Systemic Monotherapy vs Combination Therapy for CTCL: Rationale and Future Strategies
There are few approved therapies for cutaneous T-cell lymphoma (CTCL). The retinoids are the major biologic response modifiers used in CTCL, producing good response rates but few complete responses. For patients with early-stage disease, the oral retinoids can be combined with other therapies, such as psoralen plus ultraviolet A or interferon α, to improve response rates. Combined-modality therapy with oral retinoids, combined chemotherapy, electron-beam therapy, and topical mustargen has also proved effective. For the treatment of advanced-stage disease, the targeted therapy denileukin diftitox (Ontak) provides a nonimmunosuppressive alternative to conventional chemotherapy or radiation therapy. Of the conventional chemotherapies that have been tested in CTCL, gemcitabine (Gemzar) has demonstrated good efficacy in producing responses, particularly in patients with tumors. This agent can be used in combination with a maintenance therapy of bexarotene (Targretin) to manage the plaques and patches of mycosis fungoides. Several other targeted therapies are now also in testing, for example, alemtuzumab (CamPath), HuMax-CD4, several histone deacetylase inhibitors, and the transition-state inhibitor forodesine. These drugs, in combination with currently used therapies, may increase the number and combinations of therapies available for the treatment of this chronic condition to optimize long-lasting responses in CTCL.
There are few approved therapies for cutaneous T-cell lymphoma (CTCL). The retinoids are the major biologic response modifiers used in CTCL, producing good response rates but few complete responses. For patients with early-stage disease, the oral retinoids can be combined with other therapies, such as psoralen plus ultraviolet A or interferon α, to improve response rates. Combined-modality therapy with oral retinoids, combined chemotherapy, electron-beam therapy, and topical mustargen has also proved effective. For the treatment of advanced-stage disease, the targeted therapy denileukin diftitox (Ontak) provides a nonimmunosuppressive alternative to conventional chemotherapy or radiation therapy. Of the conventional chemotherapies that have been tested in CTCL, gemcitabine (Gemzar) has demonstrated good efficacy in producing responses, particularly in patients with tumors. This agent can be used in combination with a maintenance therapy of bexarotene (Targretin) to manage the plaques and patches of mycosis fungoides. Several other targeted therapies are now also in testing, for example, alemtuzumab (CamPath), HuMax-CD4, several histone deacetylase inhibitors, and the transition-state inhibitor forodesine. These drugs, in combination with currently used therapies, may increase the number and combinations of therapies available for the treatment of this chronic condition to optimize long-lasting responses in CTCL.
Only a limited number of therapies are approved for cutaneous T-cell lymphoma (CTCL), the most common disorders of which are mycosis fungoides (MF) and Sézary syndrome (SS). The most recently approved therapies for CTCL are vorinostat (Zolinza), a histone deacetylase inhibitor (in 2006); denileukin diftitox (Ontak), an interleukin (IL)-2 fusion protein (in 1999); and bexarotene (Targretin), the first retinoid-X receptor (RXR)-selective retinoid (in 1999). Treatment strategies in the management of MF are aimed at removal of the persistent antigen stimulus, reversal of the shift from Th2 to Th1 cytokine expression, induction of an increase in CD8+ cells, avoidance of immunosuppression, and prophylaxis or treatment of associated infectious complications.
A number of treatment options are available for different disease stages of MF.[1] Patients in early disease stages are prescribed skin-directed topical therapies, including steroids, bexarotene gel or topical mustargen, or phototherapy. For intermediate stages such as extensive plaques, biologic response modifiers (such as oral bexarotene, interferons [IFNs], and denileukin diftitox) are available and increase the immune response. In patients with tumors or nodal disease, single-agent nucleoside analogs (such as gemcitabine [Gemzar] and pentostatin [Nipent]),[2,3] combination chemotherapy, or targeted therapy (with fusion toxins, antibodies, and small molecules) is used. If patients at late stages can produce a good partial response, allogeneic bone marrow transplant (BMT) may offer the possibility of complete remission. However, it is possible that efficacy of treatment could be increased by combining these agents.
The question of whether to use a series of single conservative therapies or intensive early combination therapy was first addressed in a clinical trial in the 1980s. Sequential conservative therapy produced the same overall survival rates as intensive combination chemotherapy, and there were early deaths in the latter arm.[4] However, this study is out of date and should be repeated using some of the newer agents available. How best to integrate the new agents with existing therapies will require additional well-designed, randomized trials. Our goal should be to produce rational combinations of drugs that can either induce a cure or prolonged complete response in patients. But how can such combinations be identified without conducting a huge number of clinical trials to test the many possible combinations? The aim of this manuscript is to look at some of the evidence available on a number of combination therapies, based on published data and on the author's experience in the clinical management of CTCL, with a particular focus on advanced, progressive refractory MF.
Retinoids or Rexinoid Therapy
Retinoids are the major biologic response modifiers that have been used in CTCL since the 1980s.[5-11] Retinoic acid receptor (RAR) agonists (isotretinoin, etretinate [Tegison]) have been demonstrated to produce an overall response rate of about 58%, but the complete response rate is low, at about 19% for the RAR retinoids.[9,12-15] Furthermore, these drugs are more effective in patients with early disease than in those with advanced CTCL. However, combination with psoralen plus ultraviolet A (PUVA) or IFN increases overall response rates to about 70%,[15] as discussed elsewhere in this supplement.
Several oral retinoids are currently available: isotretinoin, acetretin (Soriatane), bexarotene, and all trans-retinoic acids. Many more are in development, each showing different selectivity for the retinoid receptors. If clear evidence was available to identify which retinoid receptors are key for putting CTCL in remission, it is possible that these selective retinoids could be combined in a rational manner to improve their effectiveness. Bexarotene, for example, is a retinoid that is selective for the RXR (described as a rexinoid), and is highly active in CTCL for both early[16] and advanced disease[17] and as a topical formulation.[18] At high concentrations, this drug also has RAR activity, which may possibly be important for its efficacy, as the response rates showed a dose response.
Bexarotene has been shown to induce T-cell modulation and to increase the number of circulating CD8+ T cells among responders. Among 33 patients with MF and 4 with other lymphomas, 32 had high CD4:CD8 ratios at baseline.[19] Following treatment with bexarotene at 150-300 mg/m2/d for 13 months (range: 4-18 months), a total of 26 patients showed normalization of CD8+ cell counts after 6.5 weeks (range: 3.5-12 weeks). The patients who responded to bexarotene therapy had higher numbers of CD8+ cells than those who did not (975 vs 221/mm3; P = .002) and lower CD4:CD8 ratios (0.8 vs 2.5; P = .005). In addition, a subsequent reduction in CD8+ cell count was associated with relapse. As an increase in CD8+ cells is a desirable outcome in the treatment of CTCL, this provides a rationale for the use of bexarotene in combination with a number of other agents.
Optimizing Therapy by Combination
In an effort to improve treatment efficacy and outcome with retinoids in CTCL, a combined-modality protocol was initiated in 1987 at the M.D. Anderson Cancer Center for patients with advanced, refractory MF, and was updated.[17,20,21] This was a multiphase therapy, beginning with treatment for 4 months with the retinoid oral isotretinoin at 1 mg/kg/d and IFNα at 3-5 MIU three times weekly (tiw). Patients with late-stage (IIB-IVB) disease were then given combined chemotherapy consisting of methotrexate, etoposide, and dexa-methasone for six courses over 6 months. They subsequently underwent electron-beam therapy (3,600 Gy) before entering a maintenance phase in which they received topical mustargen ointment as well as subcutaneous IFNα at 3-5 MIU tiw, for 1 to 2 years, as tolerated until relapse.[21] A total of 91 patients were treated with the combined-modality therapy.
When outcomes were last assessed in 2003, 57 were still alive (62%), there were 24 deaths (26.4%), mostly in the patients at later disease stages, and 11 patients were lost to follow-up.[21] The overall complete response rate was 57%, with a median duration of response of 20.8 months.[21] Patients at all stages showed treatment responses, even patients with stage IVB disease achieved complete remissions. Furthermore, some patients at early disease stages have ongoing complete responses at ≥ 10 years.
This multiphase, combined-modality therapy is capable of achieving good response rates and even complete responses. It is generally well tolerated. The first regimen now includes bexarotene rather than isotretinoin in patients who do not have intrinsic hypertriglyceridemia. In addition, younger patients at later disease stages who are able to achieve a near-complete response following electron-beam therapy are now offered the option of allogeneic BMT, if there is a matched (preferably related) bone marrow or peripheral stem cell donor available. Patients who fail to reach complete response are treated either with experimental agents or a nucleoside analog such as gemcitabine for tumor stage [22] or deoxycoformycin for SS.[3] Relapsed patients with advanced disease have also shown excellent responses to a combination of reduced doses of gemcitabine, liposomal doxorubicin (Doxil) and bortezomib (Velcade) in an ongoing phase I trial, although myelosuppression and infection are possible side effects.
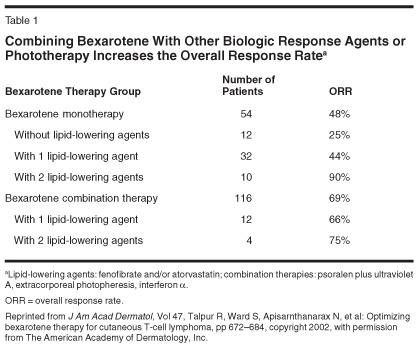
Combining bexarotene with other biologic response agents or with phototherapy has been shown to increase its efficacy. Thus, in a study of bexarotene in 70 patients with CTCL at our center, 54 received bexarotene monotherapy and showed a response rate of 48%. Tightly controlling hyperlipidemia by adding the lipid-lowering agents fenofibrate and atorvastatin (Lipitor) to the treatment regimen was shown to increase the response rate to 70%, and four patients experienced complete responses lasting longer than 4 years. A total of 16 patients received combination therapy of bexarotene with photopheresis, IFNα, or PUVA, producing an overall response rate of 69% (Table 1).[23]
Bexarotene binds to the RXR receptor; thus its efficacy might be enhanced by the addition of vitamin D, peroxisome proliferator-activated receptor (PPAR) agonists, or retinoids specific for the RAR. We have shown that bexarotene will induce T-cell apoptosis in vitro as a single agent [24] and demonstrated increased activity when bexarotene is combined with 2-cyano-3,12-dioxoolean-1,9-dien-28-oic acid (CDDO), a PPAR agonist.[25] Another possible combined therapy would be with agents such as the histone deacetylase (HDAC) inhibitors that change levels of transcription factors including retinoid receptors at the level of the promoter.[26]
An obvious combination of oral bexarotene with IFNα 2b was tested in a phase II, single-arm, multicentre study. A total of 22 patients with MF stages IB to IV were enrolled. Most of them had advanced disease, and all but one had failed prior therapy.[27] Therapy was initiated with bexarotene at a dose of 300 mg/m2 for 8 weeks. Three patients showed a complete response to this therapy and were not given IFN. In those who did not show a complete response, IFNα 2b at 3 to 5 MIU tiw was added for another 8 weeks. From the 17 of the 22 patients who completed the trial, 6/17 had partial responses and 1 had a complete response, giving an overall response rate of 41%. The mean duration of response in these advanced-stage patients, however, was low at 2.7 months (range: 1-7.6 months).
On this combination of full doses of IFN and bexarotene, the side effects were more prevalent and the response rate was not different from that for either drug alone. Grade 3 or 4 toxicities recorded were high cholesterol and triglyceridemia in five patients, neutropenia in three, lymphopenia in two, and elevated aspartate aminotransferase in two; therefore, the trial was stopped early. A combination of lower doses of both IFN and bexarotene with photopheresis is widely used and effective in the treatment of patients with SS who have remaining CD8+ cells, and excellent response rates have been reported (see discussion below).
Treatment of Advanced Tumors and Nodal Lymphoma
Denileukin Diftitox
For patients with advanced tumors and nodal lymphoma, the treatment choice is generally between radiation therapy (for cutaneous tumors) and single- or multiagent chemotherapy. A nonimmunosuppressive and effective alternative to conventional chemotherapy is now provided by denileukin diftitox.
Denileukin diftitox is a recombinant fusion protein composed of the receptor-binding domain of IL-2 conjugated to diphtheria toxin. Denileukin diftitox must bind to the high- or intermediate-affinity IL-2 receptors to be internalized into the cell effectively.[28] The drug is given by rapid intravenous infusion, with the maximum tolerated dose found to be 23 µg/kg. It has a serum half-life of 70 to 80 minutes, but this is reduced by the production of antibodies in subsequent courses.
In CTCL cell lines, the response and sensitivity to denileukin diftitox is related to the level of expression of the high-affinity IL-2 receptor, but whether this holds true in patients is not yet known.[29] As the α chain of the IL-2 receptor (CD25) is not expressed in the intermediate receptors, which are also capable of binding and internalizing denileukin diftitox, CD25 staining may not be the best marker for predicting clinical response. However, we found that patients whose lesional lymphocytes had more than 20% CD25 expression had an 80% response rate to denileukin diftitox compared with a 20% response rate in patients whose biopsies showed CD25 expression on immunohistochemistry staining of less than 20% of the lymphocytes.[30] A large multicenter trial treating patients irrespective of CD25 expression should help to answer whether or not efficacy in patients is correlated to the level of CD25 expression.
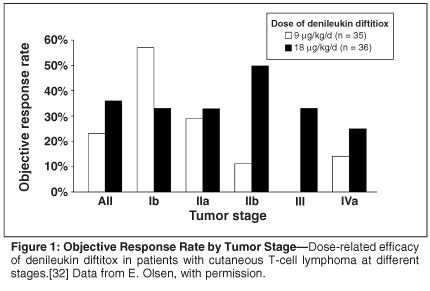
The initial proof-of-concept study of denileukin diftitox in patients with CTCL reported complete responses in 14% and partial responses in 20%, giving a 34% overall response rate.[31] In the subsequent pivotal trial of patients who had failed more than three therapies, the difference in the rates of best response for the two dose groups (9 and 18 µg/kg/d) was not significant. There was, however, a trend suggesting a dose effect in patients with more advanced disease; there was a 38% response rate with 18 µg/kg/day vs a 10% response rate for the lower dose (Figure 1).[32] The reason for this difference may relate to the greater tumor burden in patients with tumors and nodal disease. In the pivotal trial, the overall response was 30%, including 10% complete responses. The median duration of response in the pivotal study was 6.9 months; however, some durable long-term responses were also seen. Thus, patients may experience complete responses with denileukin diftitox, and even partial responses are associated with improved quality of life.[33] This drug may be superior to chemotherapy in debulking tumor disease in MF[34] and other forms of peripheral lymphoma.[35] Denileukin diftitox is safer than chemotherapy because there is no neutropenia and the rate of infection is lower.
As no premedication was allowed in the study, acute infusion reactions were seen in approximately 70% of patients receiving treatment with this agent in the pivotal trial. They include fever, chills, urticaria, nausea, chest pain, and rarely, anaphylaxis. Acute infusion reactions can be prevented by the coadministration of low-dose steroids prior to each therapy. This practice of combining steroids with denileukin diftitox has increased the response rates to > 60%, some of which may be related to the cortico-steroids or to increased tolerance to the drug in patients.[36] In some patients with erythroderma, systemic steroids may lead to rebound flare when they are tapered.
The major undesirable side effect of denileukin diftitox is the capillary-leak syndrome (CLS), which was experienced by 27% of patients during the pivotal trial. In our experience, patients with CLS most often respond to therapy, which may indicate that cells found around blood vessels are being killed. It is rare to experience CLS more than once. The severity and incidence of CLS following denileukin diftitox may be prevented by giving 500 to 1,000 mL of saline after the infusion, which flushes the drug quickly through the kidneys.[36] Other adverse events that occur not infrequently include transaminase elevations with nausea and acute thyroiditis in about 10% of patients that can be confused with an acute infusion reaction if there is transient thyrotoxicosis.[37] There is a learning curve to using denileukin diftitox effectively, and many patients on the clinical trial dropped out early due to side effects that are now easily prevented or managed conservatively.
Other combinations with denileukin diftitox need to be explored, in particular, a phase I trial combining escalating doses of oral bexarotene given prior to initiating treatment with denileukin diftitox. There was an increase in the expression of CD25 on lymphocytes, as determined by flow cytometry, following treatment even with low doses of bexarotene (at least 150 mg/d). Thus, there may be some synergism between these two drugs.[38] Clinically, we have found that treating tumors with denileukin diftitox can be followed by oral bexarotene maintenance with the addition of skin-directed therapies as needed to achieve near-complete and durable responses in patients with advanced, difficult-to-treat disease.[39]
Chemotherapy: Alone or in Combination
Single-agent chemotherapies (such as methotrexate, nitrogen mustard, cyclophosphamide, carmustine [BiCNU], bleomycin, doxorubicin, cisplatin, etoposide, and gemcitabine) are widely used for MF and other forms of CTCL. Their response rates as single agents are high (about 60%) for most, but the median duration of response is very low at less than 6 months. Thus when using these therapies, a maintenance treatment should also be considered. If a patient shows a good response to a single agent, it would then be appropriate to add bexarotene, for example, to the treatment regimen, to try to maintain the response. However, further evidence is needed on how we can best combine these chemotherapies with other drugs to improve the complete response rate.
Of the nucleoside analogs, gemcitabine has started to be widely used in CTCL. Fludarabine (Fludara) is considerably less active than gemcitabine (response rate 19%),[40] and may produce immunosuppression. In one clinical trial Ara-G was associated with neurotoxicity and the trial was discontinued. Deoxycoformycin is highly active in patients with Sézary syndrome, and produces response rates of 60% for this indication;[3] however, this drug is not effective in treating tumors and does not produce durable responses.[3]
Gemcitabine has been approved for pancreatic and lung cancer in the United States. A European phase II study of this agent in CTCL reported an 11% complete response and a 70% overall response rate.[41] These results were confirmed in a subsequent study of 25 patients with highly refractory CTCL who were given gemcitabine at 1,000 mg/m2 three times per month, with a similar overall response rate of 68%.[22] Patients with tumors responded very well (7/8 patients responded), but complete responses were seen only rarely. Another European study tested gemcitabine at the higher dose of 1,200 mg/m2 three times in a month for 6 months. In 32 untreated patients, there were 7 complete responses (rate of 22%), with a median duration of 10 months and a partial response rate of 53%.[42] Although there are side effects associated with this treatment, these are tolerable; patients do not suffer alopecia and myelosuppression is mild.
The obvious agent for combination with gemcitabine is bexarotene. While gemcitabine is highly effective against tumors, bexarotene will clear patches and plaques of MF. In the author's experience, it is possible to use a combination of low-dose bexarotene and low-dose gemcitabine in elderly patients for whom chemotherapy would be dangerous or ill-advised. Lower doses of gemcitabine (500 to 750 mg/m2) given by infusion twice a month as long as tumors persist and bexarotene at 150 to 300 mg/m2 have maintained patients for more than 1 year. Bexarotene is given continuously, whereas gemcitabine is infused only when required to treat new tumors. The patients have been well, treated at home, with no infections and no need for intravenous lines. We find the treatment to be well tolerated and it seems to be a safe alternative to combined chemotherapy in elderly patients. Patients may experience mild myelosuppression and anemia, but no nausea, vomiting, or alopecia. Stem-cell factor support is rarely needed.
Another active single agent is liposomal doxorubicin, which is stable, long-acting, and has low toxicity. In a prospective pilot study of six patients with refractory MF, the extremely high response rate of 83% was obtained, with four complete responses.[43] Doxorubicin is highly effective, but it is associated with dose-dependent cardiomyopathy in the long term, and with some myelosuppression, nausea, and vomiting. Doxorubicin also causes painful palmar-plantar dysesthesia. We are therefore investigating lower doses of a combination of liposomal doxorubicin, gemcitabine, and the proteosome inhibitor bortezomib in a phase I combination trial in all patients with cancer. The five patients with MF enrolled in this trial so far have shown excellent responses, but some have also become neutropenic. A second trial will combine induction with doxorubicin and bexarotene maintenance therapy.
Currently, the preferred approach to the management of tumor-stage disease is to treat with denileukin diftitox to debulk the tumors, rather than use chemotherapy. This is followed by maintenance therapy with bexarotene or IFN and, if required, skin-directed therapy (PUVA). Additional topical therapy with bexarotene gel may also be used. An example of this combination was recently published as a case report on a woman maintained for 5 years.[44]
HDAC inhibitors also show activity in MF and other forms of CTCL. Several different agents in clinical trials including oral vorinostat and intravenous depsipeptide have shown activity even in patients with advanced disease. These agents also have the potential to be combined with retinoids such as bexarotene to increase the response rate without producing overlapping toxicities.
Sézary Syndrome
Photopheresis has been used to treat SS since 1987, giving complete response rates of 15% and overall response rates of 50%. A combination of photopheresis with other agents can increase those response rates to 70%.[45] As erythroderma is associated with Staphylococcus colonization, our initial treatment regimen for patients with SS consists of oral dicloxicillin daily, nasal and topical mupirocin and skin care meant to eradicate S aureus colonization. Photopheresis is administered every 2-4 weeks, with the frequency being reduced if patients show a response. Low-dose IFNα (3 million units subcutaneously 3 to 7 times per week) and low-dose bexarotene (150-225 mg) are subsequently added to the treatment regimen, and granulocyte-macrophage colony-stimulating factor is added after each photopheresis if patients are not responding or if they have a low white blood cell count while taking bexarotene and IFN. This treatment regimen produces a response rate of 70%, with complete responses seen in 10%. If patients do not respond, denileukin diftitox may be considered as the next-line therapy and, if that treatment fails, other targeted therapies or experimental agents such as HDAC inhibitors may be tried.
Targeted Therapies
Denileukin diftitox is the first of the targeted therapies that has become available. Others include monoclonal antibodies to tumor targets and small molecule inhibitors. These agents are effective as monotherapies, but they also may prove to accelerate patients' time to response if they are combined with other drugs. However, at present it is unclear whether they produce sustained responses as monotherapies or whether they are best combined with other agents. In addition, the emergence of resistance through an immune response or mutations has been seen with some agents, for example in the treatment of chronic myelogenous leukemia with imatinib mesylate (Gleevec).
Alemtuzumab
Alemtuzumab (CamPath) is a monoclonal antibody to CD52, a molecule expressed on both B and T cells. It is active in T-cell malignancies including MF,[46] and may be less toxic when administered subcutaneously. This antibody results in suppressed B- and T-cell numbers, and has been associated with a 67% incidence of cytomegalovirus reactivation in one study in patients with lymphoproliferative disorders.[47]
HuMax-CD4
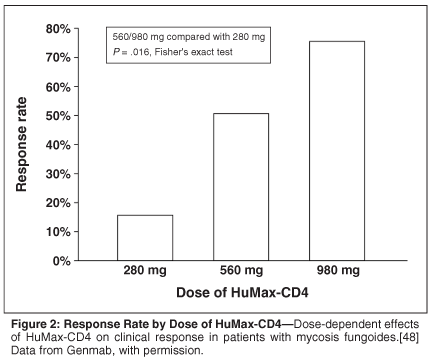
HuMax-CD4 is a monoclonal antibody to CD4. It inhibits signal transduction, cytokine production, and surface-marker expression, and down-modulates CD4 expression. It has been studied in two phase II trials in Europe and the United States that demonstrated dose-dependent responses. Among patients at mixed disease stages of MF, there was a 15% response rate (3/20 patients, with one complete response) at a dose of 280 mg, a 50% response rate (7/14 patients, two complete responses) at 560 mg, and partial response in three of four patients with advanced disease at a dose of 980 mg (Figure 2).[48] A maximal trough serum concentration of HuMax-CD4 > 10 µg/mL was associated with a clinical response. Patients' CD4+ cell counts were reduced, and this reduction was prolonged to at least 24 months in some patients. This, again, was a dose-dependent effect. Further studies to define the optimal dose of this agent are warranted.
HDAC Inhibitors
A number of HDAC inhibitors are currently in development.[49] Suberoylanilide hydroxamic acid, or vorinostat, was approved in 2006 for treatment of cutaneous manifestations in patients with CTCL who have progressive, persistent, or recurrent disease on or following two systemic therapies. Vorinostat is a very small molecule (molecular weight < 300) that binds to the active site on HDAC. In vitro, it blocks proliferation of cultured cancer cells and inhibits tumor growth in xenograft animal models. Our laboratory has demonstrated that vorinostat causes T-cell apoptosis and downregulates Stat 6 in CTCL lines, and has selectivity for malignant SS cells.[26] When given to 37 heavily pretreated CTCL patients, vorinostat produced an overall response rate of 24%.[50]
The dosing regimen may be important, as vorinostat has a short half-life. Intermittent dosing was less effective than sustained dosing at 400 mg/d. At the high dose of 600 mg/d for 2 weeks, patients with hematologic malignancies experienced myelotoxicity-particularly dose-limiting thrombocytopenia.[51] The onset of action was faster and duration of response was shorter (3 to 24 weeks) in comparison with bexarotene. It is therefore possible that a combination of these two drugs would provide both a rapid response and maintained efficacy. Furthermore, a second phase II multicenter study of vorinostat has been conducted using a dose of 400 mg/d; an overall response rate of 29% was achieved.[52]
Depsipeptide (FK228) is an HDAC inhibitor that is in phase II trials for MF/SS after demonstrating activity in phase I studies.[53] As a single agent, it has achieved a reported overall, and durable, response rate of 36% in patients with CTCL.[54] When used in combination with denileukin diftitox, depsipeptide was shown to increase expression of the IL-2 receptor and produce cumulative toxicity.[55] Other HDAC inhibitors, Trichostatin A, LAQ824, and PDX-101, are also in preclinical testing. The common side effects of the HDAC inhibitors include fatigue, gastrointestinal symptoms, change in taste, and dehydration. At higher doses, these agents also cause thrombocytopenia, low white blood cell counts, and anemia. The most worrying side effect is prolonged QT interval and electrocardiogram changes, and therefore the potential for sudden death. The cardiac effects of depsipeptide have been extensively examined in the phase II studies of this drug.[56]
As described above, it may be possible to prolong patients' treatment responses by combining HDAC inhibitors with retinoids such as bexarotene. Methylation inhibitors (5-azacytidine or decytabine) also show synergism in this combination in vitro (Zhang and Duvic, unpublished data), and could be used in combination with HDAC inhibitors. HDAC inhibitors are thought to work by increasing transcription of genes involved in tumor suppression, cell-cycle arrest, cell differentiation, and apoptosis.[26] Combination with methylation inhibitors may further help to promote this synergism. In addition, the HDAC inhibitors have direct effects on some important proteins such as p53 and other tumor suppressors.[57] Thus, these agents have many potential effects on the cell and on the disease process in CTCL.
Forodesine
Forodesine is a nucleoside analog that acts as a transition-state inhibitor. It is a small molecule that blocks the enzyme purine nucleoside phosphorylase, and hence increases cell concentrations of 2'-deoxyguanosine 5'-triphosphate. This imbalance in the nucleotide pools kills T cells. Initial efficacy data from a phase I/II study of the intravenous formulation of forodesine in 13 patients with CTCL were presented in 2005,[58] and this study has recently been completed. A phase I/II study of the oral formulation is now under way. Forodesine has the potential to reduce T cells in patients with CTCL and is reversible when the drug is withdrawn. This differentiates it from the monoclonal antibodies that may produce long-lasting T-cell depletion.
Conclusions
There are several treatment combinations currently used in CTCL (MF). Bexarotene, IFNα, and PUVA are frequently used in combination in MF. Photopheresis is used in combination with bexarotene and IFN in patients with SS. In addition, combinations of retinoids with different receptor specificities and PPAR agonists and HDAC inhibitors are attractive for clinical evaluation in trials. Denileukin diftitox can replace current chemotherapies for debulking tumors because this therapy is not associated with immunosuppression and increased risk of infection. Following such treatment, bexarotene can be given to maintain a response in those patients who are not ready to proceed to BMT. In addition, bexarotene may optimize the efficacy of denileukin diftitox by increasing CD25 expression.
Bexarotene plus gemcitabine (possibly in combination with denileukin diftitox) is another combination that may show promise for future trials. However, many potential new therapies are in development that will increase dramatically the range of possible combination treatments available. Identification of the optimal combination therapies may allow us to achieve complete, lasting responses in CTCL.
Disclosures:
Dr. Duvic is principal investigator on clinical trials, an advisory board member and speaker for Ligand, Biocryst, Merck, Genmab, and Novartis.
References:
1. Apisarnthanarax N, Talpur R, Duvic M: Treatment of cutaneous T cell lymphoma: Current status and future directions. Am J Clin Dermatol 3:193-215, 2002.
2. Cummings FJ, Kim K, Neiman RS, et al: Phase II trial of pentostatin in refractory lymphomas and cutaneous T-cell disease. J Clin Oncol 9:565-571, 1991.
3. Kurzrock R, Pilat S, Duvic M: Pentostatin therapy of T-cell lymphomas with cutaneous manifestations. J Clin Oncol 17:3117-3121, 1999.
4. Kaye FJ, Bunn PA, Jr, Steinberg SM, et al: A randomized trial comparing combination electron-beam radiation and chemotherapy with topical therapy in the initial treatment of mycosis fungoides. N Engl J Med 321:1784-1790, 1989.
5. Claudy AL, Rouchouse B, Boucheron S, et al: Treatment of cutaneous lymphoma with etretinate. Br J Dermatol 109:49-56, 1983.
6. Kessler JF, Meyskens FL, Jr, Levine N, et al: Treatment of cutaneous T-cell lymphoma (mycosis fungoides) with 13-cis-retinoic acid. Lancet 1:1345-1347, 1983.
7. Thomsen K, Molin L, Volden G, et al: 13-cis-retinoic acid effective in mycosis fungoides. A report from the Scandinavian Mycosis Fungoides Group. Acta Derm Venereol 64:563-566, 1984.
8. Fitzpatrick JE, Mellette JR: Treatment of mycosis fungoides with isotretinoin. J Dermatol Surg Oncol 12:626-629, 1986.
9. Kessler JF, Jones SE, Levine N, et al: Isotretinoin and cutaneous helper T-cell lymphoma (mycosis fungoides). Arch Dermatol 123:201-204, 1987.
10. Dreno B, Claudy A, Meynadier J, et al: The treatment of 45 patients with cutaneous T-cell lymphoma with low doses of interferon-alpha 2a and etretinate. Br J Dermatol 125:456-459, 1991.
11. Molin L, Thomsen K, Volden G, et al: Oral retinoids in mycosis fungoides and Sezary syndrome: A comparison of isotretinoin and etretinate. A study from the Scandinavian Mycosis Fungoides Group. Acta Derm Venereol 67:232-236, 1987.
12. Neely SM, Mehlmauer M, Feinstein DI: The effect of isotretinoin in six patients with cutaneous T-cell lymphoma. Arch Intern Med 147:529-531, 1987.
13. Bagot M: Treatment of cutaneous T-cell lymphoma by retinoids and calcitriol. Lancet 346:376-377, 1995.
14. French LE, Saurat JH: Treatment of cutaneous T-cell lymphoma by retinoids and calcitriol. Lancet 346:376, 1995.
15. Stadler R, Otte HG, Luger T, et al: Prospective randomized multicenter clinical trial on the use of interferon-2a plus acitretin versus interferon-2a plus PUVA in patients with cutaneous T-cell lymphoma stages I and II. Blood 92:3578-3581, 1998.
16. Duvic M, Martin AG, Kim Y, et al: Phase 2 and 3 clinical trial of oral bexarotene (Targretin capsules) for the treatment of refractory or persistent early-stage cutaneous T-cell lymphoma. Arch Dermatol 137:581-593, 2001.
17. Duvic M, Hymes K, Heald P, et al: Bexarotene is effective and safe for treatment of refractory advanced-stage cutaneous T-cell lymphoma: multinational phase II-III trial results. J Clin Oncol 19:2456-2471, 2001.
18. Breneman D, Duvic M, Kuzel T, et al: Phase 1-2 clinical trial supports the safety and efficacy of targretin topical gel, a novel RXR-selective retinoid analogue, in the treatment of cutaneous T-cell lymphoma. Blood 88:569A, 1996.
19. Porcu P, Baiocchi R, Buckner M, et al: Bexarotene-induced T-cell immunomodulation and response in CTCL. Blood 104:744, A2004.
20. Duvic M, Lemak NA, Redman JR, et al: Combined modality therapy for cutaneous T-cell lymphoma. J Am Acad Dermatol 34:1022-1029, 1996.
21. Duvic M, Apisarnthanarax N, Cohen DS, et al: Analysis of long-term outcomes of combined modality therapy for cutaneous T-cell lymphoma. J Am Acad Dermatol 49:35-49, 2003.
22. Duvic M, Talpur R, Wen S, et al: Phase II evaluation of gemcitabine monotherapy for cutaneous T-cell lymphoma. Clin Lymphoma Myeloma 7:51-58, 2006.
23. Talpur R, Ward S, Apisarnthanarax N, et al: Optimizing bexarotene therapy for cutaneous T-cell lymphoma. J Am Acad Dermatol 47:672-684, 2002.
24. Zhang C, Hazarika P, Ni X, et al: Induction of apoptosis by bexarotene in cutaneous T-cell lymphoma cells: Relevance to mechanism of therapeutic action. Clin Cancer Res 8:1234-1240, 2002.
25. Zhang C, Ni X, Konopleva M, et al: The novel synthetic oleanane triterpenoid CDDO (2-cyano-3, 12-dioxoolean-1, 9-dien-28-oic acid) induces apoptosis in Mycosis fungoides/Sezary syndrome cells. J Invest Dermatol 123:380-387, 2004.
26. Zhang C, Richon V, Ni X, et al: Selective induction of apoptosis by histone deacetylase inhibitor SAHA in cutaneous T-cell lymphoma cells: Relevance to mechanism of therapeutic action. J Invest Dermatol 125:1045-1052, 2005.
27. Straus DJ, Duvic M, Kuzel T, et al: Results of a phase II trial of oral bexarotene combined with interferon alfa-2b for patients with cutaneous T-cell lymphoma (abstract 2644). Blood 104:723a, 2004.
28. Waters CA, Schimke PA, Snider CE, et al: Interleukin 2 receptor-targeted cytotoxicity. Receptor binding requirements for entry of a diphtheria toxin-related interleukin 2 fusion protein into cells. Eur J Immunol 20:785-791, 1990.
29. Re GG, Waters C, Poisson L, et al: Interleukin 2 (IL-2) receptor expression and sensitivity to diphtheria fusion toxin DAB389IL-2 in cultured hematopoietic cells. Cancer Res 56:2590-2595, 1996.
30. Talpur R, Jones DM, Alencar AJ, et al: CD25 expression is correlated with histological grade and response to denileukin diftitox in cutaneous T-cell lymphoma. J Invest Dermatol 126:575-583, 2006.
31. Nichols J, Foss F, Kuzel TM, et al: Interleukin-2 fusion protein: An investigational therapy for interleukin-2 receptor expressing malignancies. Eur J Cancer 33(suppl 1):S34-S36, 1997.
32. Olsen E, Duvic M, Frankel A, et al: Pivotal phase III trial of two dose levels of denileukin diftitox for the treatment of cutaneous T-cell lymphoma. J Clin Oncol 19:376-388, 2001.
33. Duvic M, Kuzel TM, Olsen EA, et al: Quality-of-life improvements in cutaneous T-cell lymphoma patients treated with denileukin diftitox (ONTAK). Clin Lymphoma 2:222-228, 2002.
34. Duvic M, Cather JC, Maize J, et al: DAB389IL2 diphtheria fusion toxin produces clinical responses in tumor stage cutaneous T cell lymphoma. Am J Hematol 58:78-90, 1998.
35. Talpur R, Apisarnthanarax N, Ward S, et al: Treatment of refractory peripheral T-cell lymphoma with denileukin diftitox (ONTAK). Leuk Lymphoma 43:121-126, 2002.
36. Foss FM, Bacha P, Osann KE, et al: Biological correlates of acute hypersensitivity events with DAB389IL-2 (denileukin diftitox, ONTAK) in cutaneous T-cell lymphoma: Decreased frequency and severity with steroid premedications. Clin Lymphoma 1:298-302, 2001.
37. Ghori F, Polder KD, Pinter-Brown LC, et al: Thyrotoxicosis after denileukin diftitox therapy in patients with mycosis fungoides.
J Clin Endocrinol Metab 91:2205-2208, 2006.
38. Foss F, Demierre MF, DiVenuti G: A phase-1 trial of bexarotene and denileukin diftitox in patients with relapsed or refractory cutaneous T-cell lymphoma. Blood 106:454-457, 2005.
39. Talpur R, Duvic M: Treatment of mycosis fungoides with denileukin diftitox and oral bexarotene. Clin Lymphoma Myeloma 6:488-492, 2006.
40. Bunn PA, Jr, Hoffman SJ, Norris D, et al: Systemic therapy of cutaneous T-cell lymphomas (mycosis fungoides and the Sezary syndrome). Ann Intern Med 121:592-602, 1994.
41. Zinzani PL, Baliva G, Magagnoli M, et al: Gemcitabine treatment in pretreated cutaneous T-cell lymphoma: Experience in 44 patients. J Clin Oncol 18:2603-2606, 2000.
42. Marchi E, Alinari L, Tani M, et al: Gemcitabine as frontline treatment for cutaneous T-cell lymphoma: Phase II study of 32 patients. Cancer 104:2437-2441, 2005.
43. Wollina U, Graefe T, Karte K: Treatment of relapsing or recalcitrant cutaneous T-cell lymphoma with pegylated liposomal doxorubicin. J Am Acad Dermatol 42:40-46, 2000.
44. Talpur R, Duvic M: Bexarotene gel as adjuvant therapy for mycosis fungoides and lymphomatoid papulosis lesions refractory to oral bexarotene and/or denileukin diftitox.
J Am Acad Dermatol 50(3 suppl 1):P114, 2004.
45. Richardson SK, McGinnis KS, Shapiro M, et al: Extracorporeal photopheresis and multimodality immunomodulatory therapy in the treatment of cutaneous T-cell lymphoma.
J Cutan Med Surg 7:8-12, 2003.
46. Kennedy GA, Seymour JF, Wolf M, et al: Treatment of patients with advanced mycosis fungoides and Sezary syndrome with alemtuzumab. Eur J Haematol 71:250-256, 2003.
47. Martin SI, Marty FM, Fiumara K, et al: Infectious complications associated with alemtuzumab use for lymphoproliferative disorders. Clin Infect Dis 43:16-24, 2006.
48. Kim YH, Duvic M, Knox SJ, et al: A fully human anti-CD4 antibody: Phase II trial in cutaneous T-cell lymphoma. J Am Acad Dermatol 52(3 suppl 1):P143, 2005.
49. Mei S, Ho AD, Mahlknecht U: Role of histone deacetylase inhibitors in the treatment of cancer (review). Int J Oncol 25:1509-1519, 2004.
50. Duvic M, Talpur R, Ni X, et al: Phase II trial of oral vorinostat (suberoylanilide hydroxamic acid, SAHA) for refractory cutaneous T-cell lymphoma (CTCL). Blood 7 September 2006 (e-pub ahead of print).
51. O'Connor OA, Heaney ML, Schwartz L, et al: Clinical experience with intravenous and oral formulations of the novel histone deacetylase inhibitor suberoylanilide hydroxamic acid in patients with advanced hematologic malignancies. J Clin Oncol 24:166-173, 2006.
52. Olsen E, Kim YH, Kuzel T, et al: Vorinostat (suberoylanilide hydroxamic acid, SAHA) is clinically active in advanced cutaneous T-cell lymphoma (CTCL): Results of a phase IIb trial (abstract 7500). J Clin Oncol 24(suppl 18S):422s, 2006.
53. Sandor V, Bakke S, Robey RW, et al: Phase I trial of the histone deacetylase inhibitor, depsipeptide (FR901228, NSC 630176), in patients with refractory neoplasms. Clin Cancer Res 8:718-728, 2002.
54. Piekarz R, Bates S: A review of depsipeptide and other histone deacetylase inhibitors in clinical trials. Curr Pharm Des 10:2289-2298, 2004.
55. Piekarz RL, Robey RW, Zhan Z, et al: T-cell lymphoma as a model for the use of histone deacetylase inhibitors in cancer therapy: Impact of depsipeptide on molecular markers, therapeutic targets, and mechanisms of resistance. Blood 103:4636-4643, 2004.
56. Piekarz RL, Frye AR, Wright JJ, et al: Cardiac studies in patients treated with depsipeptide, FK228, in a phase II trial for
T-cell lymphoma. Clin Cancer Res 12:3762-3773, 2006.
57. Bhalla KN: Epigenetic and chromatin modifiers as targeted therapy of hematologic malignancies. J Clin Oncol 23:3971-3993, 2005.
58. Duvic M, Breneman D, Cooper M, et al: Phase I/II study of oral fosodine, a PNP inhibitor in refractory cutaneous T-cell lymphoma patients (abstract 2683). Blood 106:753a, 2005.