmunoassay in diagnosing prostatic disease. Clin Chem 26:433-436, 1980.
50. Zhou R, Sause WT, Hammond EH, et al: Correlation of survival with quantitative tissue staining of prostate specific acid phosphatase in patients with prostate carcinoma by using microscopic image analysis: A preliminary report of correlative studies on RTOG protocols 75-06, 77-06, and 83-07. Int J Radiat Oncol Biol Phys 33:823-829, 1995.
51. Fang LC, Dattoli M, Wallner K, et al: Prostatic acid phosphatase predicts cancer-specific survival after palladium-103 brachytherapy for prostate cancer. Brachytherapy 6:79-80, 2007.