(S021) Central Versus Peripheral Tumor Location: Influence on Survival, Local Control, and Toxicity Following Stereotactic Body Radiotherapy for Primary Non–Small-Cell Lung Cancer
The goal of this study is to compare survival, local control, and toxicity outcomes for non–small-cell lung cancer patients treated with SBRT for centrally versus peripherally located tumors.
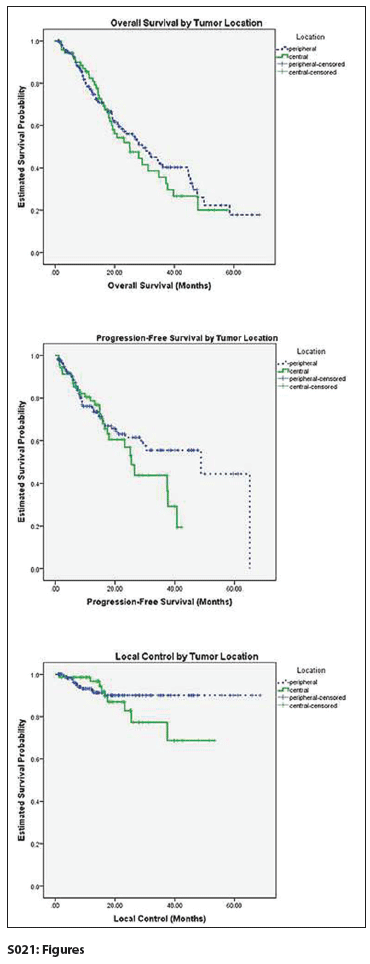
S021: Figures
Henry S. Park, MD, MPH, Eileen M. Harder, BS, Roy H. Decker, MD, PhD; Yale University School of Medicine
Background: Stereotactic body radiotherapy (SBRT) has been increasingly utilized in the management of medically inoperable non–small-cell lung cancer (NSCLC). However, there is concern that treatment of centrally located tumors could lead to increased toxicity. This has generally led to a treatment with a lower biological equivalent dose (BED) for centrally located tumors, although this could potentially be concerning for decreased local control. The goal of this study is to compare survival, local control, and toxicity outcomes for patients treated with SBRT for centrally versus peripherally located tumors.
Methods: Patients with primary NSCLC treated with SBRT at Yale-New Haven Hospital from 2007 to 2013 were included in this analysis. Central tumor location was defined as within 2 cm of the proximal bronchial tree, heart, great vessels, trachea, or other mediastinal structures. Acute toxicity was defined as occurring within 3 months of treatment, and late toxicity was defined as occurring after at least 3 months of treatment. Toxicity was defined as “severe” if graded as 3 or higher. The association of tumor location with overall survival (OS), progression-free survival (PFS), and local control (LC) was assessed with Kaplan-Meier analysis and Cox regression modeling. For evaluation of toxicity, chi-square analysis and logistic regression modeling were used. Multivariate analyses adjusted for potential covariates, including age, sex, BED, performance status, clinical versus pathologic diagnostic method, tumor histology, tumor size, and total number of targets.
Results: There were 253 patients included in this analysis (70 with central tumor location and 183 with peripheral tumor location). Median follow-up was 24.9 months. Patients with central tumors were more likely to have larger tumors (median 2.6 cm vs 1.9 cm; P < .001) and be treated with a lower BED (median 112.5 Gy vs 151.2 Gy; P < .001) compared with those with peripheral tumors. Univariate analysis revealed that tumor location was not associated with OS (52% vs 56% at 2 years; P = .56), PFS (57% vs 62% at 2 years; P = .22), LC (83% vs 90% at 2 years; P = .33), acute toxicity (23% vs 26%; P = .75), acute severe toxicity (1% vs 7%; P = .12), late toxicity (17% vs 15%; P = .70), or late severe toxicity (7% vs 3%; P = .15). After adjustment for demographic and clinical covariates in the multivariate analysis, tumor location did not predict for OS (hazard ratio [HR] = 0.88; P = .63), PFS (HR = 1.02; P = .94), LC (HR = 1.24; P = .73), acute toxicity (odds ratio [OR] = 0.74; P = .45), acute severe toxicity (OR = 0.22; P = .15), late toxicity (OR = 1.75 at 2 years; P = .17), or late severe toxicity (OR = 2.95; P = .10). BED did not predict for any of these outcomes overall or within either subgroup of tumor location.
Conclusions: Despite presenting with larger tumors and being treated with a lower BED, patients with central NSCLC who received SBRT had similar survival, local control, and toxicity outcomes compared with those with peripheral NSCLC. Greater numbers of patients and longer follow-up are needed to further characterize the expected long-term outcomes following SBRT for central NSCLC.
Proceedings of the 96th Annual Meeting of the American Radium Society - americanradiumsociety.org