Colorectal Cancer Patients With Oligometastatic Liver Disease: What Is the Optimal Approach?
In a good percentage of patients who have oligometastatic disease confined to a single organ-usually the liver-complete metastasectomy can result in cure. However, once the decision to pursue surgery is made, there remain a number of issues that must be addressed in order to ensure the best possible outcome.
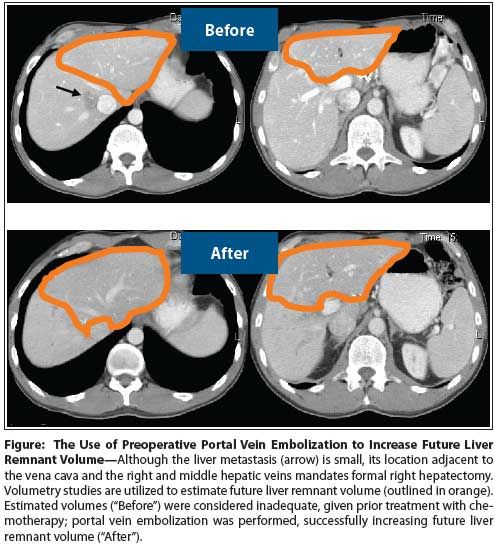
Figure: The Use of Preoperative Portal Vein Embolization to Increase Future Liver Remnant Volume
Although metastatic colorectal cancer is typically incurable, in a good percentage of patients (20% to 50%) who have oligometastatic disease confined to a single organ-usually the liver-complete metastasectomy can result in cure. However, once the decision to pursue surgery is made, there remain a number of issues that must be addressed in order to ensure the best possible outcome. These include whether to perform synchronous or staged resections of the liver metastasis and the primary colon cancer; whether surgery should be performed before, after, or in the absence of chemotherapy; if chemotherapy is used, which agents will be best; and in patients with locally advanced rectal cancer, whether pelvic radiation should be incorporated into the treatment plan. Unfortunately, there are limited data that can provide guidance in deciding these questions in a particular patient. Here we present the insights we have arrived at through our own considerable experience with this patient population, and we reflect on the relevant studies that are available.
Introduction
Metastatic colorectal cancer is typically a treatable but incurable disease. Patients with oligometastatic disease confined to a single organ, most often the liver, are a notable exception. Multiple series have now confirmed that in this setting cure is attained in 20% to 50% of patients who undergo complete metastasectomy.[1] Even in the absence of randomized trials comparing operative with nonoperative management, surgery has become standard practice for patients with resectable oligometastatic disease. On the other hand, for those with more extensive disease involving multiple organs and numerous (> 4) lesions, the value of this approach is controversial; surgery may be followed by long-term survival but is rarely curative.[2,3] Consider the hypothetical case of an asymptomatic patient with colorectal cancer and two resectable liver metastases. The issues that would need to be addressed in such a case are typical of this patient population. These include whether surgery should be performed before, after, or in the absence of chemotherapy; and whether operations for the metastases and the primary tumor should be performed at the same time. In the setting of locally advanced rectal cancer, an additional concern is the utility of pelvic radiation. There are few, if any, data to directly inform these decisions. Therefore, all recommendations are subjective and remain open to debate. In this paper we present our views and the rationale behind them.
Synchronous or Staged Surgery?
Combined resection of liver metastasis along with the primary colon cancer is often feasible and is commonly performed. The benefits of synchronous resection include less exposure to general anesthesia (one vs two operations), less morbidity, and the opportunity to eradicate all disease in one procedure. The risk associated with anesthesia varies from patient to patient and depends on comorbidity, age, and disease status. Although the risk is minor in many patients, it is additive and can be substantial in older patients. Perioperative complications are also additive, and there are fewer total complications following synchronous vs staged resections.[4] Complications are especially burdensome in patients who undergo staged resections, and these can significantly delay treatment of remaining gross disease. However, some centers advocate a more selective approach, reserving synchronous resection for patients with colon rather than rectal cancer, and for those who require more minor hepatectomy.[5,6] Our preferred approach is synchronous resection to eradicate all disease, except in the settings of high comorbidity or emergent presentation with perforation or obstruction.
It can be argued that metachronous resection should be reconsidered in the era of laparoscopy. Most colon tumors can now be removed using a minimally invasive approach, with fewer complications and rapid recovery. Although we favor synchronous resection, in the era of laparoscopy, one could argue that laparoscopic colon resection should be performed first, followed at a later date by liver resection. In some very select circumstances, the logical approach is to resect the metastases first.[7]
Preoperative disease workup for synchronous resection includes high-quality CT scans of the chest, abdomen, and pelvis, with triphasic examination of the liver. In patients with hepatic steatosis resulting from chemotherapy or other causes, liver MRI is often used, since it provides better visualization of the parenchyma. Positron emission tomography (PET) scans are not routinely obtained. Liver volumetry (calculation of the future liver remnant volume) is performed for patients being considered for extended hepatic resection; preoperative portal vein embolization can then be performed in patients with inadequate or borderline future liver remnant volumes (Figure).
Role of Nonsurgical Modalities in the Eradication of Liver Metastasis
Other modalities are available to eradicate liver metastasis; however, surgery is favored in fit patients with resectable disease.[8] In general, ablative therapies play a secondary role in patients with hepatic colorectal metastases. Thermal ablation (radiofrequency or microwave) is the technique used most commonly, and while potentially effective in select patients, it has limited application in patients with larger tumors (> 3 cm) or tumors in close proximity to major intrahepatic vascular or biliary structures or adjacent extrahepatic organs (ie, stomach, duodenum, colon). Thermal ablation is most appropriate in patients with limited disease who are poor candidates for resection, or in conjunction with resection in patients with multiple, bilobar tumors. Transcatheter arterial embolization techniques with bland or drug-eluting beads, and radioembolization with yttrium-90 are palliative therapies; these currently are not appropriate for patients who are candidates for complete surgical resection.[9,10]
Chemotherapy
The European Organisation for Research and Treatment of Cancer (EORTC) intergroup trial 40983 is the one randomized trial that directly addresses the question of the role of chemotherapy in the setting of resection of colorectal liver metastasis. Patients with 1 to 3 liver metastases deemed resectable by the evaluating surgeon were randomly assigned either to surgery, or to surgery with 3 months of preoperative and 3 months of postoperative chemotherapy.[11] The predefined endpoint was 3-year recurrence-free survival. Chemotherapy included folinic acid, 5-fluorouracil, and oxaliplatin (FOLFOX4). The surgery-and-chemotherapy group achieved a statistically significant 9% absolute improvement in 3-year recurrence-free survival compared with the surgery-alone group. Many experts contest the interpretation that this is a definitive study, since no difference in overall survival was observed. Nevertheless, chemotherapy is almost always used in conjunction with surgery in this setting.
Several important issues are not yet settled, including the course, timing, and duration of chemotherapy. The study design described above called for split-course chemotherapy. Many cancer biologists would argue that this is suboptimal, since interruption of chemotherapy before eradication of all disease may lead to the development of tumor resistance.[12] Thus, it is preferable to deliver all planned chemotherapy before or after resection. However, prolonged courses of chemotherapy are toxic to the liver. Almost all colorectal cancer–active agents are hepatotoxic and cause some degree of chemotherapy-associated steatohepatitis (CASH) and sinusoidal congestion (“blue liver”), which will increase the risk of complications at liver resection. Therefore, in the setting of resectable liver metastasis, a strong argument can be made for primary resection of all disease followed by postoperative chemotherapy. Indeed, this is the preferred approach for a fully resectable patient at our institution.
Conversion therapy vs neoadjuvant therapy
Some patients have multiple lesions or lesions in close proximity to vascular structures, such that resection would result in an insufficient liver remnant or a positive margin. The purpose of chemotherapy in this setting is to “convert” unresectable to resectable disease. Substantial tumor regression may allow for safe, margin-negative resection. In this setting, chemotherapy combinations that are active in unresectable metastatic disease are reasonable and appropriate.[13] However, patients should be evaluated frequently, typically at 2-month intervals, and surgery should be undertaken only when there has been adequate response and the disease has been rendered resectable.
Metachronous liver metastasis in previously treated patients
For patients previously treated with adjuvant oxaliplatin in combination with a fluoropyrimidine, who subsequently develop resectable liver metastasis, the issue of chemotherapy is far more controversial. Again, relevant questions include whether chemotherapy should be given before or after resection, and which agents should be used. For patients with oligometastatic liver disease (eg, two resectable lesions), the goal of chemotherapy is to prevent development of further disease following resection. We favor upfront surgery with postoperative chemotherapy, because of the chemotherapy-associated hepatotoxicity outlined above. However, a short disease-free interval between the resection of the primary lesion and the development of metastasis, and/or the presence of associated indeterminate lesions possibly indicating more advanced disease, would favor initial chemotherapy prior to surgery.
Which agents should be used? Since the disease developed after FOLFOX, one would be inclined to use other agents, such as irinotecan, bevacizumab, or cetuximab. However, it should be remembered that the intent of chemotherapy is to prevent the development of further disease by eradicating occult metastasis. Since few studies directly address the question of which agents are most effective at eradicating occult micrometastases in colorectal cancer patients with oligometastatic liver disease, it is reasonable to extrapolate from the collective experience of patients with resected stage III disease, for whom the goal of adjuvant chemotherapy is similar: to eliminate micrometastatic disease. Although irinotecan is active in unresected stage IV disease, it has failed to show benefit as adjuvant therapy in three individual trials of stage III disease.[14-16] In addition, a European randomized study showed that the addition of irinotecan to postoperative 5-fluorouracil and folinic acid offered no benefit to patients with resected stage IV disease.[17] Thus, it appears that irinotecan is ineffective in the treatment of micrometastatic disease.
What about bevacizumab? Two large studies of patients with resected stage III colorectal cancer noted no improvement in recurrence-free or overall survival with the addition of bevacizumab to oxaliplatin and fluoropyrimidine-based chemotherapy.[18,19] In the metastatic setting, a trial of 1,400 patients randomized to oxaliplatin and a fluoropyrimidine with or without bevacizumab showed no improvement in rate or degree of response, suggesting that bevacizumab does not shrink liver lesions or improve resectability.[20] Many interpret these studies as indicating that bevacizumab has no role in the pre- or postoperative management of patients with resectable liver metastases.
Similarly, there is little support for using cetuximab to treat micrometastasis. In the cooperative group study N1047, cetuximab was added to FOLFOX in patients with resected stage III colon cancer.[21] Even after the exclusion of KRAS-mutated tumors,[22] this large randomized controlled study showed no benefit in the cetuximab arm. In fact, the study revealed a significant detriment to outcomes in patients over the age of 70. For this reason, cetuximab is not considered appropriate treatment for stage III colorectal cancers and does not appear to improve outcomes in patients following complete metastasectomy. This has been substantiated by the recently reported EPOC study,[23] which randomized patients with resectable or near-resectable colorectal liver metastasis to FOLFOX, with or without cetuximab. Chemotherapy was delivered for 3 months before and 3 months after resection. The trial was halted early by the safety data monitoring board on grounds of futility, since patients in the cetuximab arm were noted to have worse progression-free survival.[24]
Locally Advanced Rectal Cancer
The treatment of patients with locally advanced rectal cancer (tumor extension through the rectal wall or involvement of locoregional lymph nodes) who also have oligometastatic, resectable liver disease is challenging. Specifically, the challenge is determining the role of pelvic radiation. In the nonmetastatic setting, pelvic radiation is standard, and evidence supports its use preoperatively. The German Rectal Cancer Study Group trial demonstrated less local recurrence and less toxicity when patients received preoperative rather than postoperative chemoradiotherapy.[25] Delivered over 5 to 6 weeks, followed by a 6- to 12-week break, radiation downsizes bulky tumor and facilitates complete R0 resection. However, surgery and systemic treatment are delayed for 3 to 5 months, which is not ideal for most patients with metastatic disease. A selective approach to pelvic radiation is generally used in patients with metastatic disease, in which chemotherapy is delivered to treat local and distant disease. FOLFOX chemotherapy is effective in downsizing primary rectal cancer.[26,27] In a retrospective study of patients treated with FOLFOX followed by surgery without radiation, 85% of rectal cancer patients achieved a greater than 90% tumor response.[27] The efficacy of a selective approach to pelvic radiation in patients with metastatic disease has been illustrated in a retrospective study of stage IV rectal cancer patients undergoing liver metastasectomy following initial systemic chemotherapy. There was no difference in local recurrence rates between those who did and those who did not receive pelvic radiation; and, as expected, distant recurrence was far more common than local recurrence in both cohorts.[28] There are alternatives to the preoperative radiotherapy regimen used in the German rectal cancer trial described above; these include the use of short-course pelvic radiotherapy delivered over 5 days before combined resection.[29] However, this approach cannot be used in the setting of bulky rectal disease, since it provides insufficient time for tumor downsizing. This has led some practitioners to add a delay following short-course radiotherapy, during which chemotherapy is given to facilitate tumor downsizing.[30] Clearly, an individualized approach is necessary in patients with metastatic disease to ensure complete resection without overtreating local disease.
Conclusions
The concept of oligometastatic disease emerged 2 decades ago, as clinicians recognized that, with judicious and appropriate treatment, patients with limited metastasis have a genuine potential for cure.[31] The prognosis for these patients lies somewhere between the prognosis for locoregional disease and that for widely metastatic disease. The patient with two resectable liver metastases is a good example. If such a patient is medically fit, surgery should be offered and chemotherapy delivered postoperatively. In a chemotherapy-naive patient, oxaliplatin-based treatment is most appropriate. If the margin of resection of either the primary lesion or the metastasis is at risk, chemotherapy should be delivered preoperatively, with frequent assessment of response. Surgery should proceed once complete resection can be achieved; prolonged courses of preoperative chemotherapy should be avoided to limit hepatotoxicity. Pelvic radiation should be considered if the radial circumferential margin remains at risk after chemotherapy. As in all tumors that require multimodal treatment, early engagement and communication among members of a multidisciplinary team that includes surgeons, medical oncologists, radiation oncologists, and other specialists are needed to facilitate treatment and optimize the chance for cure.
Disclosures:
Dr. Saltz serves as a paid consultant to Bayer, Bristol-Myers Squibb, and Roche-Genentech; and as an unpaid consultant to Sanofi-Aventis. Drs. Jarnagin and Weiser have no significant financial interest or other relationship with the manufacturers of any products or providers of any service mentioned in this article.
References:
1. House MG, Ito H, Gonen M, et al. Survival after hepatic resection for metastatic colorectal cancer: trends in outcomes for 1,600 patients during two decades at a single institution. J Am Coll Surg. 2010;210:744-52,52-5.
2. Kornprat P, Jarnagin WR, Gonen M, et al. Outcome after hepatectomy for multiple (four or more) colorectal metastases in the era of effective chemotherapy. Ann Surg Oncol. 2007;14:1151-60.â©
3. Tomlinson JS, Jarnagin WR, DeMatteo RP, et al. Actual 10-year survival after resection of colorectal liver metastases defines cure. J Clin Oncol. 2007;25:4575-80.
4. Martin R, Paty P, Fong Y, et al. Simultaneous liver and colorectal resections are safe for synchronous colorectal liver metastasis. J Am Coll Surg. 2003;197:233-41; discussion 41-2.
5. Reddy SK, Pawlik TM, Zorzi D, et al. Simultaneous resections of colorectal cancer and synchronous liver metastasis: a multi-institutional analysis. Ann Surg Oncol. 2007;14:3481-91.
6. Tzeng CS, Aloia TA, Vauthey JN, et al. Morbidity of staged proctectomy after hepatectomy for colorectal cancer: a matched case-control analysis. Ann Surg Oncol. 2013;20:482-90.
7. Poultsides GA, Servais EL, Saltz LB, et al. Outcome of primary tumor in patients with synchronous stage IV colorectal cancer receiving combination chemotherapy without surgery as initial treatment. J Clin Oncol. 2009;27:3379-84.
8. Abdalla EK, Bauer TW, Chun YS, et al. Locoregional surgical and interventional therapies for advanced colorectal cancer liver metastases: expert consensus statements. HPB (Oxford). 2013;15:119-30.
9. Gruber-Rouh T, Naguib NN, Eichler K, et al. Transarterial chemoembolization of unresectable systemic chemotherapy-refractory liver metastases from colorectal cancer: long-term results over a 10-year period. Int J Cancer. Sep 3 2013. [Epub ahead of print]
10. Nace GW, Steele JL, Amesur N, et al. Yttrium-90 radioembolization for colorectal cancer liver metastases: a single institution experience. Int J Surg Oncol. 2011;2011:571261.
11. Nordlinger B, Sorbye H, Glimelius B, et al. Perioperative chemotherapy with FOLFOX4 and surgery versus surgery alone for resectable liver metastases from colorectal cancer (EORTC Intergroup trial 40983): a randomised controlled trial. Lancet. 2008;22:1007-16.
12. Misale S, Yaeger R, Hobor S, et al. Emergence of KRAS mutations and acquired resistance to anti-EGFR therapy in colorectal cancer. Nature. 2012;486:532-6.
13. Adam R, Wicherts DA, de Haas RJ, et al. Patients with initially unresectable colorectal liver metastases: is there a possibility of cure? J Clin Oncol. 2009;27:1829-35.
14. Saltz LB, Niedzwiecki D, Hollis D, et al. Irinotecan fluorouracil plus leucovorin is not superior to fluorouracil plus leucovorin alone as adjuvant treatment for stage III colon cancer: results of CALGB 89803. J Clin Oncol. 2007;25:3456-61.
15. Ychou M, Raoul J-L, Douillard J-Y, et al. A phase III randomised trial of LV5FU2 + irinotecan versus LV5FU2 alone in adjuvant high-risk colon cancer (FNCLCC Accord02/FFCD9802). Ann Oncol. 2009;20:674-80.
16. Van Cutsem E, Labianca R, Bodoky G, et al. Randomized phase III trial comparing biweekly infusional fluorouracil/leucovorin alone or with irinotecan in the adjuvant treatment of stage III colon cancer: PETACC-3. J Clin Oncol. 2009;27:3117-25.
17. Ychou M, Hohenberger W, Thezenas S, et al. A randomized phase III study comparing adjuvant 5-fluorouracil/folinic acid with FOLFIRI in patients following complete resection of liver metastases from colorectal cancer. Ann Oncol. 2009;20:1964-70.
18. Wolmark N, Yothers G, O'Connell MJ, et al. A phase III trial comparing mFOLFOX6 to mFOLFOX6 plus bevacizumab in stage II or III carcinoma of the colon: Results of NSABP Protocol C-08. J Clin Oncol. 2009;27(suppl):abstr LBA4.
19. de Gramont A, Van Cutsem E, Schmoll H-J, et al. Bevacizumab plus oxaliplatin-based chemotherapy as adjuvant treatment for colon cancer (AVANT): a phase 3 randomised controlled trial. Lancet Oncol. 2012;13:1225-33.
20. Saltz LB, Clarke S, Diaz-Rubio E, et al. Bevacizumab in combination with oxaliplatin-based chemotherapy as first-line therapy in metastatic colorectal cancer: a randomized phase III study. J Clin Oncol. 2008;26:2013-19.
21. Alberts SR, Sargent DJ, Nair S, et al. Effects of oxaliplatin, 5-fluorouracil, and leucovorin with or without cetuximab on survival among patients with resected stage III colon cancer: a randomized trial. JAMA. 2012;307:1383-93.
22. Amado RG, Wolf M, Peeters M, et al. Wild-type KRAS is required for panitumumab efficacy in patients with metastatic colorectal cancer. J Clin Oncol. 2008;26:1626-34.
23. Efficacy evaluation of TheraSphere following failed first line chemotherapy in metastatic colorectal cancer. Available from: http://clinicaltrials.gov/show/NCT01483027. Accessed September 3, 2013.
24. Primrose J, Falk S, Finch-Jones M, et al. A randomized clinical trial of chemotherapy compared to chemotherapy in combination with cetuximab in k-RAS wild-type patients with operable metastases from colorectal cancer: the new EPOC study. J Clin Oncol. 2013;31(suppl):abstr 3504.
25. Sauer R, Becker H, Hohenberger W, et al; German Rectal Cancer Study Group. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med. 2004;351:1731-40.
26. Cercek A, Weiser MR, Goodman KA, et al. Complete pathologic response in the primary of rectal or colon cancer treated with FOLFOX without radiation. J Clin Oncol. 2010;28(suppl):abstr 3649.
27. Schrag D, Weiser MR, Goodman KA, et al. Neoadjuvant FOLFOX-bev, without radiation, for locally advanced rectal cancer. J Clin Oncol. 2010;28(suppl):abstr 434.
28. Butte JM, Gonen M, Ding P, et al. Patterns of failure in patients with early onset (synchronous) resectable liver metastases from rectal cancer. Cancer. 2012;118:5414-23.
29. Kapiteijn E, Marijnen CA, Nagtegaal ID, et al; Dutch Colorectal Cancer Group. Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer. N Engl J Med. 2001;345:638-46.
30. van Dijk TH, Tamas K, Beukema JC, et al. Evaluation of short-course radiotherapy followed by neoadjuvant bevacizumab, capecitabine, and oxaliplatin and subsequent radical surgical treatment in primary stage IV rectal cancer. Ann Oncol. 2013;24:1762-9.
31. Hellman S, Weichselbaum RR. Oligometastasis. J Clin Oncol. 1995;13:8-10.