Stereotactic Radiation Therapy Combined With Immunotherapy: Augmenting the Role of Radiation in Local and Systemic Treatment
In this review we detail the rationale supporting a combination of immunotherapy and stereotactic radiation. Additionally, we discuss the evidence for the immune stimulatory effects of focused radiation and the role that radiation may play in enhancing the systemic treatment effects of immunotherapy.
Figure 1: Potential Immune-Stimulatory Effects of Stereotactic Radiosurgery (SRS)
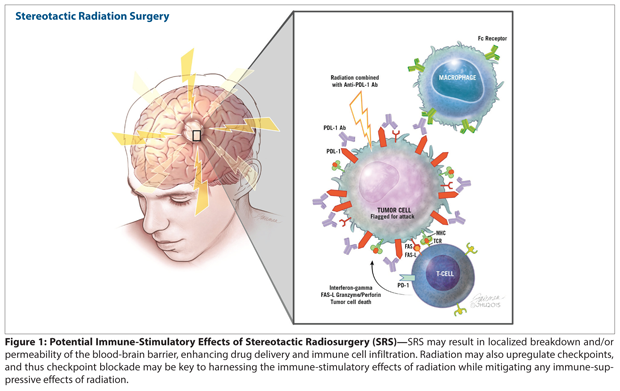
Figure 2: Potential Immune-Stimulatory Effects of SBRT for Lung Tumors
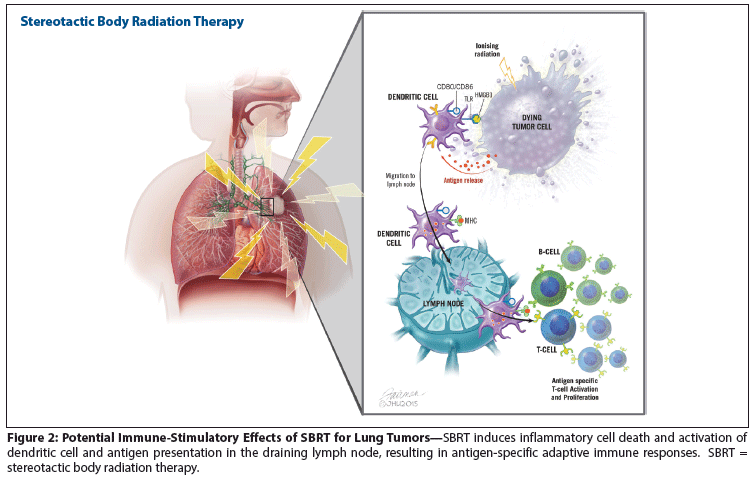
Stereotactic radiosurgery and stereotactic body radiation therapy are two contemporary radiation modalities that can treat tumors in any area of the body using highly focused radiation. Recently, immunotherapy has established itself as a viable and powerful anticancer treatment. In this review we detail the rationale supporting a combination of immunotherapy and stereotactic radiation. Additionally, we discuss the evidence for the immune stimulatory effects of focused radiation and the role that radiation may play in enhancing the systemic treatment effects of immunotherapy.
Introduction
Radiation therapy has a long and established history in the field of oncology.[1] The term stereotactic radiation-or stereotaxy-refers to the use of a referenced three-dimensional coordinate system to locate targets inside the body and deliver highly focused beams of radiation to that site with millimeter accuracy.
Swedish neurosurgeon Dr. Lars Leksell was a pioneer of stereotactic neurosurgery and the inventor of stereotactic radiosurgery.[2] Dr. Leksell created a stereotactic frame that used a polar coordinate system and a “center-of-arc” concept that was more versatile than the Cartesian coordinate system used by previous stereotactic devices.[3] In 1948 Dr. Leksell used his stereotactic system for the first time in the treatment of a patient with a craniopharyngioma, where the frame guided injection of radioactive phosphorus into the cyst. Dr. Leksell introduced the term stereotactic radiosurgery (SRS) in 1951 to describe the use of multiple beams of radiation incident on a single point as a noninvasive method of ablating tissue in the brain, in lieu of traditional surgery.[2] In 1967 he inaugurated the “Gamma Knife,” as it is known today, which uses hundreds of Cobalt-60 sources, all focused on a single point stereotactically referenced to the patient’s skull using a fixed frame. This device has been updated and modified over the years and is still an important tool today. Importantly, because of its design, the Gamma Knife is essentially limited to targeting intracranial lesions. The CyberKnife® was developed by Dr. John R. Adler at Stanford University and uses a miniaturized linear accelerator mounted on a general-purpose industrial robot to deliver precision radiation with sub-millimeter accuracy. The CyberKnife® was designed to deliver stereotactic radiation to any part of the body.[4] Stereotactic delivery of radiation is usually termed “stereotactic body radiation therapy” (SBRT); it is also called stereotactic ablative body radiation therapy, although for this review we will use the acronym SBRT. Importantly, SBRT can also be delivered using standard linear accelerators equipped and commissioned for stereotactic treatment.
Because of the accuracy and ability of SRS to precisely modify the radiation dose distribution to minimize radiation to normal tissue, it allows for hypofractionation-delivery of very high doses of radiation during each fraction of treatment. In the United States, clinical stereotactic radiation courses are currently completed in 1 to 5 fractions total, with each fraction taking approximately 1 hour to complete. This is a dramatic shortening of total treatment duration compared with conventionally fractionated radiation, which can take from 2 to 8 weeks to complete. (Conventional fractionation is delivered in 10 to 40 fractions, with each fraction taking 15 to 20 minutes to complete.) The ability to effectively treat patients’ tumors anywhere in the body with SBRT, using high tumoricidal doses while limiting dose to surrounding normal structures, has been a major advance and a fundamental shift in the field of radiation oncology.[5] Aside from patient convenience and the ability to resume or transition more rapidly to other therapies, such as surgery or systemic therapy, there are also important radiobiologic effects of delivering high doses per fraction, which are thought to increase the therapeutic ratio of SBRT. Clinically, stereotactic radiation achieves excellent local control rates, for example, for arteriovenous malformation,[6] trigeminal neuralgia,[7] pituitary adenoma,[8] and brain metastases.[9] SBRT for early-stage lung cancer has local control rates rivaling those of surgery.[10] SBRT is also actively being studied in the treatment of prostate cancer, with excellent early control rates, and is being used in numerous other tumors, including cancers of the pancreas, liver, kidney, and CNS.
Immune Stimulatory Effects of Radiation
Large radiation fields encompassing significant volumes of bone marrow or blood pool have been observed to result in decreases in white blood cell counts, giving rise to the notion that radiation may be generally immunosuppressive.[11,12] There have even been reports of decreased blood cell counts after SBRT to the lung, although this effect correlated with the amount of vertebral body irradiated, and counts began to recover 4 weeks after therapy.[13] Nonetheless, with the application of SRS and SBRT, there is the possibility of significantly limiting the volume of bone marrow and/or blood pool being irradiated, thereby minimizing these potentially consequential immunosuppressive effects. This significant advance in radiation technology and capability calls for a re-evaluation of the effects of focused radiation on the immune system.
There is now an established body of preclinical literature demonstrating that radiation can modify antitumor immune responses. Radiation has been demonstrated to cause upregulation of major histocompatibility complexes (MHCs) and to increase presentation of antigens on the surface of tumor cells.[14-19] The DNA damage and reactive oxygen species induced by radiation have been shown to result in inflammatory tumor cell death and release of damage-associated molecular patterns, including high mobility group box chromosomal protein 1 (HMGB1), which can activate antigen-presenting cells.[20-22] Radiation-induced activation of antigen-presenting cells has also been demonstrated in animal models to enhance tumor antigen cross-presentation in the draining lymph node, resulting in activation and proliferation of tumor-specific cytotoxic T cells.[18,23-28] Radiation has also been shown to influence expression of cytokines and chemokines, such as interleukin (IL)-1, IL-2, IL-6, tumor necrosis factor (TNF)-alpha, transforming growth factor (TGF)-beta, chemokine (C-X-C motif) ligand 16 (CXCL-16), as well as type I and type II interferons, which may play a critical role in modulating immune responses.[29-36] Undoubtedly as the cumulative result of these effects, multiple groups have demonstrated that radiation can cause tumor cells to become more susceptible to immune-mediated attack.[15,16,37] Indeed, some authors have suggested that the therapeutic effects of radiation alone may depend on the status of the host immune system and antitumor immune responses in the radiation field.[25,34,38-40] Given these effects, which can occur when using radiation alone, there has been a significant effort to combine radiation with various immunotherapies, with sometimes striking results within the radiation field (radiosensitizing immunotherapy), as well as distantly outside the radiation field (abscopal responses).[15,18,24,36,37,40-49] A number of excellent reviews have also highlighted the potential benefits and ongoing clinical trials of radiation combined with immunotherapy.[32,50-54]
Checkpoint Blockade Immunotherapy
Over the past 5 years, cancer immunotherapy has achieved some major successes, including being designated as breakthrough of the year in 2013 by Science magazine.[55] Multiple types of immunotherapy have garnered significant attention recently, including dendritic cell vaccines, T-cell adoptive transfer, and checkpoint blockade immunotherapy (CBI). The recent momentum began in 2010, when the US Food and Drug Administration (FDA) granted approval to sipuleucel-T for minimally symptomatic metastatic castration-resistant prostate cancer (CRPC). Notably, sipuleucel-T was the first therapeutic dendritic cell–based vaccine approved for any cancer type. In 2011, the FDA granted approval to the anti–cytotoxic lymphocyte antigen 4 (CTLA-4) drug ipilimumab for the treatment of unresectable or metastatic melanoma, and in September 2014, the anti–programmed death 1 (PD-1) drug pembrolizumab was approved by the FDA for the same indication. In December 2014, the FDA granted accelerated approval to the anti–PD-1 drug nivolumab for patients with progressive unresectable or metastatic melanoma; in March 2015, the approved use of nivolumab was expanded to include treatment of patients with advanced (metastatic) squamous non–small-cell lung cancer (NSCLC) with progression on or after platinum-based chemotherapy. Notably, nivolumab is the first CBI approved for lung cancer. Additional CBI antibodies in development include: tremelimumab, which targets CTLA-4; MPDL3280A, which targets the PD-1 ligand (PD-L1); MEDI4736, which targets PD-L1; lirilumab, which targets the killer inhibitory receptor (KIR); and BMS-986016, which targets the checkpoint molecule lymphocyte-activation gene 3 (LAG-3).
The significant interest in CBI stems from the dramatic and durable responses observed in a subset of patients with metastatic disease who were heavily pretreated. At its core, CBI functions to inhibit negative regulators of immune responses; in other words, it removes the brakes on the immune system. For decades, immunotherapy approaches have focused on attempting to positively stimulate the immune responses without necessarily addressing the powerful negative regulatory systems that are in place that dampen or prevent excessive immune responses. It is now understood that disabling these negative regulators or checkpoints can result in robust and clinically efficacious immune responses, which in some cases can control widely metastatic disease. CTLA-4 is a receptor present on the surface of T cells that binds the costimulatory molecules B7-1 and B7-2 on antigen-presenting cells with a much higher affinity than CD28. Instead of transmitting a positive costimulatory signal to the T cell, ligation of CTLA-4 transmits a powerful inhibitory signal to T cells that can block T-cell activation. Indeed, CTLA-4 is one of the most powerful negative regulatory molecules on the cell surface of T cells.[56] Similarly, PD-1 is a receptor on T cells that binds PD-L1 or PD-L2 and recruits SHP phosphatases to impose a powerful inhibitory signal on T-cell activation and proliferation. Inhibiting the CTLA-4 and PD-1 pathways using CBI has demonstrated clinical activity in a variety of tumor types, including melanoma, lung cancer, renal cancer, bladder cancer, Hodgkin lymphoma, and prostate cancer.[57-66]
Chimeric Antigen Receptor T Cells
Significant progress and clinical responses have also been observed with adoptive T-cell transfer. Adoptive T-cell transfer bypasses the requirement for antigen presentation and development of an adaptive immune response, and instead, large numbers of effector T cells are generated ex vivo and are directly infused into the patient. This therapy has the capacity to eradicate malignant cells, although it is limited by the ability to isolate and expand endogenous antigen-specific antitumor T cells, such as from tumor infiltrating lymphocytes (TILs). One strategy for overcoming this limitation is to use chimeric antigen receptor (CAR) T cells. CAR T cells are engineered to express a specific antibody-binding domain connected to transmembrane and intracellular T-cell activation domains that function as an artificial T-cell receptor and allow for MHC-independent T-cell activation to a specified epitope. The activity of CAR therapy was demonstrated as a proof of principle for CD19-positive advanced chronic lymphocytic leukemia (CLL), in which the infused T cells expanded significantly in vivo and developed into CAR T cells with lasting memory.[67] Subsequent clinical trials have demonstrated activity in neuroblastoma, CLL, and B-cell lymphoma, with additional tumor types under investigation.[68] As a result of bypassing central tolerance and the requirement for MHC-mediated T-cell activation, one significant risk of CAR therapy is the potential for fatal unanticipated off-target side effects, which have been reported. Nevertheless, with clinically validated targets, CAR therapy represents a powerful tool in the immunotherapy armamentarium against cancer.
Much of the preclinical work combining radiation with CBI has been performed in animal models of melanoma, breast cancer, and colorectal cancer.[18,36,43-45,48] The initial work by Demaria and Formenti established key models for investigating abscopal effects-the effects of radiation outside of the field. Their pioneering studies used a bilateral flank model where one side was irradiated and the other flank was shielded, allowing for analysis of the systemic effects of radiation combined with CBI. Their studies clearly demonstrated that radiation can augment the systemic effects of CBI, and that the abscopal effect was immune-mediated. Recently, our work demonstrated that antigen-specific immune responses can be induced by stereotactic radiation alone or by radiation combined with CBI.[18] Using a knockout model, we also demonstrated that antigen cross-presentation may be required for the immune stimulatory effects of radiation.[18] This body of work in melanoma and other tumor types has been highlighted in a number of excellent reviews.[53,54,69] Below we discuss the preclinical and clinical data on additional and upcoming sites of investigation, namely glioma, lung cancer, and prostate cancer.
Radiation Combined With Checkpoint Blockade in Glioma
Glioblastoma (GBM) is one of the most common and highly aggressive forms of adult brain cancer. Life expectancy is very poor, with a median overall survival of 14.6 months and an approximate 75% mortality rate within the first 2 years; less than 10% of patients survive more than 5 years.[70] The current standard of care is maximum safe resection followed by adjuvant radiation combined with temozolomide, a treatment regimen founded on a randomized phase III trial testing radiation therapy vs radiation therapy plus temozolomide. In this study, the addition of temozolomide to adjuvant radiation improved survival by 2.5 months.[70] Of note, a companion study showed that patients with methylated O6-methylguanine-DNA methyltransferase (MGMT), a protein involved in DNA repair, derive a statistically significant benefit from adding temozolomide to radiation compared with patients with unmethylated MGMT, in whom there was less benefit from the use of temozolomide.[71]
Multiple immunotherapeutic approaches are under investigation for the treatment of GBM, including: anti–epidermal growth factor receptor variant III (EGFRvIII) CAR T cells that target the mutant EGFRvIII peptide, which is expressed in approximately one-third of GBM tumors (ClinicalTrials.gov identifier: NCT01454596); dendritic cell vaccines, DCVax-L (NCT00045968) and ICT-107 (NCT01280552), which use patient-specific tumor lysates and synthetic peptides respectively; the indoleamine 2,3-dioxygenase inhibitor indoximod, which is in a phase I/II trial (NCT02052648); and rindopepimut (CDX-110), a vaccine in phase III development that also targets EGFRvIII (NCT01480479). Importantly, CBI is also being studied in GBM, and below we summarize the preclinical and clinical studies using radiation and CBI in glioma.
Preclinical data in glioma
Zeng et al published the first study using the small animal radiation research platform (SARRP)-which allows for stereotactic radiation delivery-combined with anti–PD-1 immunotherapy.[46] In this study, the authors performed intracranial implantation of mouse glioma cell line GL261 to establish an orthotopic GBM model in order to investigate the effects of stereotactic radiosurgery combined with anti–PD-1 immunotherapy. Improved survival was observed in the group that received combined treatment, with a median survival of 25 days in the control arm, 27 days in the anti–PD-1 antibody arm, 28 days in the radiation arm, and 53 days in the radiation plus anti–PD-1 therapy arm (P < .05 by log-rank Mantle-Cox). Moreover, analysis on day 21 after implantation revealed increased cytotoxic T-cell tumor infiltration and decreased regulatory T cells in tumors of animals in the combined treatment group compared with control arms. These preclinical data provide ample rationale for clinical trials investigating radiation combined with anti–PD-1 immunotherapy for glioma.
Recently, Belcaid et al used a GBM model to investigate the effects of stereotactic radiation combined with a 4-1BB (CD137) agonist antibody and a CTLA-4–blocking antibody. The investigators first showed that stereotactic brain radiation combined with an anti–CTLA-4 antibody could prolong survival of mice with orthotopic GL261-luc gliomas. In an important sequencing experiment, the first dose of anti-CTLA-4 was given either prior to, during, or after radiation. Although the differences were not statistically significant, there appeared to be a trend towards concurrent radiation therapy plus CBI resulting in improved survival compared with initiation of CBI after completion of radiation. The authors then showed that by adding an agonist stimulatory antibody, approximately 50% of tumor-bearing mice exhibited long-term survival. Interestingly, they also showed that radiation and combined immunotherapy increased TIL populations, and that CD4 T cells appeared to be required for the improvement in survival, with CD8 T cells providing a modest benefit in this GBM model. These preclinical data provide an additional rationale for clinical trials combining stereotactic radiation with CBI, including anti–CTLA-4 antibodies, in glioma patients (Figure 1).
Clinical translation in GBM
Given the promising results of these preclinical studies, a phase I/II trial of anti–PD-1 therapy in relapsed GBM is currently underway (NCT01952769). In this study, pidilizumab (CT-011) will be administered to eligible patients at 6.0 mg/kg every other week until disease progression or a serious adverse event occurs. Additionally, a phase III randomized open-label trial of nivolumab vs bevacizumab and a safety study of nivolumab or nivolumab in combination with ipilimumab in adults with recurrent GBM is currently recruiting (NCT02017717). Clearly, additional combinatorial therapies are needed to help improve outcomes in this highly lethal disease.
Finally, there is now a phase II study of MEDI4736 (anti–PD-L1) combined with radiation in patients with GBM (NCT02336165). This multicenter study sponsored by the Ludwig Institute for Cancer Research aims to enroll over 80 patients with GBM into three cohorts. Cohort A will include patients with newly diagnosed unmethylated MGMT GBM who will receive MEDI4736 every 2 weeks in combination with standard radiation therapy; Cohort B will include bevacizumab-naive patients with recurrent GBM who will receive MEDI4736 every 2 weeks as monotherapy; and Cohort C will enroll bevacizumab-refractory patients with recurrent GBM who will receive MEDI4736 every 2 weeks in combination with continued bevacizumab. The primary endpoints include overall survival and progression-free survival. Secondary objectives include safety, tolerability, and biologic activity as assessed by immunologic markers. This study will investigate the efficacy of anti–PD-L1 monotherapy in GBM patients and radiation combined with anti–PD-L1 in patients with newly diagnosed GBM with unmethylated MGMT.
Radiation Combined with Immunotherapy in Lung Cancer
Lung cancer is the leading cause of cancer-related mortality in men and women. The majority of patients present after they become symptomatic and are diagnosed with advanced-stage disease. On February 2, 2015, the Centers for Medicare & Medicaid Services issued a final national coverage determination stating that Medicare would cover annual low-dose computed tomography (LDCT) screening for lung cancer in patients who meet the following criteria: age 55 to 77 years, either current smoker or have quit smoking within the last 15 years, and have a tobacco smoking history of at least 30 pack-years. This determination was based in part on the results of the National Lung Screening Trial, which reported a 20% relative reduction in lung cancer mortality with the use of LDCT screening compared with chest x-ray.[72] As with other national screening programs for cancer, there is the possibility for a relative increase in the percentage of lung cancer patients diagnosed with early-stage disease. The primary treatment for early-stage lung cancer is surgical resection, although definitive SBRT is the preferred treatment option for medically inoperable patients or those with poor performance status. Definitive SBRT for early-stage lung cancer has excellent local control rates that are similar to those of conventional surgery.[10] Thus, with the use of LDCT it is possible that SBRT will play an even more prominent role in lung cancer treatment in the future.
Systemic treatments for NSCLC have been advancing rapidly, with multiple different agents approved for specific molecular subtypes, including four targeted therapies approved since 2011. Although traditionally thought to be poorly immunogenic, lung cancer is now one of the most active areas of investigation for immunotherapy, especially CBI.[73] Nivolumab is now the first CBI approved to treat lung cancer and is also FDA-approved for advanced (metastatic) squamous NSCLC with progression on or after platinum-based chemotherapy. It is speculated that the high mutational burden induced by the carcinogens in smoke may result in numerous neo-antigens that the immune system can respond to once the tumor-mediated immunosuppression is blocked. A search identified at least 26 separate National Institutes of Health current clinical trials involving various CBI antibodies in some phase of investigation for the treatment of lung cancer. Interestingly, while radiation plays a key role in the management of lung cancer, very few of these studies incorporate radiation. Below we discuss the preclinical data and clinical trials of hypofractionated radiation combined with immunotherapy in lung cancer.
Preclinical data in lung cancer
Fotin-Mleczek et al recently published a study combining microRNA (mRNA)-based vaccination with radiation in the syngeneic Lewis lung cancer (LLC) model.[74] The authors reported that the combination of mRNA-based immunotherapy with radiation resulted in a strong synergistic antitumor effect.
Consistent with prior studies, they reported that radiation combined with immunotherapy induced a number of distinct changes in gene expression at the tumor site, including upregulation of genes involved in antigen presentation, and adhesion and immune cell infiltration, as well as activation of the innate immune system.[74] Analysis of LLC tumors after combined treatment with 12 Gy × 3 fractions demonstrated increases in immune cell infiltrates, including CD4- and CD8-positive T cells, CD8-positive dendritic cells, and natural killer T cells.[74] Given the multiple immune-stimulatory effects of radiation reported in this study, these results provide a mechanistic rationale for clinical trials combining radiation with immunotherapy in lung cancer.
Our group has shown that a combination of PD-L1 blockade and irradiation in an autochthonous model of NSCLC significantly improved local tumor response in the irradiated lung (A Walker, A Sharabi, C Drake, PT Tran, unpublished data). We also demonstrated evidence of partial tumor response in the unirradiated lung. An increase in T cells was observed in both irradiated and unirradiated lungs after radiation and checkpoint blockade, consistent with an abscopal effect (A Walker, A Sharabi, C Drake, PT Tran, unpublished data). These preclinical findings support clinical trials combining SBRT with CBI in patients with NSCLC (Figure 2).
Clinical translation in lung cancer
New York University has developed a phase II study for patients with metastatic NSCLC exploring the combination of radiation and ipilimumab, to test whether this combination can potentiate the immune system to produce an abscopal response (NCT02221739). Patients receive ipilimumab (3 mg/kg) within 24 hours of starting hypofractionated radiation therapy (6 Gy × 5 fractions). Ipilimumab dosing is repeated on days 22, 43, and 64. The primary goal is to evaluate the safety and therapeutic efficacy of anti–CTLA-4 monoclonal antibodies and concurrent local radiation therapy in NSCLC patients with metastatic disease. The secondary outcomes include the effects of radiation therapy and anti–CTLA-4 monoclonal antibodies on the development of antitumor immunity.
MD Anderson Cancer Center has also developed a phase I/II trial of ipilimumab and hypofractionated SBRT in patients with advanced solid malignancies (NCT02239900). The primary outcome of this study is the maximum tolerated dose of ipilimumab and SBRT. Secondary outcome measures include the effects of radiation therapy and anti–CTLA-4 on development of antitumor immunity. Patients will receive ipilimumab (3 mg/kg) combined with SBRT given at 50 Gy in 4 fractions. Importantly, the effect of timing and sequencing will also be investigated, with concurrent and sequential treatment groups. These clinical trials and others like them will help to determine whether the synergistic preclinical effects observed with radiation combined with CBI will translate into patients and improve clinical outcomes in lung cancer and patients with lung metastases.
Radiation Combined with Immunotherapy in Prostate Cancer
Prostate cancer is the most common cancer diagnosed in men in the United States and the second leading cause of cancer-related mortality. The vast majority of patients are diagnosed at early stages, when the disease is organ-confined. For those men who require therapy, the primary therapeutic treatment approaches are surgical resection or a course of radiation therapy with or without androgen deprivation therapy, depending on risk stratification. Although conventionally fractionated external beam radiation or brachytherapy are the standard radiation options, SBRT is under active study for definitive treatment of organ-confined prostate cancer. Long-term toxicity and outcomes data for prostate SBRT are being collected and are maturing.
The first FDA-approved autologous cell-based vaccine to treat any cancer was sipuleucel-T for the treatment of men with hormone-refractory metastatic prostate cancer. Sipuleucel-T is a dendritic cell vaccine generated from autologous peripheral blood mononuclear cells and is designed to induce an immune response against prostatic acid phosphatase. It was approved by the FDA in 2010 for the treatment of minimally symptomatic metastatic CRPC based on results of a randomized double-blind placebo-controlled phase III trial that showed an average survival improvement of 4.1 months, along with a very minimal side-effect profile.[75] Interestingly, recent follow-up data have identified that additional antigen-specific immune responses to epitopes not specifically targeted by the vaccine, including prostate-specific antigen (PSA) and LGALS3, can occur with sipuleucel-T and correlate with improved outcomes.[76] Numerous additional vaccines and combination immunotherapies are being investigated for metastatic CRPC, including: sipuleucel-T with enzalutamide (NCT01981122); sipuleucel-T and indoximod (NCT01560923); adoptive transfer of NY-ESO-1–specific T cells after chemotherapy (NCT01967823); PROSTVAC-VF vaccine and fowlpox vaccine (NCT01322490); and a neoadjuvant study of androgen ablation combined with cyclophosphamide and GVAX vaccine for localized prostate cancer (NCT01696877). Below we discuss some of the preclinical and clinical data combining radiation with immunotherapy in prostate cancer.
Preclinical data in prostate cancer
Harris et al initially studied the timing and sequencing of immunotherapy and radiation therapy in transgenic mice that develop spontaneous prostate cancer (TRAMP mice); they used an autochthonous model treated with a vaccinia-based tumor vaccine.[24] In this study, Pro-HA-TRAMP mice engineered to express the prostate-restricted hemagglutinin antigen (HA) were used to study the effects of a single high dose of radiation and a recombinant vaccinia-HA tumor vaccine on adoptive transfer of HA-specific CD4 T cells. In this study, our group reported that radiation combined with vaccine immunotherapy mitigated tumor-mediated T-cell tolerance, resulting in antitumor T-cell activation. Importantly, this effect was critically dependent on the timing of radiation therapy and immunotherapy, with antitumor immune responses observed when immunotherapy was administered 3 to 5 weeks post-radiotherapy, but not when immunotherapy was administered either prior to or later than 5 weeks post-radiotherapy. This study highlighted many important considerations for the sequencing and timing of radiation combined with immunotherapy for prostate cancer.
In a subsequent paper by Wada et al, the Pro-HA autochthonous TRAMP mouse model was used to study the effect of stereotactic radiation combined with a granulocyte-macrophage colony-stimulating factor–secreting cellular immunotherapy for prostate cancer (T-GVAX).[47] In this study, our group used the SARRP to deliver focused stereotactic radiation of 6 Gy × 2 fractions to the prostate. We reported that the combined therapy resulted in improved overall survival in a preventive metastasis model.[47] This same study used a micrometastasis model to show that combination therapy could mediate a modest but significant systemic antitumor immunity. It was also observed that combined therapy resulted in an increase of the ratio of effector-to-regulatory T cells for both CD4 and CD8 TILs. Similar data have subsequently been reported in numerous studies, demonstrating that radiation can enhance immune cell infiltration into tumors. These preclinical data provided ample rationale for subsequent clinical trials combining radiation with immunotherapy in prostate cancer.
Clinical translation in prostate cancer
Gully et al reported results of a randomized phase II clinical trial designed to determine whether a poxviral vaccine encoding PSA could induce PSA-specific T-cell responses when combined with radiation therapy in patients with clinically localized prostate cancer.[77] Thirty patients were randomly assigned to radiation alone vs radiation plus vaccine, with the latter group receiving “priming” vaccines with recombinant vaccinia PSA (rV-PSA) and recombinant vaccinia containing the costimulatory molecule B7.1 (rV-B7.1) followed by monthly booster vaccines with recombinant fowlpox PSA.
Standard external beam radiation therapy was given between the fourth and the sixth vaccinations. The authors reported evidence of de novo generation of T cells specific for prostate-associated antigens not present in the vaccine.[77] They argued that this epitope spreading was indirect evidence of immune-mediated tumor killing. The effects of radiation combined with a poxvirus-based vaccine encoding PSA were further analyzed by Nesslinger et al in patients with localized prostate cancer. In this study, pre- and post-treatment serum samples from a previously reported phase II clinical trial of patients treated with radiation combined with vaccine or patients treated with radiation alone were evaluated by Western blot and serologic screening. They reported that external beam radiation combined with vaccination against PSA resulted in epitope spreading and immune responses to additional tumor-associated antigens.[78]
A phase I/II study in patients with metastatic CRPC explored ipilimumab treatment alone or in combination with 8-Gy radiation given in a single fraction to metastatic lesions.[79] The study tested the hypothesis that ipilimumab would potentiate antitumor immunity following radiation by converting the tumor into an in situ vaccine via induction of immunogenic cell death and exposure of cryptic tumor antigens.[80] In the highest-dose group of 10 mg/kg, 8 of 50 patients exhibited a PSA decline of at least 50%, and 1 patient experienced a complete response, while 6 patients had stable disease. Kwon et al recently reported long-term follow-up of the large multi-institutional, prospective, phase III randomized trial of radiation combined with ipilimumab. This phase III study of men with metastatic CRPC was very close to meeting its primary endpoint of improved median overall survival (P = .053).[64] However, in a subset analysis there appeared to be clinically meaningful benefit in men without good performance status who did not have visceral metastases. A subsequent clinical trial is enrolling men without visceral metastases.[81]
Finally the ProstAtak trial is a national phase III placebo-controlled clinical trial incorporating a replication-defective adenovirus (AdV) combined with radiation in the definitive setting (NCT01436968). This trial employs an intraprostatic injection of AdV to deliver the herpesvirus thymidine kinase (HSV-tk) gene directly to prostate cancer cells. The oral antiherpetic drug valacyclovir is then administered as a prodrug that is phosphorylated by HSV-tk to form a cytotoxic nucleotide analog resulting in termination of DNA replication and, ultimately, cell death. AdV-tk is given concurrently with standard-of-care external beam radiation for intermediate- to high-risk prostate cancer. The primary outcome is disease-free survival in the ProstAtak arm vs the placebo control arm, and secondary endpoints concerned with immune responses are being collected. In part, this trial is supported by data from a study by Chhikara et al in which immunocompetent mice bearing the mouse prostate tumor RM-1 were treated with direct intratumoral injections of AdV-tk followed by ganciclovir and 5 Gy of radiation. These mice exhibited a significantly greater CD-4 infiltrate in tumors compared with mice treated with AdV-tk alone or radiation alone. Mice also received tail vein injection of RM-1 cells at the same time RM-1 xenografts were established. Xenografts were treated with AdV-tk, radiation, or a combination of both. Mice treated with a combination of AdV-tk and radiation exhibited a significantly reduced number of lung metastases compared with either unimodal therapy, suggesting that the combination therapy resulted in a systemic antitumor immune response.[82]
Conclusions and Future Directions
Ever-accumulating preclinical data have documented that immunotherapy can augment radiation-mediated local tumor response. Similarly, radiation can augment the systemic effects of immunotherapy.
Most preclinical data to date are from studies of high doses of radiation that, when translated to the clinic, may be best delivered with SBRT/stereotactic ablative radiotherapy. These data also support much of the ongoing clinical work, including demonstration that CBI has clinical activity in a wide variety of tumor types, as does adoptive T-cell transfer and certain cancer vaccines in tumors with known antigenic targets. One of the primary questions to answer is how best to incorporate immunotherapy into current definitive and palliative radiation treatment regimens. There is now an established body of literature demonstrating that radiation has the potential to enhance local and systemic antitumor immune responses and is thus an ideal modality to combine with immunotherapy. Additional questions remain regarding the optimal total dose, fraction size, field size, and scheduling for induction of immune responses. Thus, carefully designed studies will be required to investigate the effects of radiation combined with immunotherapy on local tumor control in the definitive setting and on systemic tumor control in the metastatic setting.
Financial Disclosure:Dr. Tran serves on the advisory boards of Astellas-Medivation and Regeneron, and he has received clinical trial funding from Astellas-Medivation. Dr. Drake has consulted for Amplimmune, Bristol-Myers Squibb (BMS), Merck, and Roche-Genentech, all of whom have either anti–PD-1 or anti–PD-L1 reagents in various stages of clinical development; in addition, Dr. Drake has received sponsored research funding from BMS. Dr. Lim has consulted for BMS and Accuray and has received research support from BMS, Accuray, Arbor Pharmaceuticals, Altor, Aegenus, and Immunocellular. Dr. DeWeese receives clinical trial support from Advantagene. Dr. Sharabi has no conflicts of interest to declare.
References:
1. Gunderson L, Tepper J. Clinical radiation oncology. Philadelphia, PA: Elsevier; 2012.
2. Leksell L. The stereotaxic method and radiosurgery of the brain. Acta Chir Scand. 1951;102:316-9.
3. Lozano AM. Textbook of Stereotactic and functional neurosurgery (v. 1 & 2). Springer; 2009.
4. Accuray. Cyberknife reimbursement information. 2001. Available from: http://www.cyberknife.com/reimbursement-insurance/index.aspx. Accessed April 17, 2015.
5. Timmerman RD, Herman J, Cho LC. Emergence of stereotactic body radiation therapy and its impact on current and future clinical practice. J Clin Oncol. 2014;32:2847-54.
6. Flickinger JC, Pollock BE, Kondziolka D, Lunsford LD. A dose-response analysis of arteriovenous malformation obliteration after radiosurgery. Int J Radiat Oncol Biol Phys. 1996;36:873-9.
7. Cheng JS, Sanchez-Mejia RO, Limbo M, et al. Management of medically refractory trigeminal neuralgia in patients with multiple sclerosis. Neurosurg Focus. 2005;18:e13.
8. Sheehan JP, Niranjan A, Sheehan JM, et al. Stereotactic radiosurgery for pituitary adenomas: an intermediate review of its safety, efficacy, and role in the neurosurgical treatment armamentarium. J Neurosurg. 2005;102:678-91.
9. Lutterbach J, Cyron D, Henne K, Ostertag CB. Radiosurgery followed by planned observation in patients with one to three brain metastases. Neurosurgery. 2003;52:1066-73; discussion 73-4.
10. Timmerman R, Paulus R, Galvin J, et al. Stereotactic body radiation therapy for inoperable early stage lung cancer. JAMA. 2010;303:1070-6.
11. Uh S, Lee SM, Kim HT, et al. The effect of radiation therapy on immune function in patients with squamous cell lung carcinoma. Chest. 1994;105:132-7.
12. Order SE. The effects of therapeutic irradiation on lymphocytes and immunity. Cancer. 1977;39:737-43.
13. Maehata Y, Onishi H, Kuriyama K, et al. Immune responses following stereotactic body radiotherapy for stage I primary lung cancer. Biomed Res Int. 2013;2013:731346.
14. Hauser SH, Calorini L, Wazer DE, Gattoni-Celli S. Radiation-enhanced expression of major histocompatibility complex class I antigen H-2Db in B16 melanoma cells. Cancer Res. 1993;53:1952-5.
15. Garnett CT, Palena C, Chakraborty M, et al. Sublethal irradiation of human tumor cells modulates phenotype resulting in enhanced killing by cytotoxic T lymphocytes. Cancer Res. 2004;64:7985-94.
16. Reits EA, Hodge JW, Herberts CA, et al. Radiation modulates the peptide repertoire, enhances MHC class I expression, and induces successful antitumor immunotherapy. J Exp Med. 2006;203:1259-71.
17. Wan S, Pestka S, Jubin RG, et al. Chemotherapeutics and radiation stimulate MHC class I expression through elevated interferon-beta signaling in breast cancer cells. PLoS One. 2012;7:e32542.
18. Sharabi AB, Nirschl CJ, Kochel CM, et al. Stereotactic radiation therapy augments antigen-specific PD-1 mediated anti-tumor immune responses via cross-presentation of tumor antigen. Cancer Immunol Res. 2015;3:345-55
19. Verbrugge I, Gasparini A, Haynes NM, et al. The curative outcome of radioimmunotherapy in a mouse breast cancer model relies on mTOR signaling. Radiat Res. 2014;182:219-29.
20. Gameiro SR, Jammeh ML, Wattenberg MM, et al. Radiation-induced immunogenic modulation of tumor enhances antigen processing and calreticulin exposure, resulting in enhanced T-cell killing. Oncotarget. 2014;5:403-16.
21. Rovere-Querini P, Capobianco A, Scaffidi P, et al. HMGB1 is an endogenous immune adjuvant released by necrotic cells. EMBO Rep. 2004;5:825-30.
22. Andersson U, Erlandsson-Harris H, Yang H, Tracey KJ. HMGB1 as a DNA-binding cytokine. J Leukoc Biol. 2002;72:1084-91.
23. Lugade AA, Moran JP, Gerber SA, et al. Local radiation therapy of B16 melanoma tumors increases the generation of tumor antigen-specific effector cells that traffic to the tumor. J Immunol. 2005;174:7516-23.
24. Harris TJ, Hipkiss EL, Borzillary S, et al. Radiotherapy augments the immune response to prostate cancer in a time-dependent manner. Prostate. 2008;68:1319-29.
25. Takeshima T, Chamoto K, Wakita D, et al. Local radiation therapy inhibits tumor growth through the generation of tumor-specific CTL: its potentiation by combination with Th1 cell therapy. Cancer Res. 2010;70:2697-706.
26. Parker JJ, Jones JC, Strober S, Knox SJ. Characterization of direct radiation-induced immune function and molecular signaling changes in an antigen-presenting cell line. Clin Immunol. 2013;148:44-55.
27. Gupta A, Probst HC, Vuong V, et al. Radiotherapy promotes tumor-specific effector CD8+ T cells via dendritic cell activation. J Immunol. 2012;189:558-66.
28. Bernstein MB, Garnett CT, Zhang H, et al. Radiation-induced modulation of costimulatory and coinhibitory T-cell signaling molecules on human prostate carcinoma cells promotes productive antitumor immune interactions. Cancer Biother Radiopharm. 2014;29:153-61.
29. Ishihara H, Tsuneoka K, Dimchev AB, Shikita M. Induction of the expression of the interleukin-1 beta gene in mouse spleen by ionizing radiation. Radiat Res. 1993;133:321-6.
30. Hallahan DE, Spriggs DR, Beckett MA, et al. Increased tumor necrosis factor alpha mRNA after cellular exposure to ionizing radiation. Proc Natl Acad Sci USA. 1989;86:10104-7.
31. Hong JH, Chiang CS, Tsao CY, et al. Rapid induction of cytokine gene expression in the lung after single and fractionated doses of radiation. Int J Radiat Biol. 1999;75:1421-7.
32. Drake CG. Radiation-induced immune modulation. Springer New York; 2011.
33. Matsumura S, Demaria S. Up-regulation of the pro-inflammatory chemokine CXCL16 is a common response of tumor cells to ionizing radiation. Radiat Res. 2010;173:418-25.
34. Burnette BC, Liang H, Lee Y, et al. The efficacy of radiotherapy relies upon induction of type I interferon-dependent innate and adaptive immunity. Cancer Res. 2011;71:2488-96.
35. Gerber SA, Sedlacek AL, Cron KR, et al. IFN-gamma mediates the antitumor effects of radiation therapy in a murine colon tumor. Am J Pathol. 2013;182:2345-54.
36. Dovedi SJ, Adlard AL, Lipowska-Bhalla G, et al. Acquired resistance to fractionated radiotherapy can be overcome by concurrent PD-L1 blockade. Cancer Res. 2014;74:5458-68.
37. Chakraborty M, Abrams SI, Camphausen K, et al. Irradiation of tumor cells up-regulates Fas and enhances CTL lytic activity and CTL adoptive immunotherapy. J Immunol. 2003;170:6338-47.
38. Stone HB, Peters LJ, Milas L. Effect of host immune capability on radiocurability and subsequent transplantability of a murine fibrosarcoma. J Natl Cancer Inst. 1979;63:1229-35.
39. Lee Y, Auh SL, Wang Y, et al. Therapeutic effects of ablative radiation on local tumor require CD8+ T cells: changing strategies for cancer treatment. Blood. 2009;114:589-95.
40. Yoshimoto Y, Suzuki Y, Mimura K, et al. Radiotherapy-induced anti-tumor immunity contributes to the therapeutic efficacy of irradiation and can be augmented by CTLA-4 blockade in a mouse model. PLoS One. 2014;9:e92572.
41. Chakravarty PK, Alfieri A, Thomas EK, et al. Flt3-ligand administration after radiation therapy prolongs survival in a murine model of metastatic lung cancer. Cancer Res. 1999;59:6028-32.
42. Cao ZA, Daniel D, Hanahan D. Sub-lethal radiation enhances anti-tumor immunotherapy in a transgenic mouse model of pancreatic cancer. BMC Cancer. 2002;2:11.
43. Demaria S, Ng B, Devitt ML, et al. Ionizing radiation inhibition of distant untreated tumors (abscopal effect) is immune mediated. Int J Radiat Oncol Biol Phys. 2004;58:862-70.
44. Demaria S, Kawashima N, Yang AM, et al. Immune-mediated inhibition of metastases after treatment with local radiation and CTLA-4 blockade in a mouse model of breast cancer. Clin Cancer Res. 2005;11:728-34.
45. Dewan MZ, Galloway AE, Kawashima N, et al. Fractionated but not single-dose radiotherapy induces an immune-mediated abscopal effect when combined with anti-CTLA-4 antibody. Clin Cancer Res. 2009;15:5379-88.
46. Zeng J, See AP, Phallen J, et al. Anti-PD-1 blockade and stereotactic radiation produce long-term survival in mice with intracranial gliomas. Int J Radiat Oncol Biol Phys. 2013;86:343-9.
47. Wada S, Harris TJ, Tryggestad E, et al. Combined treatment effects of radiation and immunotherapy: studies in an autochthonous prostate cancer model. Int J Radiat Oncol Biol Phys. 2013;87:769-76.
48. Deng L, Liang H, Burnette B, et al. Irradiation and anti-PD-L1 treatment synergistically promote antitumor immunity in mice. J Clin Invest. 2014;124:687-95.
49. Belcaid Z, Phallen JA, Zeng J, et al. Focal radiation therapy combined with 4-1BB activation and CTLA-4 blockade yields long-term survival and a protective antigen-specific memory response in a murine glioma model. PLoS One. 2014;9:e101764.
50. Friedman EJ. Immune modulation by ionizing radiation and its implications for cancer immunotherapy. Curr Pharm Des. 2002;8:1765-80.
51. Formenti SC, Demaria S. Combining radiotherapy and cancer immunotherapy: a paradigm shift. J Natl Cancer Inst. 2013;105:256-65.
52. Zeng J, Harris TJ, Lim M, et al. Immune modulation and stereotactic radiation: improving local and abscopal responses. Biomed Res Int. 2013;2013:658126.
53. Demaria S, Pilones KA, Vanpouille-Box C, et al. The optimal partnership of radiation and immunotherapy: from preclinical studies to clinical translation. Radiat Res. 2014;182:170-81.
54. Zamarin D, Postow MA. Immune checkpoint modulation: rational design of combination strategies. Pharmacol Ther. 2015;150:28-32.
55. Couzin-Frankel J. Breakthrough of the year 2013. Cancer immunotherapy. Science. 2013;342:1432-3.
56. Scalapino KJ, Daikh DI. CTLA-4: a key regulatory point in the control of autoimmune disease. Immunol Rev. 2008;223:143-55.
57. Hodi FS, O’Day SJ, McDermott DF, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 2010;363:711-23.
58. Robert C, Thomas L, Bondarenko I, et al. Ipilimumab plus dacarbazine for previously untreated metastatic melanoma. N Engl J Med. 2011;364:2517-26.
59. Topalian SL, Hodi FS, Brahmer JR, et al. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med. 2012;366:2443-54.
60. McDermott DF, Drake CG, Sznol M, et al. Survival, Durable response, and long-term safety in patients with previously treated advanced renal cell carcinoma receiving nivolumab. J Clin Oncol. 2015 Mar 30. [Epub ahead of print]
61. Hamid O, Robert C, Daud A, et al. Safety and tumor responses with lambrolizumab (anti-PD-1) in melanoma. N Engl J Med. 2013;369:134-44.
62. Wolchok JD, Kluger H, Callahan MK, et al. Nivolumab plus ipilimumab in advanced melanoma. N Engl J Med. 2013;369:122-33.
63. Topalian SL, Sznol M, McDermott DF, et al. Survival, durable tumor remission, and long-term safety in patients with advanced melanoma receiving nivolumab. J Clin Oncol. 2014;32:1020-30.
64. Kwon ED, Drake CG, Scher HI, et al. Ipilimumab versus placebo after radiotherapy in patients with metastatic castration-resistant prostate cancer that had progressed after docetaxel chemotherapy (CA184-043): a multicentre, randomised, double-blind, phase 3 trial. Lancet Oncol. 2014;15:700-12.
65. Powles T, Eder JP, Fine GD, et al. MPDL3280A (anti-PD-L1) treatment leads to clinical activity in metastatic bladder cancer. Nature. 2014;515:558-62.
66. Ansell SM, Lesokhin AM, Borrello I, et al. PD-1 blockade with nivolumab in relapsed or refractory Hodgkin’s lymphoma. N Engl J Med. 2015;372:311-9.
67. Kalos M, Levine BL, Porter DL, et al. T cells with chimeric antigen receptors have potent antitumor effects and can establish memory in patients with advanced leukemia. Sci Transl Med. 2011;3:95ra73.
68. Barrett DM, Singh N, Porter DL, et al. Chimeric antigen receptor therapy for cancer. Annu Rev Med. 2014;65:333-47.
69. Tang C, Wang X, Soh H, et al. Combining radiation and immunotherapy: a new systemic therapy for solid tumors? Cancer Immunol Res. 2014;2:831-8.
70. Stupp R, Mason WP, van den Bent MJ, et al. Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med. 2005;352:987-96.
71. Hegi ME, Diserens AC, Gorlia T, et al. MGMT gene silencing and benefit from temozolomide in glioblastoma. N Engl J Med. 2005;352:997-1003.
72. National Lung Screening Trial Research Team, Aberle DR, Adams AM, et al. Reduced lung-cancer mortality with low-dose computed tomographic screening. N Engl J Med. 2011;365:395-409.
73. Brahmer JR, Pardoll DM. Immune checkpoint inhibitors: making immunotherapy a reality for the treatment of lung cancer. Cancer Immunol Res. 2013;1:85-91.
74. Fotin-Mleczek M, Zanzinger K, Heidenreich R, et al. mRNA-based vaccines synergize with radiation therapy to eradicate established tumors. Radiat Oncol. 2014;9:180.
75. Kantoff PW, Higano CS, Shore ND, et al. Sipuleucel-T immunotherapy for castration-resistant prostate cancer. N Engl J Med. 2010;363:411-22.
76. GuhaThakurta D, Sheikh NA, Fan LQ, et al. Humoral immune response against non-targeted tumor antigens after treatment with sipuleucel-T and its association with improved clinical outcome. Clin Cancer Res. 2015 Feb 3. [Epub ahead of print]
77. Gulley JL, Arlen PM, Bastian A, et al. Combining a recombinant cancer vaccine with standard definitive radiotherapy in patients with localized prostate cancer. Clin Cancer Res. 2005;11:3353-62.
78. Nesslinger NJ, Ng A, Tsang KY, et al. A viral vaccine encoding prostate-specific antigen induces antigen spreading to a common set of self-proteins in prostate cancer patients. Clin Cancer Res. 2010;16:4046-56.
79. Slovin SF, Higano CS, Hamid O, et al. Ipilimumab alone or in combination with radiotherapy in metastatic castration-resistant prostate cancer: results from an open-label, multicenter phase I/II study. Ann Oncol. 2013;24:1813-21.
80. Golden EB, Frances D, Pellicciotta I, et al. Radiation fosters dose-dependent and chemotherapy-induced immunogenic cell death. Oncoimmunology. 2014;3:e28518.
81. Drake CG. Visceral metastases and prostate cancer treatment: ‘die hard,’ ‘tough neighborhoods,’ or ‘evil humors’? Oncology (Williston Park). 2014;28: 974-80
82. Chhikara M, Huang H, Vlachaki MT, et al. Enhanced therapeutic effect of HSV-tk+GCV gene therapy and ionizing radiation for prostate cancer. Mol Ther. 2001;3:536-42.