Chemotherapy for Non–Small-Cell Lung Cancer, Part I
Non–small-cell lung cancer (NSCLC) accounts for approximately80% of all lung tumors. Patients diagnosed with early-stage diseasegenerally undergo surgery, but up to 50% develop local or distantrecurrences. The benefit of chemotherapy in this disease is modest, butnew drugs and combined strategies offer hope of improved survivalrates. Because the disease recurs outside the chest in 70% of cases, oneof the foremost goals of therapy is to prevent distant dissemination. Tothis end, chemotherapy may be administered preoperatively or afterresection of the tumor. The first part of this article, which concludesnext month, will address adjuvant and neoadjuvant chemotherapy inearly-stage non–small-cell lung cancer.
ABSTRACT: Non-small-cell lung cancer (NSCLC) accounts for approximately 80% of all lung tumors. Patients diagnosed with early-stage disease generally undergo surgery, but up to 50% develop local or distant recurrences. The benefit of chemotherapy in this disease is modest, but new drugs and combined strategies offer hope of improved survival rates. Because the disease recurs outside the chest in 70% of cases, one of the foremost goals of therapy is to prevent distant dissemination. To this end, chemotherapy may be administered preoperatively or after resection of the tumor. The first part of this article, which concludes next month, will address adjuvant and neoadjuvant chemotherapy in early-stage non-small-cell lung cancer.
Lung cancer remains a major public health problem, accounting for more than 1 million new cases per year worldwide.[1] In the United States, lung cancer is the third most common malignancy after prostate and breast cancer, and the leading cause of cancer death in both men and women.[2] In Eastern Europe, lung cancer is the most frequent cause of cancer-related mortality among men and the third among women. Mortality rates in women are rising, due to the increasing use of tobacco.[3] Despite advances in surgical and nonsurgical therapy, overall 5-year survival rates have only increased modestly over the last 25 years, remaining at approximately 14%.[4]
Non-small-cell lung cancer (NSCLC) accounts for approximately 80% of all lung tumors. For earlystage disease, surgery remains the most common treatment and can be considered curative. However, only 20% to 30% of all patients with NSCLC are diagnosed at an early stage, and up to 50% of these patients will develop local or distant recurrences. The prognosis of patients with clinical stage IIIA or IIIB disease (ie, with radiologically documented involvement of the mediastinum or a technically unresectable tumor) continues to be poor, with 5-year survival rates ranging from 5% to 10% and median survivals from 12 to 15 months.
The outcome of untreated patients with advanced NSCLC is predictable: The median survival is 4 months, and the 1-year survival rate ranges from 10% to 15%. The role of chemotherapy in this disease is generally modest, but new drugs and combined strategies offer hope of improved survival rates in the near future. In this two-part article, which concludes next month, we review the role of chemotherapy in the various presentations of NSCLC.
Early-Stage Disease
Surgery remains the primary curative treatment for patients with early- stage NSCLC, ie, stage I, II, and minimal IIIa. Nevertheless, approximately half of these patients will die of tumor progression after complete surgical resection. Because the disease recurs outside the chest in 70% of cases, one of the foremost goals of therapy is the development of systemic treatments-mainly chemotherapy- to prevent distant dissemination. Chemotherapy may be administered preoperatively or after resection of the tumor.
Adjuvant Treatment
• Radiation-The first adjuvant treament explored after complete resection of lung tumors was radiation. Several trials have compared surgery alone to surgery plus postoperative radiotherapy, and a meta-analysis of those trials-the postoperative radiotherapy (PORT) meta-analysis, which included 2,128 patients-was recently reported.[5] Results show the significantly detrimental effect of postoperative radiotherapy on survival with an absolute reduction at 2 years of 7%. However, a subgroup analysis suggests that this effect occurs mainly in patients with N0/1 disease, whereas there is no evidence of a detrimental effect in patients with N2 disease.
The results of this meta-analysis should be considered with caution, as many patients were treated with equipment, doses, and irradiation fields that are now considered suboptimal. In addition, there are insufficient data on mediastinal lymph node dissection, and the surgical procedure differed among studies and centers. Thus, the role of radiotherapy in patients with N2 disease remains unclear, and new randomized studies are necessary to clarify its impact on local control and the survival of patients with resected N2 disease.
• Chemotherapy-The role of adjuvant chemotherapy has been highly controversial for years: The first chemotherapeutic agents studied in the postoperative setting, alone or in combination, were alkylating agents. From 1980 on, most trials used cisplatin- containing chemotherapy regimens, and the most well-known were those conducted by the Lung Cancer Study Group.
Holmes et al[6] reported the first efficacy trial of postoperative chemotherapy in patients who had undergone complete resection for stage II/III NSCLC. Participants were randomized to either four cycles of adjuvant CAP (cyclophosphamide [Cytoxan, Neosar], doxorubicin [Adriamycin], cisplatin [Platinol]) or immunotherapy with bacillus Calmette- Gurin (BCG). The median recurrence- free period was significantly longer for the chemotherapy group (7 months), and a survival benefit was demonstrated for adjuvant chemotherapy vs immunotherapy, but the difference was not statistically significant significant (P = .078). In a second study, adjuvant CAP chemotherapy did not improve survival compared with surgery alone in patients with stage I NSCLC, but this lack of efficacy could be explained by the suboptimal chemotherapy regimen.[7]
TABLE 1

Randomized Trials of Platinum-Based Postoperative Chemotherapy
A survival benefit was reported by Niiranen et al in patients with T1-3, N0 tumors treated with adjuvant CAP chemotherapy. The 5-year survival rate increased from 56% to 67% (P = .05) in the group that received adjuvant therapy compared to those who underwent surgery alone.[8] Wada et al found the 5-year survival rate increased from 49% to 61% with the use of postoperative cisplatin/vindesine/UFT (uracil and tegafur) chemotherapy in patients with completely resected stage I-III NSCLC (P = .04).[9] In another Japanese study, VP (vindesine/platinum) was reported to be more effective than CAP in the treatment of resected stage IIIA patients, but there was no difference in recurrence-free or overall survival between untreated patients and those in the VP group.[10] Several other studies also reported negative results. The main platinumbased randomized trials are summarized in Table 1.[6-10]
• Meta-Analysis of Cumulative Data-Given the limited number of patients enrolled in these and other trials, it was not possible to clearly establish the role of adjuvant chemotherapy in early-stage NSCLC. Therefore, the Medical Research Council (MRC) and Institut Gustave-Roussy (IGR) conducted a large meta-analysis using updated data.[11] More than 9,000 patients from 52 randomized trials fulfilled the selection criteria. The group comparing surgery alone to surgery followed by adjuvant chemotherapy encompassed 14 trials, with an overall accrual of 4,357 patients (2,574 of whom died).
The results of the five trials that used long-term alkylating agents (2,145 patients, 1,670 deaths) showed a 15% increase in the risk of death, which corresponds to a 5% absolute negative effect of chemotherapy on survival at 5 years (P = .005). In the eight trials that used a cisplatin-based regimen (1,394 patients, 614 deaths), the risk of death was reduced by 13%, suggesting an absolute benefit of 5% with adjuvant chemotherapy at 5 years (P = .08). The group comparing surgery and radiotherapy to surgery, radiotherapy, and chemotherapy included 807 patients, 619 of whom died. Cisplatin-based chemotherapy provided a 6% reduction in the risk of death, suggesting a 2% absolute benefit at 5 years. Sex, performance status, age, and histologic subtype had no impact on the effect of chemotherapy.
Even if the potential advantage of adjuvant chemotherapy in NSCLC is small, the high incidence of the disease would translate this benefit into a prolongation of life for more than 10,000 patients worldwide each year. The findings of the above trials provided the rationale for several large-scale trials of cisplatin-based regimens in the late 1990s.
• Intergroup Trial 0115-The North American Intergroup Trial INT-0115 is the only recent adjuvant trial that has already been published.[ 12] It was designed to determine whether a combination of four cycles of chemotherapy with cisplatin at 60 mg/m2 on day 1 and etoposide at 120 mg/m2 on days 1 to 3 every 28 days, plus concomitant thoracic radiotherapy to a total dose of 50.4 Gy delivered in 28 daily fractions, was superior to radiotherapy alone given at the same dose.
A total of 488 patients with stage II/IIIA NSCLC from 121 centers were randomized. All patients underwent either systemic sampling or complete dissection of mediastinal lymph nodes. The results failed to show any advantage for adjuvant chemotherapy plus radiotherapy over radiotherapy alone in preventing local recurrences or increasing survival. A recurrence was documented in 56% of patients who received chemotherapy plus radiotherapy and in 53% of patients who received radiotherapy alone.
The rate of intrathoracic recurrences within the radiotherapy field was 12% for the combined treatment group vs 13 % for the adjuvant radiotherapy alone treatment group (P = .84). The pattern of recurrences and the median time to recurrence were not significantly different in the two groups. Median survival also did not differ significantly between groups (39 months with chemotherapy and radiotherapy vs 38 months with radiotherapy alone [P = .56]).
In a multivariate analysis, the factors that significantly influenced overall survival were the extent of lymph node involvement, the type of lymph node dissection, the histologic subtype, and the patient's gender. The side effects of treatment were more common and severe in the chemoradiotherapy arm. An analysis of the impact of K-ras and p53 on the activity of chemotherapy also failed to demonstrate any interaction between overexpression of these genes and efficacy of treatment.[13] The lack of a significant difference in survival rates in this study may be due to the chemotherapy regimen used, as cisplatin was given at a low dose (60 mg/m2) concomitantly with radiotherapy. Even if the combination of cisplatin and etoposide is not the most effective regimen in NSCLC, this study demonstrated that it is easily administered concurrently with radiotherapy.
• Adjuvant Lung Project Italy Trial-Among the adjuvant studies recently completed, the Adjuvant Lung Project Italy (ALPI) trial aimed to assess the effectiveness of adjuvant chemotherapy, with or without radiotherapy.[14] It was initiated in 1994 with the participation of 66 Italian centers and 5 from the European Organization for Research and Treatment of Cancer (EORTC). The study was coordinated by the Laboratory of Cancer Clinical Research at the Mario Negri Institute in Milan.
After surgery, patients with stage I, II, and IIIa NSCLC were randomized to receive either three courses of MVP (mitomycin [Mutamycin], 8 mg/m2 on day 1; vindesine, 3 mg/m2 on days 1 and 8; cisplatin, 100 mg/m2 on day 1, every 3 weeks for three cycles) or no adjuvant treatment. Patient referral to radiotherapy was left to the discretion of the participating centers and, if given, thoracic irradiation (50 to 54 Gy over 5 to 6 weeks) was initiated after completion of chemotherapy.
Overall, 1,209 patients were enrolled in the study between January 1994 and February 1998. A total of 602 patients were randomized to chemotherapy and 594 to the control group; 13 patients were excluded from the analysis due to protocol violations. Radiotherapy was delivered in 482 patients, of whom 5% were stage I, 45% stage II, and 50% stage IIIa. (These data were obtained from Dr. Scagliotti's slide presentation at the American Society of Clinical Oncology [ASCO] website.)
Of the 327 evaluable patients (69%) who completed chemotherapy, 166 required modification of the planned regimen and 100 (21%) discontinued treatment, mainly due to toxicity. Overall, 127 (30%) and 79 (18%) patients receiving chemotherapy, respectively, experienced grade 3 and 4 toxicity, and 47 patients never started chemotherapy. Results were presented at the 2002 ASCO meeting.[14]
• Ongoing and Recently Completed Trials-The International Adjuvant Lung Cancer Trial (IALT) was a randomized study designed to determine the impact on overall survival of a chemotherapy regimen including cisplatin and either a vinca alkaloid or etoposide vs no chemotherapy after complete surgical resection in patients with stage I, II, or III NSCLC. The total dose of cisplatin in this trial was 300 to 400 mg/m2 administered in three or four cycles of 80 to 120 mg/m2. The vinca alkaloid was either vindesine at 3 mg/m2/wk, vinblastine at 4 mg/m2/wk, or vinorelbine (Navelbine) at 30 mg/m2/wk, given up to the last dose of cisplatin. The dose of etoposide was 100 mg/m2/d for 3 consecutive days every 3 to 4 weeks with cisplatin. Thoracic radiotherapy was given according to the preregistration policy of each center. A total of 1,867 patients were enrolled in the study, and the results will be presented at the next ASCO meeting in Chicago.
In the Adjuvant Navelbine International Trial Association (ANITA1) study, which is also evaluating treatment of patients with completely resected NSCLC, chemotherapy consists of four cycles of cisplatin at 100 mg/m2 every 4 weeks and 16 cycles of vinorelbine at 30 mg/m2/wk compared to a control arm. The trial enrolled 831 patients between October 1994 and December 2000. At the same time, the ANITA2 trial was initiated for patients who were unable to receive cisplatin and were instead randomized to either vinorelbine alone (30 mg/m2/wk for a total of 16 administrations) or the control arm.
The National Cancer Institute of Canada recently completed accrual of 482 patients into a phase III trial comparing surgery alone to surgery followed by adjuvant chemotherapy with cisplatin and vinorelbine in patients with stage T1/2, N0/1 disease. The Cancer and Leukemia Group B (CALGB) is also sponsoring an intergroup study (CALGB 9633) in patients with high-risk stage I NSCLC randomized to surgery alone or surgery followed by treatment with carboplatin (Paraplatin)/paclitaxel. Finally, adjuvant chemotherapy is part of the Big Lung Trial led by the MRC; 481 patients were included in the corresponding subgroup.
In conclusion, randomized postoperative chemotherapy trials have to date provided inconclusive results and have failed to demonstrate a significant benefit in survival. The results and an overview of all recently completed studies will clarify the role of chemotherapy after complete resection of early-stage NSCLC. Notably, there have been no published results of studies using recent cytotoxic or cytostatic agents as adjuvant chemotherapy in patients with early-stage NSCLC. Parameters such as angiogenesis, expression of oncogenes, mutations in tumorsuppressor genes, and presence of a drug-resistance mechanism might be taken into consideration in future protocols.
Neoadjuvant Treatment
The theoretical advantages of preoperative treatment include systemic and local effects such as early control of distant micrometastatic disease, prevention of viable tumor seeding at the time of surgery, increased resectability of neoplastic lesions that are technically unresectable at the time of diagnosis (or reduction of tumor mass before definitive sur- gery), decreased incidence of positive margins at the time of surgery, possible use of less radical surgery with organ preservation, and "in vivo" assessment of the effects of chemotherapy and radiotherapy. Drawbacks of this approach include the lack of pathologic staging, the small size of the specimen on which an entire strategy is based (for what may be a bulky and heterogeneous tumor), and the delay in realizing the curative procedure.
The role of preoperative radiotherapy was explored in the 1970s, and some phase II trials reported encouraging results. Two large randomized studies conducted in North America, however, did not show any benefit compared to surgery alone,[15,16] and preoperative radiotherapy was no longer considered for early-stage NSCLC.
TABLE 2

Randomized Studies of Neoadjuvant Chemotherapy Followed by Surgery vs Surgery Alone for Patients With Non-Small-Cell Lung Cancer
• Front-Line Chemotherapy-The role of front-line chemotherapy, with or without radiotherapy, before surgical resection in NSCLC is greatly debated in the setting of stage I, II, and minimal IIIA disease, because surgery is still considered standard treatment. Although there are few published randomized trials in stage I and II disease, many have been conducted in stage IIIA disease. With surgery alone, the 5-year survival rate of stage IIIA NSCLC patients ranges from 10% to 30%, and the median survival is 15 months.
Martini et al reported the feasibility of preoperative chemotherapy in a retrospective study in 136 patients with stage IIIA (N2) disease.[17] They observed a high response rate of 77% and an improvement in 5-year survival of 17% compared to historical controls. Since then, several published phase II trials have demonstrated a possible advantage for preoperative chemotherapy compared to historical controls, particularly for stage IIIA patients.
In 1994, two randomized studies conducted in patients with stage IIIA disease reported that preoperative cisplatin- based chemotherapy significantly improved survival compared to surgery alone or surgery combined with radiotherapy.[18,19] Both studies were closed prematurely after each had enrolled 60 patients because interim analyses indicated a survival advantage for the chemotherapy arm. More recently, the results of these studies have been updated and long-term survival rates reported (Table 2).[20-22]
In the M. D. Anderson study, the 5-year survival was 36% in the combined-modality arm vs 15% in the surgery-alone arm, but the difference was not statistically significant (P = .056).[20] In the Spanish study, there was a significant improvement in median survival in the neoadjuvant chemotherapy arm compared to the surgery-alone arm (22 vs 10 months, P = .005), and the overall 5-year survival was also significantly better in the chemotherapy arm (17% vs 0%).[21]
These studies were too small for conclusions to be drawn, with only 30 patients in each arm and poor survival in the control arms. Moreover, both studies have been criticized for the absence of systematic mediastinoscopy. Accurate assessement of mediastinal lymph nodes is an important issue in neoadjuvant strategies.
• MIP Regimen-From 1991 to 1997, a French multicenter randomized trial enrolled 373 patients, and the results were reported recently.[22] Eligible patients had stage I (except T1, N0), II, or IIIA resectable NSCLC. Preoperative chemotherapy consisted of two cycles of MIP (mitomycin, 6 mg/m2 on day 1; ifosfamide [Ifex], 1.5 g/m2 on days 1 to 3; cisplatin, 30 mg/m2 on days 1 to 3) every 3 weeks, administered before radical surgery in the experimental arm vs surgery alone in the control arm. Patients who responded to induction chemotherapy received two additional postoperative cycles of chemotherapy. Patients with pT3 and/or pN2 disease received postoperative thoracic radiotherapy to a total dose of 60 Gy delivered over 6 weeks.
TABLE 3
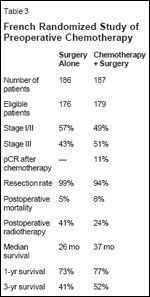
French Randomized Study of Preoperative Chemotherapy
The main results of the study are summarized in Table 3.[22] After induction chemotherapy, 11% of patients achieved a pathologic complete response. Postoperative mortality was 8% in the investigational arm and 5% in the control arm. Median survival was 37 months in the combined- therapy group vs 27 months in the control group (P = .11). The 1- and 3-year survival rates were 77% and 52% in the investigational arm vs 73% and 41% in the control arm (P = .09). Disease-free survival was significantly longer in the investigational arm (P = .02). A subgroup analysis showed that the benefit was mainly seen among patients with N0/1 disease (P = .008).
The survival advantage may have been overshadowed by perioperative toxicity, which was due, in part, to the choice of drugs. Because mediastinoscopy was not performed systematically, most patients did not undergo mediastinal pathologic staging prior to study entry. Thus, to date, no definitive trial supports induction chemotherapy before surgical resection as a standard of care.
French investigators conducted a retrospective analysis of 702 resected patients with N2 NSCLC.[23] At a median follow-up of 52 months, they found a benefit in patients who received neoadjuvant chemotherapy compared to those who did not receive preoperative treatment.
• Newer Combination Therapies-North American investigators recently studied a new drug combination in a prospective multicenter phase II trial. Conducted on behalf of the Bimodality Lung Oncology Team (BLOT), this study included 94 patients with stage I, II, and IIIA NSCLC.[24] It showed that two cycles of induction chemotherapy with paclitaxel at 225 mg/m2 and carboplatin at an area under the concentration-time curve (AUC) of 6 every 21 days before surgery, combined with three cycles of the same chemotherapy after surgery, was feasible with an acceptable toxicity.
Grade 3/4 neutropenia was reported in 35% of patients, grade 3 myalgia and arthralgia in 5% of patients, and grade 3/4 hypersensitivity due to paclitaxel in 3 patients. The objective response rate was 56% after induction chemotherapy, and 86% of patients underwent a complete resection. The 2-year survival rate was 56%. These results are encouraging, and worldwide phase III studies comparing surgery alone to neoadjuvant chemotherapy followed by surgery are ongoing.
Other drug combinations have also been evaluated in the neoadjuvant setting.[25] A phase II study (EORTC 08955) examined the feasibility and activity of preoperative GC (gemcitabine [Gemzar] at 1,000 mg/m2 on days 1, 8, and 15 combined with cisplatin at 100 mg/m2 on day 2 every 4 weeks) in 47 patients with stage IIIA (N2) NSCLC.[26] Mediastinoscopy was mandatory in this study. The main toxicity was hematologic, with 46% grade 3/4 thrombocytopenia, 14.9% grade 3/4 anemia, and 38.3% grade 3/4 neutropenia; four patients had grade 3/4 neurotoxicity, mainly ototoxicity. Three cycles of chemotherapy were administered to 38 patients, and 9 patients did not receive the complete treatment because of toxicity.
REFERENCE GUIDE
Therapeutic Agents
Mentioned in This Article
Bacillus Calmette-Gurin (BCG)
Carboplatin (Paraplatin)
Cisplatin
Cyclophosphamide
(Cytoxan, Neosar)
Doxorubicin
Etoposide
Gemcitabine (Gemzar)
Ifosfamide (Ifex)
Mitomycin (Mutamycin)
Paclitaxel
UFT (uracil and tegafur)
Vinblastine
Vindesine
Vinorelbine (Navelbine)
Brand names are listed in parentheses only if a drug is not available generically and is marketed as no more than two trademarked or registered products. More familiar alternative generic designations may also be included parenthetically.
The overall response rate in this study was high (70.2%). Among the 38 patients who received the planned induction therapy, 33 had an objective response, including 3 complete remissions and 30 partial remissions. Patients with partial responses were randomized to additional treatment- either surgery or radiotherapy. Among the patients randomized to surgery, 71% underwent a complete resection. After induction therapy, the mediastinal lymph nodes were tumorfree in 53% of cases. Median survival was 18.9 months, and the estimated 1-year survival was 69%. These data clearly show that GC is highly active in patients with stage IIIA (N2) NSCLC.
The results of EORTC 08955 were compared to those reported by the Southwest Oncology Group (SWOG) for trial 8805, which evaluated concurrent chemoradiotherapy (two cycles of cisplatin and etoposide combined with thoracic radiotherapy at 45 Gy) followed by surgery in patients with stage IIIA (N2) and IIIB NSCLC.[27] The percentage of complete resections (71%) was identical in both studies, and the median survival was 18.9 months in EORTC 08955 vs 15 months in SWOG 8805.
This phase II study focused attention on the role of radiotherapy in neoadjuvant strategies, at least for patients with a marginally operable tumor. Several other encouraging phase II studies of presurgical chemoradiotherapy have been reported, and a large German study is ongoing in stage III NSCLC patients.[28]
In part 2 of this article, which will appear in the April issue of ONCOLOGY, Drs. Novello and LeChavalier will address the treatment of locally advanced and advanced non-small-cell lung cancer, including the use of novel agents such as pemetrexed and tirapazamine, considerations in elderly patients, and the issue of second-line chemotherapy.
Disclosures:
The author(s) have no significant financial interest or other relationship with the manufacturers of any products or providers of any service mentioned in this article.
References:
1. Parkin DM, Pisani P, Ferlay J: Globalcancer statistics. CA Cancer J Clin 49:33-64, 1,1999.
2. Jemal A, Thomas A, Murray T, et al:Cancer statistics, 2002. CA Cancer J Clin 52:23-47, 2002.
3. Levi F, Lucchini F, Negri E, et al: Cancermortality in Europe, 1990-1994, and an overviewof trends from 1955 to 1994. Eur J Cancer35:1477-1516, 1999.
4. Wingo P, Ries L, Rosenberg HM, et al:Cancer incidence and mortality, 1973-1995: Areport card for the US. Cancer 82:1197-1207,1998.
5. PORT Meta-analysis Trialists Group:Postoperative radiotherapy in non-small-celllung cancer: Systematic review and meta-analysisof individual patient data from nine randomisedcontrolled trials. Lancet 352:257-263,1998.
6. Holmes EC, Gail M: Surgical adjuvanttherapy for stage II and stage III adenocarcinomaand large cell undifferentiated carcinoma. JClin Oncol 4:710-715, 1986.
7. Feld R, Rubinstein L, Thomas PA: Adjuvantchemotherapy with cyclophosphamide,doxorubicin, and cisplatin in patients with completelyresected stage I non-small-cell lung cancer.The Lung Cancer Study Group. J NatlCancer Inst 85:299-306, 1993.
8. Niiranen A, Niitamo-Korhonen S, KouriM, et al: Adjuvant chemotherapy after radicalsurgery for non-small-cell lung cancer: A randomisedstudy. J Clin Oncol 10:1927-1932,1992.
9. Wada H, Hitomi S, Teramatsu T: Adjuvantchemotherapy after complete resection innon-small-cell lung cancer. West Japan StudyGroup for Lung Cancer Surgery. J Clin Oncol14:1048-1054, 1996.
10. Ohta M, Tsuchiya R, Shimoyama M, etal: Adjuvant chemotherapy for completely resectedstage III non-small-cell lung cancer. TheJapan Clinical Oncology Group. J Thorac CardiovascSurg 106:703-708, 1993.
11. Non-Small Cell Lung Cancer CollaborativeGroup: Chemotherapy in non-small celllung cancer: A meta-analysis using updateddata on individual patients from 52 randomizedclinical trials. Br Med J 311:899-909,1995.
12. Keller SM, Adak S, Wagner H, et al: Arandomized trial of postoperative adjuvant therapyin patients with completely resected stageII or IIIA non-small-cell lung cancer. EasternCooperative Oncology Group. N Engl J Med343:1217-1222, 2000.
13. Schiller J, Adak S, Feins RH, et al: Lackof prognostic significance of p53 and K-ras mutations in primary resected non-small-cell lung cancer on E4592: ALaboratory Ancillary Study on an Eastern Cooperative Oncology GroupProspective Randomised Trial of Postoperative Adjuvant Therapy. JClin Oncol 19:448-457, 2001.
14. Tonato M, on behalf of the ALPI/EORTC-LCG investigators:Final report of the Adjuvant Lung Project Italy (ALPI): An Italian/EORTC-LCG randomised trial of adjuvant chemotherapy in completelyresected non-small cell lung cancer (NSCLC) (abstract 1157). ProcAm Soc Clin Oncol 21:290a, 2002.
15. Shields T, Higgins GA Jr, Lawton R, et al: Preoperative x-raytherapy as an adjuvant in the treatment of bronchogenic carcinoma. JThorac Cardiovasc Surg 59:49-61, 1970.
16. Warram J: Preoperative irradiation of cancer of the lung: Finalreport of a therapeutic trial. Cancer 36:914-925, 1975.17. Martini N, Kris MG, Flehinger BJ, et al: Preoperative chemotherapyfor stage IIIa (N2) lung cancer: The Sloan-Kettering experiencewith 136 patients. Ann Thorac Surg 55:1365-1373, 1993.
18. Rosell R, Gomez-Codina J, Camps C, et al: A randomized trialcomparing preoperative chemotherapy plus surgery with surgery alonein patients with non-small-cell lung cancer. N Engl J Med 330:153-158,1994.
19. Roth JA, Fossella F, Komaki R, et al: A randomized trial comparingperioperative chemotherapy and surgery with surgery alone inresectable stage IIIA non-small-cell lung cancer. J Natl Cancer Inst86:673-680, 1994.
20. Roth JA, Atkinson EN, Fossella F, et al: Long-term follow-up ofpatients enrolled in a randomised trial comparing perioperative chemotherapyand surgery with surgery alone in resectable stage IIIA nonsmall-cell lung cancer. Lung Cancer 21:1-6, 1998.
21. Rosell R, Gomez-Godina J, Camps C, et al: Preresectional chemotherapyin stage IIIA non-small-cell lung cancer: A 7-year assessmentof a randomised controlled trial. Lung Cancer 26:7-14, 1999.
22. Depierre A, Milleron B, Moro-Sibilot D, et al: Preoperativechemotherapy followed by surgery compared with primary surgery inresectable stage I (except T1N0), II, and IIIa non-small-cell lung cancer.J Clin Oncol 20:247-253, 2002.
23. André F, Grunenwald D, Pignon JP, et al: Survival of patientswith resected N2 non-small cell lung cancer: Evidence for a subclassificationand implications. J Clin Oncol 18(16):2981-2989, 2000.
24. Pisters KM, Ginsberg RJ, Giroux DJ, et al: Induction chemotherapybefore surgery for early-stage lung cancer: A novel approach.Bimodality Lung Oncology Team. J Thorac Cardiovasc Surg 119:429-439, 2000.
25. Rosell R: The integration of newer agents into neoadjuvanttherapy. Semin Oncol 25:24-27, 1998.
26. Van Zandwijk N, Smit EF, Kramer GW, et al: Gemcitabine andcisplatin as induction regimen for patients with biopsy-proven stageIIIA N2 non-small-cell lung cancer: A phase II study of the EuropeanOrganization for Research and Treatment of Cancer Lung Cancer CooperativeGroup (EORTC 08955). J Clin Oncol 18:2658-2664, 2000.
27. Albain KS, Rusch VW, Crowley JJ, et al: Concurrent cisplatin/etoposide plus chest radiotherapy followed by surgery for stages IIIA(N2) and IIIB non-small-cell lung cancer: Mature results of SouthwestOncology Group phase II study 8805. J Clin Oncol 13:1880-1892,1995.
28. Thomas M, Rube M, Semik H, et al: Randomized trial ofchemotherapy (CT) and twice-daily chemoradiation (hfRT/CT) versuschemotherapy (CT) alone before surgery in stage III non-smallcell lung cancer (NSCLC): Interim analysis of toxicity (abstract 1769).Proc Am Soc Clin Oncol 18:458a, 1999.